PK/PD Fundamentals - Drug's Dance
- Pharmacokinetics (PK): Body's action on drug (ADME: Absorption, Distribution, Metabolism, Excretion). Governs drug concentration.
- Pharmacodynamics (PD): Drug's action on body. Mechanism, dose-response, therapeutic & adverse effects.
- Interplay: PK (concentration) drives PD (effect). Crucial for effective, safe therapy.
- Significance: Guides dose selection, regimen optimization, predicting interactions, minimizing toxicity.
- Steady state concentration ($C_{ss}$) is typically reached after 4-5 drug half-lives ($t_{1/2}$).
⭐ Achieving steady state ensures consistent therapeutic drug levels, vital for efficacy and minimizing toxicity, especially for chronic therapies.
Pharmacokinetics - ADME Adventure
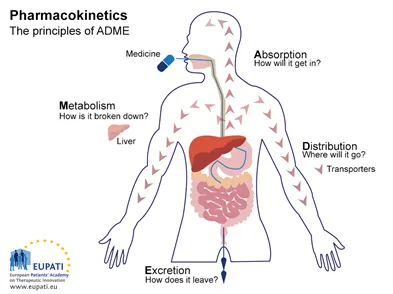
- Absorption (A): Drug entry to systemic circulation.
- Bioavailability ($F$): fraction reaching circulation; IV $F$=100%.
- First-pass metabolism (liver) ↓ oral $F$.
- pKa & pH affect absorption (📌 "Like absorbs like").
- Distribution (D): Drug spread.
- Volume of Distribution ($V_d$): $V_d = \text{Amount of drug in body} / C_p$. High $V_d$: drug in tissues. Low $V_d$: drug in plasma.
- Protein binding: unbound drug active.
- Metabolism (M): Biotransformation (liver).
- Phase I (CYP450): oxidation, reduction, hydrolysis.
- Phase II: conjugation.
- CYP Inducers (e.g., Rifampicin, 📌 "CRAP GPS"): ↓ drug effect.
- CYP Inhibitors (e.g., Macrolides, 📌 "SICKFACES.COM"): ↑ drug effect.
- Prodrugs (e.g., Levodopa): activated by metabolism.
- Excretion (E): Renal excretion.
- Clearance ($Cl$): $Cl = k \cdot V_d$.
- Half-life ($t_{1/2}$): $t_{1/2} = 0.693 / k$. 4-5 $t_{1/2}$ to $C_{ss}$/elimination.
- $C_{ss} = \text{Dose rate} / Cl$.
- Kinetics: First-order (constant fraction/time) vs. Zero-order (📌 "PEA" - Phenytoin, Ethanol, Aspirin; constant amount/time).
⭐ Loading dose depends on Volume of Distribution and target concentration, not clearance. Maintenance dose depends on clearance.
Pharmacodynamics - Receptor Rhapsody
- Receptor Types:
- Ligand-gated ion channels (e.g., nAChR)
- G-protein coupled (GPCR) (e.g., Adrenergic receptors)
- Enzyme-linked (e.g., Insulin receptor)
- Intracellular (e.g., Steroid receptors)
- Drug-Receptor Interaction:
- Affinity: Strength of drug-receptor binding.
- Intrinsic Activity (IA): Capacity to elicit a response (ranges 0 to 1).
- Agonists: Possess affinity & IA.
- Full Agonist: IA = 1 (max effect).
- Partial Agonist: 0 < IA < 1. Can act as antagonist with full agonist.
- Inverse Agonist: IA < 0 (stabilizes inactive receptor form).
- Antagonists: Possess affinity, but IA = 0 (no effect alone).
- Competitive (Reversible): Binds same site. Shifts DRC right (↑ $ED_{50}$), $E_{max}$ unchanged. 📌 "Right shift, same height."
- Competitive (Irreversible) & Non-competitive: ↓ $E_{max}$.
- Dose-Response Curves (DRC):
- Graded: Effect intensity vs. dose.
- Quantal: % individuals responding vs. dose.
- Potency: $ED_{50}$ (dose for 50% maximal effect). Lower $ED_{50}$ = ↑ potency.
- Efficacy: $E_{max}$ (maximal achievable effect).
- Spare Receptors: $E_{max}$ achieved before 100% receptor occupancy.
- Therapeutic Index (TI): $TI = TD_{50} / ED_{50}$. Larger TI = safer drug.
⭐ Most clinically used drugs target G-Protein Coupled Receptors (GPCRs).
 oka
oka
Clinical PK/PD - Dosing Decisions
- Goal: Achieve & maintain target drug conc. ($C_{target}$) in therapeutic window.
- Loading Dose ($LD$): Rapid effect. $LD = (V_d \cdot C_{target}) / F$.
- Maintenance Dose ($MD$): Steady state. $MD = (Cl \cdot C_{target} \cdot \tau) / F$.
- Therapeutic Drug Monitoring (TDM):
- Indications: Narrow Therapeutic Index drugs (📌 Do Little Pharmacists And Therapists? Digoxin, Lithium, Phenytoin, Aminoglycosides, Theophylline), toxicity, adherence, variable PK.
- Factors Affecting Dosing: Age, genetics, renal/hepatic impairment, drug interactions.
⭐ For drugs with long $t_{1/2}$, $LD$ is crucial; steady state on $MD$ alone takes 4-5 half-lives.
High‑Yield Points - ⚡ Biggest Takeaways
- First-pass metabolism significantly reduces oral drug bioavailability.
- High Volume of Distribution (Vd) indicates extensive tissue drug distribution.
- Clearance (CL) is crucial for determining the maintenance dose rate.
- Steady state is reached in 4-5 half-lives (t½), which also dictates dosing interval.
- Zero-order elimination (e.g., Phenytoin, Ethanol, Aspirin - "PEA") means constant amount eliminated.
- Efficacy (Emax) (maximal effect) is clinically more important than potency (EC₅₀).
- Narrow Therapeutic Index (TI) drugs (e.g., Warfarin, Digoxin, Lithium) demand close monitoring.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

