Edema Essentials - Swell Story Starters
- Edema: Palpable swelling from ↑ interstitial fluid volume.
- Governed by Starling equation:
- $J_v = K_f [(\P_c - P_i) - \sigma (\pi_c - \pi_i)]$
- $J_v$: Net filtration
- $K_f$: Capillary filtration coefficient
- $P_c$: Capillary hydrostatic pressure
- $P_i$: Interstitial hydrostatic pressure
- $\sigma$: Reflection coefficient
- $\pi_c$: Capillary oncotic pressure
- $\pi_i$: Interstitial oncotic pressure
- Primary Causes:
- ↑ $P_c$ (e.g., heart failure, DVT)
- ↓ $\pi_c$ (e.g., nephrotic syndrome, liver failure)
- ↑ Capillary permeability (e.g., inflammation, sepsis)
- Lymphatic obstruction (e.g., lymphedema)
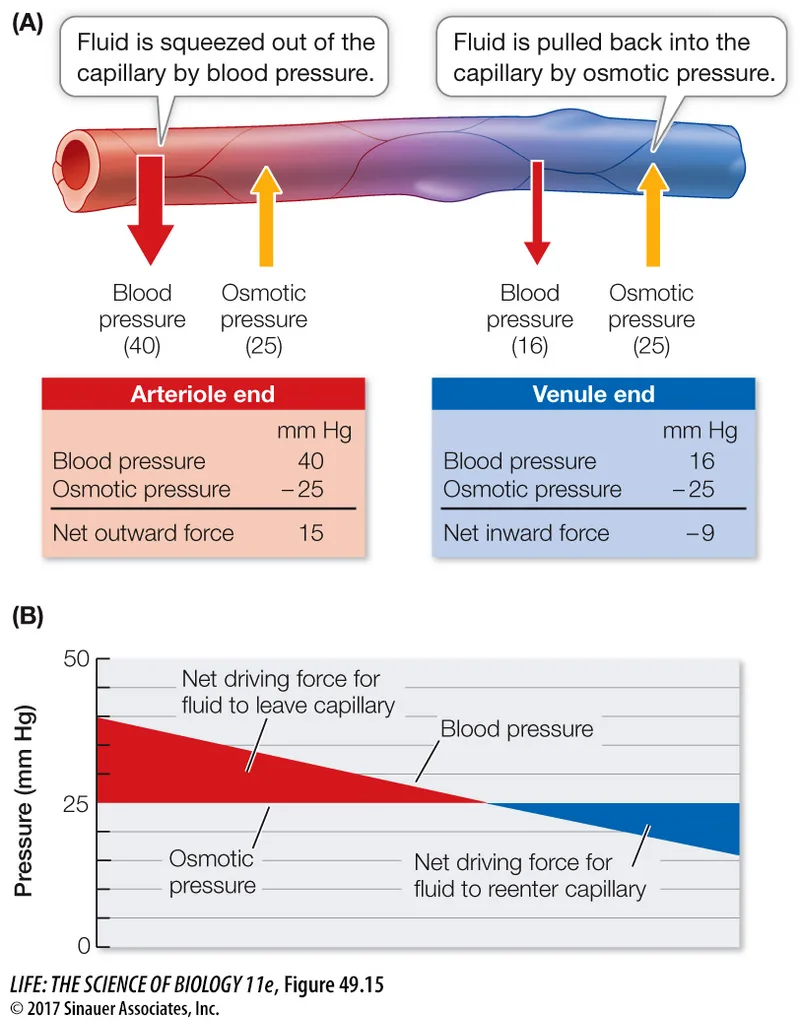
⭐ The four primary Starling forces governing fluid movement across capillaries are: capillary hydrostatic pressure ($P_c$), interstitial hydrostatic pressure ($P_i$), capillary oncotic pressure ($\pi_c$), and interstitial oncotic pressure ($\pi_i$).
Edema Evaluation - Spotting the Swell
- History & Physical Exam: Onset, duration, location (unilateral/bilateral), associated symptoms (dyspnea, pain), drug history, systemic disease review.
- Characterize Edema:
- Pitting vs. Non-pitting:
| Feature | Pitting Edema | Non-Pitting Edema |
|---|---|---|
| Mechanism | ↑ Interstitial fluid (low protein) | ↑ Interstitial protein/mucin/fibrosis |
| Indentation | Leaves a pit on pressure | No pit, firm/rubbery |
| Common Causes | Heart failure, Cirrhosis, Nephrotic syndrome, Venous insufficiency | Lymphedema, Myxedema (hypothyroidism) |
- **1+**: Mild, 2mm pit, disappears rapidly.
- **2+**: Moderate, 4mm pit, disappears in 10-15 sec.
- **3+**: Deep, 6mm pit, may last >1 min; extremity swollen.
- **4+**: Very deep, 8mm pit, lasts 2-5 min; extremity grossly distorted.
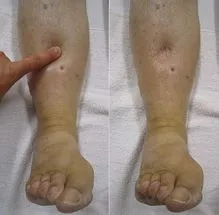
⭐ Unilateral edema often suggests local causes (e.g., DVT, cellulitis), while bilateral edema usually points to systemic conditions (e.g., heart failure, nephrotic syndrome, cirrhosis).
Systemic Swells - Body's Big Bloats
Systemic Swells (anasarca) arise from body-wide fluid dysregulation. Key mechanisms: ↑ capillary hydrostatic pressure ($P_c$), ↓ plasma oncotic pressure ($\pi_p$), ↑ capillary permeability, or lymphatic blockage.
-
Common Systemic Causes & Features:
System Key Features & Associations Cardiac Dependent, pitting edema (ankles, sacrum); worse evening. JVP ↑, dyspnea, orthopnea. (e.g., Heart Failure) Renal Periorbital puffiness (esp. AM), then generalized. Proteinuria (Nephrotic: >3.5 g/24h), hematuria (Nephritic). Hepatic Ascites often precedes peripheral edema. Jaundice, spider nevi, hypoalbuminemia. (e.g., Cirrhosis) Nutritional Generalized, soft, pitting edema. Severe hypoalbuminemia (serum albumin <2.5 g/dL). (e.g., Kwashiorkor)
⭐ Mechanism of edema in nephrotic syndrome: Massive proteinuria leads to hypoalbuminemia and decreased plasma oncotic pressure, reducing fluid return to capillaries.

📌 Mnemonic: HARK! The Swelling! (Hepatic, Albumin-low/Nutritional, Renal, Cardiac).
Local Leaks & Lumps - Regional Risers
- 📌 DVT Risk (Virchow's Triad): SHE (Stasis, Hypercoagulability, Endothelial injury).
| Feature | DVT | Cellulitis | Lymphedema |
|---|---|---|---|
| Onset | Acute/Subacute | Acute | Chronic, insidious |
| Pain | Calf tenderness, Homan's (+) | Prominent, tender, warm | Usually painless, heavy |
| Swelling | Unilateral, pitting | Unilateral, ill-defined, non-pitting early | Unilateral, non-pitting (late), brawny |
| Skin | Warm, cyanosis, dilated veins | Erythema, warmth, induration, +/- bullae | Thickened, peau d'orange, Stemmer's sign (+) |
| Fever | Low-grade possible | Common, chills | Rare |
| Dx | Doppler US; Wells Score (e.g., ≥2 high prob) | Clinical; culture if purulent | Clinical; lymphoscintigraphy |
| Etiology/Risk | Virchow's triad | Skin breach (e.g., trauma, tinea pedis) | Primary (e.g., Milroy's) or Secondary (e.g., post-surgery/RTx, filariasis) |
High‑Yield Points - ⚡ Biggest Takeaways
- Starling forces (hydrostatic & oncotic pressures) govern fluid movement across capillaries.
- Nephrotic syndrome causes generalized edema via severe hypoalbuminemia (↓ plasma oncotic pressure).
- Heart failure (especially right-sided) causes dependent edema from ↑ venous hydrostatic pressure.
- Cirrhosis leads to ascites & edema via portal hypertension and impaired albumin synthesis.
- Lymphedema is protein-rich, typically non-pitting, resulting from impaired lymphatic drainage.
- Common drug culprits: Calcium Channel Blockers (CCBs), NSAIDs, thiazolidinediones, steroids.
- Pitting edema signifies excess interstitial fluid; non-pitting suggests lymphedema or myxedema.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

