Pericardial Anatomy & Physiology - Heart's Protective Sac

- Layers: Two main parts.
- Outer: Fibrous pericardium (tough, inelastic).
- Inner: Serous pericardium.
- Parietal layer (lines fibrous).
- Visceral layer (epicardium; covers heart).
- Pericardial Cavity: Potential space between serous layers.
- Contains 15-50 mL of serous fluid (plasma ultrafiltrate) for lubrication.
- Functions:
- Fixes heart, limits motion.
- Prevents overfilling.
- Reduces friction.
- Barrier to infection/inflammation.
⭐ The pericardium has a limited elastic reserve; rapid fluid accumulation (e.g., >200 mL) can cause tamponade, while slow accumulation (e.g., >1-2 L) may be tolerated initially due to stretching over time.
Acute Pericarditis - Fiery Heart Ache

- Definition: Inflammation of the pericardium, typically < 2 weeks duration.
- Etiology:
- Idiopathic (most common)
- Infectious: Viral (Coxsackie B, Echovirus), Bacterial (TB), Fungal
- Post-MI: Early (peri-infarction pericarditis), Late (Dressler's syndrome, weeks-months post-MI)
- Uremia, Neoplasm, Autoimmune (SLE, RA), Trauma, Drugs (Hydralazine, Procainamide)
- Clinical Features:
- Chest Pain: Pleuritic (sharp, worse with inspiration/cough), postural (worse supine, relieved by sitting up/leaning forward), radiates to trapezius ridge (pathognomonic).
- Pericardial Friction Rub: Scratchy, triphasic sound (atrial systole, ventricular systole, early ventricular diastole); best heard at left sternal border with diaphragm, patient leaning forward.
- Fever, dyspnea, malaise.
- ECG Findings (sequential stages):
- Stage 1: Diffuse ST elevation (concave up), PR depression (most specific early sign).
- Stage 2: ST segments normalize, T waves flatten.
- Stage 3: T wave inversion.
- Stage 4: ECG normalizes.
- Diagnosis: ≥2 of 4 criteria: typical chest pain, pericardial rub, characteristic ECG changes, new/worsening pericardial effusion.
- Treatment:
- NSAIDs (Ibuprofen 600-800 mg TID, Aspirin 2-4 g/day) + Colchicine (0.5-0.6 mg BID for 3 months) to ↓ recurrence.
- Corticosteroids: Refractory cases or if NSAIDs contraindicated (avoid in viral pericarditis if possible).
⭐ Widespread concave ST elevation and PR depression (except aVR, V1) are hallmark ECG findings in Stage 1 acute pericarditis.
📌 PERICARDITIS Mnemonic for causes: Post-MI (Dressler's) End-stage renal disease (Uremia) Rheumatic fever/RA Infection (Viral, Bacterial, TB) Cancer (Neoplasm) Autoimmune (SLE) Radiation Drugs (Hydralazine, Procainamide) Idiopathic Trauma Inflammatory bowel disease Surgery (Post-pericardiotomy syndrome)
Pericardial Effusion & Tamponade - Fluid Fiasco, Pressure Cooker
- Pericardial Effusion: Abnormal fluid (>50 mL; normal 15-50 mL) in pericardial sac.
- Etiology: Infection (TB, viral), malignancy, uremia, autoimmune, post-MI (Dressler's).
- Sx: Often asymptomatic. Dyspnea, cough. Muffled heart sounds. Ewart's sign (dullness L scapula).
- Dx:
- CXR: Globular "water bottle" heart (>250 mL).
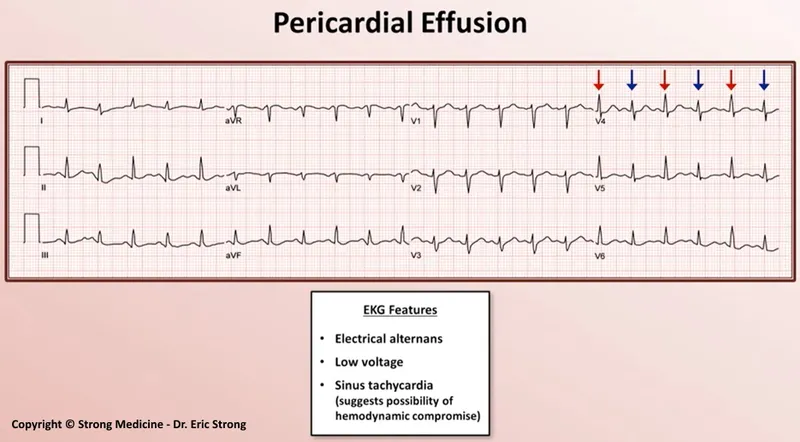
- ECG: Low voltage QRS, electrical alternans (pathognomonic).
- Echo: Gold standard; quantifies, may show swinging heart.
- Cardiac Tamponade: Life-threatening cardiac compression due to ↑intrapericardial pressure.
- Patho: ↓Venous return → ↓Diastolic filling (RA/RV collapse) → ↓CO.
- Clinical:
- Beck's Triad: Hypotension, ↑JVP (Distended Neck Veins), Muffled heart sounds. 📌 3 D's: Distant heart sounds, Distended neck veins, Decreased arterial pressure.
- Pulsus paradoxus: ↓SBP >10 mmHg on inspiration.
- Kussmaul's sign (occasional; more in constriction).
- Dx (Echo): RA & RV diastolic collapse (earliest, most sensitive), IVC plethora, swinging heart.
- Rx: Urgent pericardiocentesis. IV fluids. Avoid diuretics.
⭐ Electrical alternans on ECG, caused by the heart swinging in a large effusion, is highly specific for pericardial effusion and impending tamponade.
Constrictive Pericarditis - The Unyielding Armor
Chronic inflammation → rigid, fibrotic pericardium → impaired diastolic filling of all chambers.
- Etiology: TB (India), idiopathic, post-surgery, post-radiation.
- Clinical: Dyspnea, edema, ascites.
- Kussmaul's sign (JVP↑ inspiration).
- Pericardial knock (early diastolic).
- Friedreich's sign (prominent 'y' descent).
- Investigations:
- ECG: Low voltage, AF.
- CXR: Pericardial calcification (~50%).
- Echo: Thickened pericardium (>2mm), septal bounce.
- CT/MRI: Best for thickness (>4mm).
- Cath: Equalized diastolic pressures (within 5 mmHg), dip-and-plateau (√ sign).
- Management: Pericardiectomy (definitive). Diuretics for symptoms.
⭐ Kussmaul's sign: Paradoxical JVP rise on inspiration; classic, differentiates from tamponade (usually absent).
High‑Yield Points - ⚡ Biggest Takeaways
- Acute pericarditis: Pleuritic chest pain, friction rub, diffuse ST elevation.
- Cardiac Tamponade: Beck's triad (hypotension, JVD, muffled heart sounds), pulsus paradoxus (>10 mmHg drop).
- Constrictive Pericarditis: Kussmaul's sign, pericardial knock, pericardial calcification.
- Dressler's Syndrome: Late post-MI pericarditis (weeks after).
- Large effusion ECG: Low QRS voltage, electrical alternans.
- Viral infections (Coxsackie B) are most common cause of acute pericarditis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

