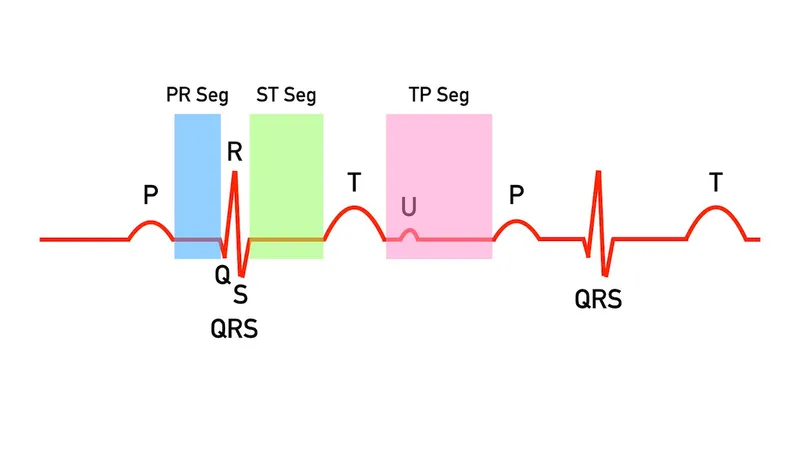
ECG - Electric Heart Beats
- Records heart's electrical activity. Standard 12 leads: 6 limb (I, II, III, aVR, aVL, aVF), 6 precordial (V1-V6).
- Calibration: 1mV = 10mm. Paper speed: 25mm/s (1 small square = 0.04s; 1 large square = 0.2s).
- Key Waveforms & Intervals:
- P wave (Atrial depol.): < 0.12s dur, < 2.5mm amp.
- PR interval (AV conduction): 0.12-0.20s.
- QRS (Ventricular depol.): < 0.12s.
- ST segment: Isoelectric. ↑/↓ = ischemia/infarct.
- T wave: Ventricular repolarization.
- QT interval (Ventricular activity). QTc (Bazett's: $QTc = QT / \sqrt{RR}$): < 0.44s M, < 0.46s F.
- Systematic Interpretation:
⭐ Wellens' syndrome: Deeply inverted/biphasic T waves in V2-V3, specific for critical LAD stenosis.
Echocardiography - Ultrasound Heart Peeks
Uses ultrasound waves for real-time imaging of heart anatomy, function, and hemodynamics.
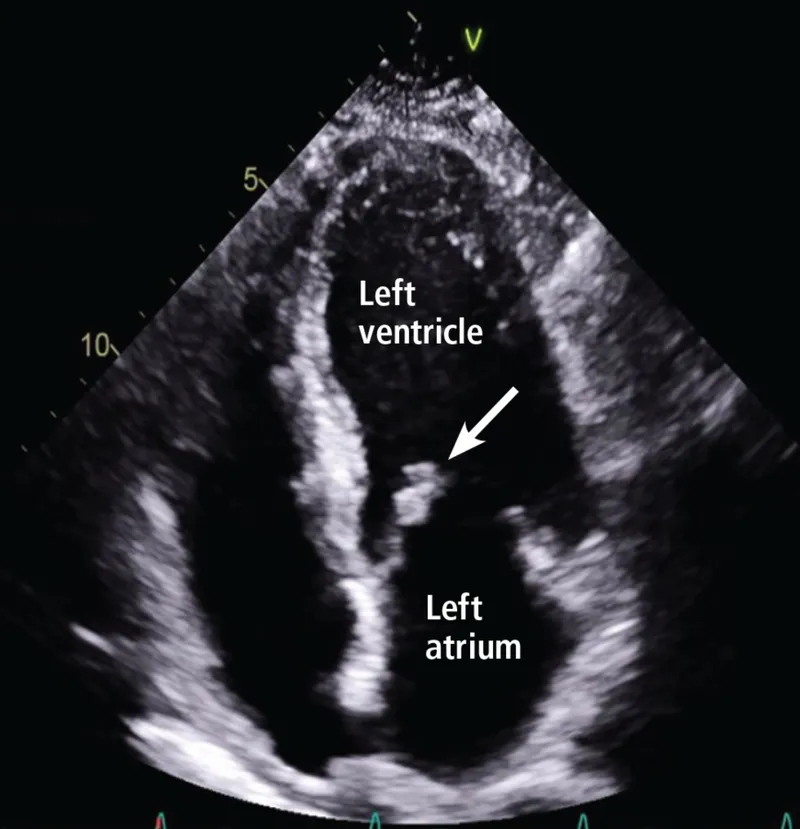
- Modes & Utility:
- 2D/M-mode: Structure, dimensions, LVEF (Normal: >55%).
- Doppler (Color, PW, CW): Blood flow, valvular lesions, shunts. $P = 4v^2$ (Modified Bernoulli for pressure gradients).
- TEE (Transesophageal Echo): Superior for posterior structures (LA/LAA, MV, aorta), endocarditis, aortic dissection.
- Stress Echo: Ischemia detection (new Regional Wall Motion Abnormalities - RWMA with stress).
- Contrast Echo: LV opacification, perfusion enhancement.
- Key Applications:
- Valvular heart disease (stenosis/regurgitation severity).
- Cardiomyopathies (HCM, DCM, RCM).
- Ischemic Heart Disease (IHD): RWMA, complications (e.g., VSR, MR).
- Pericardial effusion, tamponade.
- Diastolic dysfunction (E/A ratio, E/e' ratio).
⭐ TEE is superior to TTE for visualizing small vegetations (<5mm) in infective endocarditis and for detecting left atrial appendage (LAA) thrombus prior to cardioversion for atrial fibrillation.
Stress Testing - Heart Under Pressure
Evaluates cardiac function and ischemic response to stress.
- Types & Modalities:
- Exercise ECG (TMT): Bruce protocol. Preferred if able to exercise.
- Pharmacological Stress:
- Dobutamine Stress Echo (DSE): For wall motion.
- Vasodilator Stress MPI (Adenosine, Dipyridamole, Regadenoson): Perfusion defects (coronary steal).
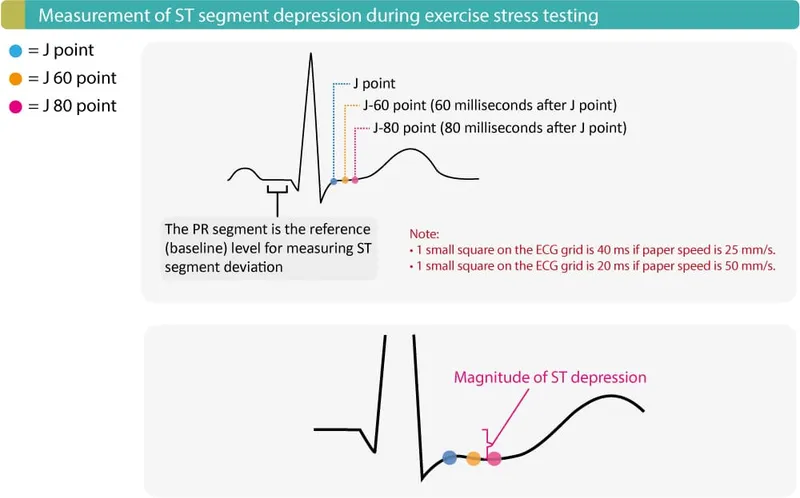
- Positive ECG: ST↓ ≥1mm (horizontal/downsloping); ST↑ ≥1mm (no prior Q-waves).
- Termination: Severe angina, ST↓ >2mm, ST↑ >1mm (no Q), ↓SBP >10mmHg, VT, target HR.
- Contraindications: Acute MI (<2 days), unstable angina, severe AS, uncontrolled HTN (>200/110 mmHg).
⭐ Duke Treadmill Score (DTS) predicts risk. High risk: score ≤ -11.
- DTS Formula: $Exercise\ time\ (min) - (5 \times ST\ deviation\ mm) - (4 \times Angina\ index)$
Ambulatory & Advanced Imaging - Beyond Clinic Walls
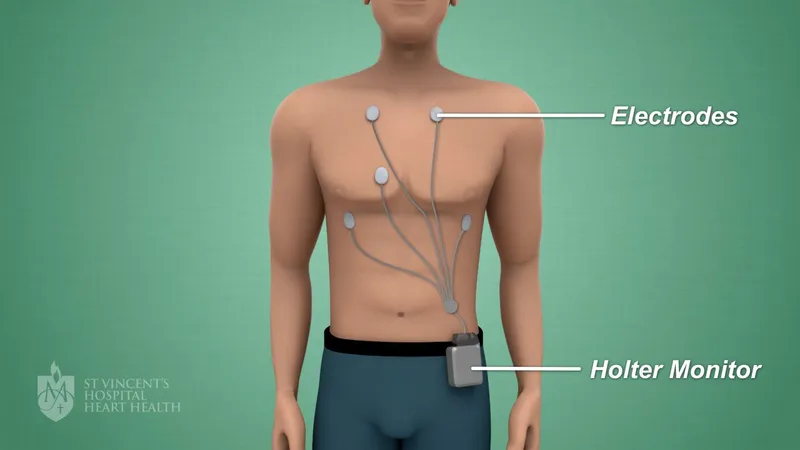
- Ambulatory ECG:
- Holter: 24-48hr continuous; frequent symptoms (palpitations, syncope).
- Event Recorders (Loop): Weeks-months; patient/auto-triggered for infrequent symptoms.
- Implantable Loop Recorder (ILR): Subcutaneous, up to 3 years; rare, severe symptoms.
- Advanced Imaging:
- Cardiac MRI (CMR): Gold standard for LV/RV volumes, function, tissue characterization (fibrosis, scar).
- Cardiac CT (CCT): Coronary Artery Calcium (CAC) score for risk; CT Coronary Angiography (CTCA) for CAD anatomy.
- Nuclear (SPECT/PET): Myocardial perfusion (ischemia/viability); PET for inflammation (e.g., sarcoidosis).
⭐ CMR is the gold standard for assessing right ventricular (RV) structure and function, key in ARVC.
High‑Yield Points - ⚡ Biggest Takeaways
- ECG is crucial for acute coronary syndromes (ACS) and arrhythmia diagnosis.
- Stress testing (TMT/Stress Echo) assesses for inducible ischemia; Dobutamine Stress Echo if unable to exercise.
- Echocardiography is key for structural heart disease, valvular function, and ejection fraction (EF).
- Holter monitoring for paroxysmal arrhythmias; Event recorders for infrequent symptoms.
- CT Coronary Angiography (CTCA) is excellent for ruling out CAD (high NPV).
- Cardiac MRI (CMR) is superior for myocardial tissue characterization, viability, and cardiomyopathies.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more