Heart Failure - The Failing Pump
-
Heart Failure (HF): Heart can't meet metabolic demands or does so at ↑ filling pressures.
- HFrEF (Heart Failure with reduced Ejection Fraction): EF < 40%
- HFpEF (Heart Failure with preserved Ejection Fraction): EF ≥ 50%
- HFmrEF (Heart Failure with mildly reduced Ejection Fraction): EF 40-49%
-
Classifications:
System Stages Summary NYHA I (Asymptomatic) - IV (Symptoms at rest) ACC/AHA A (At Risk) - D (Refractory HF)
⭐ The most common cause of Right Heart Failure is Left Heart Failure.
Heart Failure - Why It Breaks
Error generating content for this concept group: Failed to process successful response
Heart Failure - Spotting Trouble
-
Symptoms: Dyspnea (DOE, orthopnea, PND), fatigue, edema, cough (frothy).
-
Signs: Tachycardia, S3/S4, ↑JVP, edema, creps, hepatomegaly.
-
📌 Mnemonics:
- Left HF (DOABLE): Dyspnea, Orthopnea, Awakening, Basal creps, Lung sounds-wheeze, Expectoration-frothy.
- Right HF (CHAPS): Cor pulmonale, Hepatomegaly, Ascites, Peripheral edema, Splenomegaly.
-
Diagnostic Tools:
- ECG: LVH, prior MI, arrhythmias.
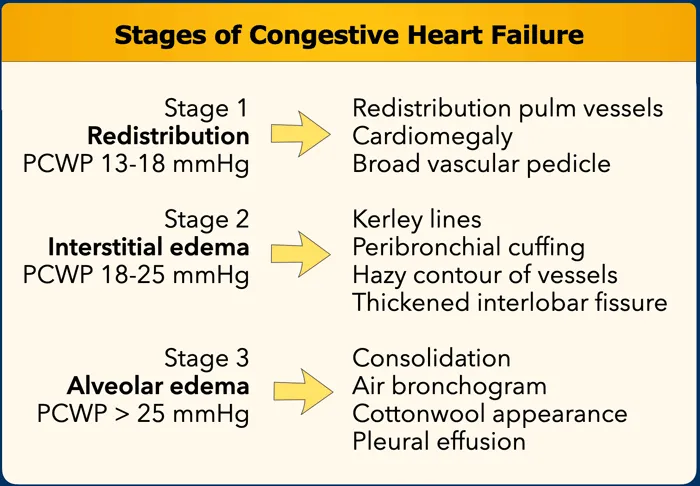
- CXR: Cardiomegaly, pulm. congestion (Kerley B), effusion.
- Echo (key): EF, wall motion, diastolic fx, valves.
- Biomarkers: BNP > 100, NT-proBNP > 300 pg/mL (↑ if renal issues/elderly).
-
Framingham criteria aid CHF diagnosis.
⭐ S3 gallop: highly specific for HF, especially with dyspnea.
Heart Failure - Mending Hearts
Non-pharm: Salt <2g/day, fluid <1.5-2L/day, lifestyle modifications. Pharm HFrEF (📌 'BASH' - 4 Pillars GDMT):
- ARNI (Sacubitril/Valsartan preferred) / ACEi / ARB
- Beta-blockers (Carvedilol, Metoprolol Succinate, Bisoprolol)
- MRA (Spironolactone, Eplerenone; monitor K+)
- SGLT2i (Dapagliflozin, Empagliflozin; regardless of diabetes) Diuretics (Loop) for symptomatic relief of congestion. HFpEF: Manage comorbidities (BP, etc.), diuretics for congestion, SGLT2i show benefit. Devices: ICD (primary/secondary SCD prevention); CRT (LVEF ≤35%, QRS ≥150ms LBBB, NYHA II-IV).
⭐ ARNIs (Sacubitril/Valsartan) have shown superiority over ACE inhibitors in reducing mortality and hospitalization in HFrEF.

Heart Failure - Code Blue Crisis
- Definition: Acute worsening of Heart Failure (HF) signs/symptoms requiring urgent therapy.
- Triggers: Non-compliance (diet/meds), ACS, arrhythmia (e.g., AF), infection, uncontrolled HTN, PE.
- Stevenson Profiles (Perfusion/Congestion) & Key Tx:
- Warm & Wet: IV Diuretics, Vasodilators (if SBP >90-100 mmHg).
- Cold & Wet: IV Diuretics + IV Inotropes/Vasopressors.
- Cold & Dry: IV Fluids (cautiously), then IV Inotropes if no response.
- Key Meds: IV Loop Diuretics, IV Vasodilators, IV Inotropes. Oxygen, Non-Invasive Ventilation (NIV).
- 📌 LMNOP for acute pulmonary edema: Lasix, Morphine (less used), Nitrates, Oxygen, Position (upright).
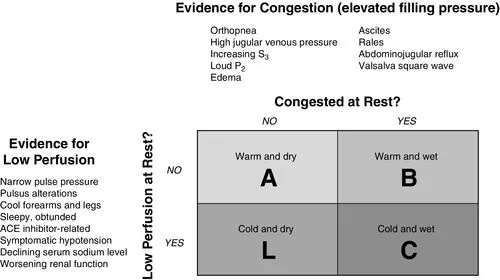
⭐ The 'Cold and Wet' profile in Acute Decompensated Heart Failure (ADHF) carries the worst prognosis and often requires aggressive therapy including inotropes.
High‑Yield Points - ⚡ Biggest Takeaways
- Ischemic Heart Disease (IHD): most common cause of heart failure.
- NYHA Classification: key for symptom severity and guiding treatment.
- BNP/NT-proBNP: vital biomarkers for diagnosis, prognosis, and therapy response.
- HFrEF cornerstone drugs: ARNI/ACEi/ARB, Beta-blockers, MRAs, SGLT2is improve survival.
- Sacubitril/Valsartan (ARNI): superior mortality benefit vs ACEi/ARB in HFrEF.
- HFpEF: manage comorbidities (HTN, DM); diuretics for congestion relief.
- Acute Decompensated HF (ADHF): manage with LMNOP (Lasix, Morphine, Nitrates, Oxygen, Position) protocol.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

