Arrhythmia Basics & ECG - ECG Code Crackers
- Normal Conduction: SA node → AV node → Bundle of His → Bundle branches → Purkinje fibers.
- Arrhythmia: Any rhythm deviating from normal sinus rhythm.
- ECG Components:
- P wave: Atrial depolarization.
- PR interval: AV nodal delay; normal 0.12-0.20s.
- QRS complex: Ventricular depolarization; normal <0.12s.
- T wave: Ventricular repolarization.
- U wave: Late ventricular repolarization (Purkinje fibers).
- Key Ion Channels: $Na^+$ (fast depolarization), $Ca^{2+}$ (pacemaker potential, plateau), $K^+$ (repolarization).

⭐ The U wave, when prominent, can indicate hypokalemia or effects of certain drugs like quinidine or digitalis.
Bradyarrhythmias - Slow Beat Scene
Error: Failed to generate content for this concept group.
Supraventricular Tachycardias - Atrial Rhythm Riot
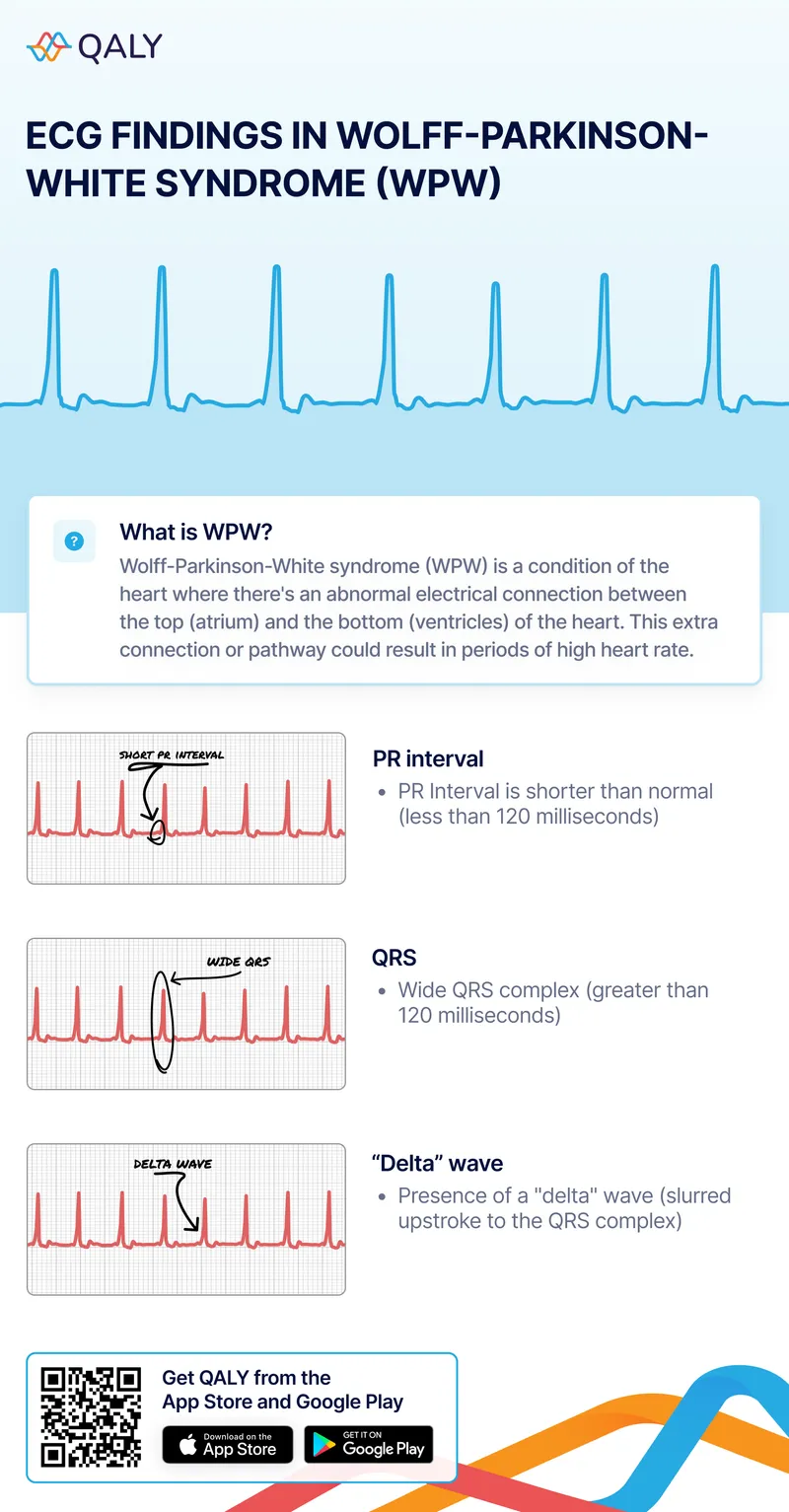
⭐ WPW + AF/Flutter: AV nodal blockers (adenosine, BB, CCB, digoxin) are contraindicated; risk VF via accessory pathway.
- Key SVTs & ECG:
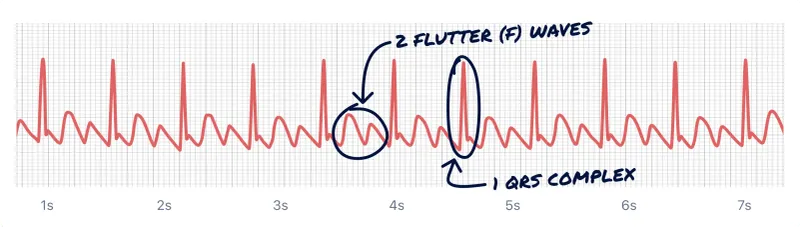
SVT Rhythm P waves / ECG Adenosine AF Irreg. irreg. Absent, fibrillatory Slows rate Atrial Flutter Regular (often) Sawtooth (F) Unmasks F waves AVNRT Regular Buried/retrograde P Terminates AVRT (WPW) Regular Delta, short PR Terminates MAT Irregular ≥3 P types, varying PR/RR; lung dz Variable, may slow - Acute: Vagal → Adenosine (6mg IV, then 12mg) → CCB/BB → Cardioversion.
- Chronic: Rate/Rhythm control. AF: Anticoagulate (CHA2DS2-VASc). 📌 CHA2DS2-VASc: CHF(1), HTN(1), Age ≥75(2)/ 65-74(1), DM(1), Stroke/TIA(2), Vasc Dz(1), Sex F(1).

Ventricular Arrhythmias - Ventricle Danger Vibes
- PVCs: Wide QRS, ectopic.
- VT (Ventricular Tachycardia): Wide QRS (>0.12s).
- Stable Monomorphic: Amiodarone 150mg IV.
- Unstable (pulse): Sync. Cardioversion (100J).
- Pulseless VT/VF: Defibrillation (e.g., 120-200J biphasic), CPR, Amiodarone 300mg IV. (ACLS)
- TdP (Torsades de Pointes): Polymorphic VT, long QT. Mgmt: IV Mg (2g).
- Brugada Syn: Coved ST ↑ V1-V3. ICD.
- ARVD: Epsilon wave. ICD.
- 📌 H's & T's for reversible causes (cardiac arrest).
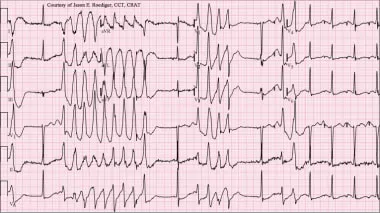
⭐ Synchronized cardioversion is used for unstable VT with a pulse, while defibrillation (unsynchronized shock) is used for pulseless VT or VF. Amiodarone is a key antiarrhythmic for both stable VT and in ACLS for refractory VT/VF.
Antiarrhythmic Drugs - Rhythm Rx Roundup
| Cl | Drug | MOA | Use | SE Crit. |
|---|---|---|---|---|
| Ia | Quinidine | Na+(mod) | SVT, VT | TdP |
| Ib | Lidocaine | Na+(wk) | Post-MI VT | Neuro |
| Ic | Flecainide | Na+(str) | SVT, AF (NSHD) | Proarrhythmia |
| II | Metoprolol | β-Blk | Rate ctrl, SVT | Brady |
| III | Amiodarone | K+ Blk | AF, VT/VF | Pulm/Thyroid |
| IV | Verapamil | Ca2+ Blk | SVT, Rate ctrl | Constipation |
- Other:
- Adenosine: ↓AVN; Acute SVT; SE: Flush.
- Digoxin: ↑Vagal; AF rate ctrl; SE: GI, vision.
- MgSO4: TdP, Dig-tox.
⭐ Beta-blockers (Class II antiarrhythmics) are contraindicated in patients with cocaine-induced myocardial ischemia/tachycardia as they can lead to unopposed alpha-adrenergic stimulation, worsening coronary vasoconstriction and hypertension.
High‑Yield Points - ⚡ Biggest Takeaways
- Atrial fibrillation: Most common sustained arrhythmia. Key is stroke prevention (CHADS-VASc).
- Ventricular tachycardia: Pulseless VT needs immediate defibrillation. Stable VT: amiodarone.
- WPW syndrome: Short PR, delta wave. Avoid AV nodal blockers (e.g., adenosine, verapamil, digoxin).
- AVNRT: Most common paroxysmal SVT. Treat with vagal maneuvers, then adenosine.
- Brugada syndrome: Coved ST elevation (V1-V3), risk of SCD. ICD is treatment.
- Torsades de Pointes: Associated with Long QT syndrome. Treat with magnesium sulfate.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

