Stimulants Overview - Buzz Basics
- Common Types:
- Cocaine
- Amphetamines (e.g., Methamphetamine, MDMA/Ecstasy)
- Methylphenidate
- Synthetic cathinones ("Bath salts")
- Core Mechanism: ↑ synaptic Dopamine (DA), Norepinephrine (NE), Serotonin (5-HT).
- Cocaine: Blocks reuptake of DA, NE, 5-HT.
- Amphetamines: ↑ release & block reuptake of DA, NE.
- Key Effects: Euphoria, ↑ alertness, ↓ appetite, sympathetic activation.
- Epidemiology: Rising trend globally and in India, especially among youth.
⭐ Formication (sensation of insects crawling on/under skin) is a common tactile hallucination in chronic cocaine/amphetamine use.
 oka
oka
Intoxication & Overdose - Highs & Hazards
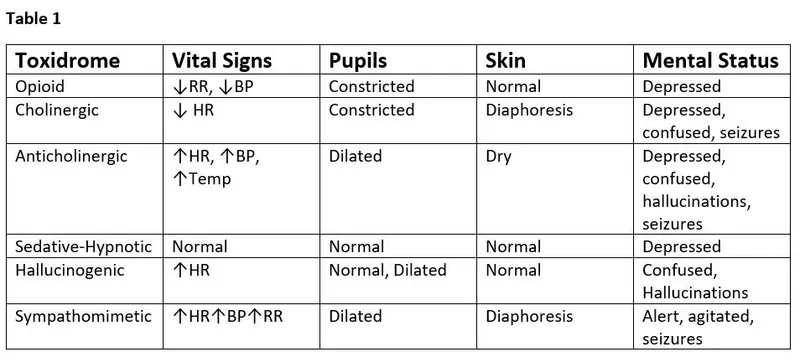
- Intoxication (Sympathomimetic Toxidrome):
- Presents with ↑SNS activity. 📌 Mnemonic: "MATHS" (Mydriasis, Agitation/Arrhythmia, Tachycardia/Tremors, Hypertension/Hyperthermia, Seizures/Sweating).
- CNS: Euphoria, agitation, psychosis, seizures, hyperthermia (can exceed 40°C).
- CVS: Tachycardia, hypertension, arrhythmias, chest pain (MI risk).
- Pupils: Mydriasis (dilated). Skin: Diaphoresis.
- Overdose Hazards (Life-Threatening):
- Cardiovascular: MI, aortic dissection, stroke.
- Neurological: Status epilepticus, intracranial hemorrhage.
- Metabolic: Severe hyperthermia → rhabdomyolysis → AKI.
- Emergency Management:
- ABCs, IV access, cardiac monitoring.
- Benzodiazepines (e.g., IV Lorazepam): First-line for agitation, seizures, tachycardia, hypertension.
- Aggressive cooling for hyperthermia.
- ⚠️ Avoid pure beta-blockers (risk of unopposed alpha-stimulation causing paradoxical hypertension/coronary vasoconstriction).
⭐ In cocaine-associated chest pain, benzodiazepines and nitrates are key. Avoid beta-blockers initially.
Withdrawal & Chronic Use - Crash & Complications
- Stimulant Withdrawal ("Crash"):
- Symptoms: Intense dysphoria, fatigue, anhedonia, ↑ appetite, vivid dreams.
- Psychomotor changes (retardation/agitation), insomnia/hypersomnia.
- Timeline: Peaks 2-4 days, resolves ~1 week. High relapse risk.
- Chronic Use Complications:
- Cardiovascular: MI, arrhythmias, cardiomyopathy, HTN, aortic dissection.
- Neurological: Stroke, seizures, movement disorders, cognitive impairment.
- Psychiatric: Psychosis (paranoid delusions, formication - "meth bugs"), anxiety, depression.
⭐ Formication (sensation of insects crawling on skin) is a classic tactile hallucination in chronic stimulant users, often leading to skin picking.
- Dental: "Meth Mouth" - severe decay (xerostomia, bruxism, poor hygiene).
- Infectious (IV use): HIV, Hepatitis B/C, endocarditis.
- Other: Malnutrition, skin excoriations, nasal septal perforation (snorting).
 oka
oka
Diagnosis & Management - Spotting & Stopping
- Diagnosis (DSM-5): Pattern of use with ≥2 of 11 criteria in 12 months (e.g., impaired control, social impairment, risky use, tolerance, withdrawal). Severity: Mild (2-3), Moderate (4-5), Severe (≥6).
- Screening: Urine drug screen (UDS), clinical interview (e.g., ASSIST, DAST-10).
- Management:
- Psychosocial interventions are cornerstone.
- Contingency Management (CM): Reinforces abstinence.
- Cognitive Behavioral Therapy (CBT).
- Supportive care for withdrawal ("crash").
- Psychosocial interventions are cornerstone.
⭐ Currently, no FDA-approved pharmacotherapy exists for stimulant use disorder; management relies heavily on behavioral therapies.
High‑Yield Points - ⚡ Biggest Takeaways
- Stimulants (e.g., cocaine, amphetamines) primarily ↑ dopamine.
- Intoxication: Euphoria, agitation, mydriasis, tachycardia, hypertension, formication ("cocaine bugs").
- Withdrawal: Dysphoria, fatigue, ↑ appetite, psychomotor changes, vivid unpleasant dreams.
- Complications: Myocardial infarction, stroke, seizures, nasal septal perforation (cocaine).
- Acute Intoxication Management: Benzodiazepines for agitation/seizures; AVOID beta-blockers (unopposed alpha risk).
- Withdrawal Management: Supportive care; no specific FDA-approved pharmacotherapy for dependence.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

