Opioids 101 - Brain's Poppy Problem
- Classification:
- Natural: Morphine, Codeine (from Papaver somniferum)
- Semi-synthetic: Heroin, Oxycodone, Buprenorphine
- Synthetic: Fentanyl, Methadone, Pethidine, Tramadol
- Mechanism of Action (MOA):
- Agonists at opioid receptors: μ (mu), κ (kappa), δ (delta).
- Primarily μ-receptor activation: analgesia, euphoria, respiratory depression, miosis.
- Receptors are G-protein coupled (Gi/Go): ↓ cAMP, open K+ channels (hyperpolarization), close Ca2+ channels (↓ neurotransmitter release).
- Neurobiology of Addiction:
- ↑ Dopamine in mesolimbic reward pathway (Ventral Tegmental Area to Nucleus Accumbens).
- Chronic use leads to neuroadaptation: tolerance & withdrawal.
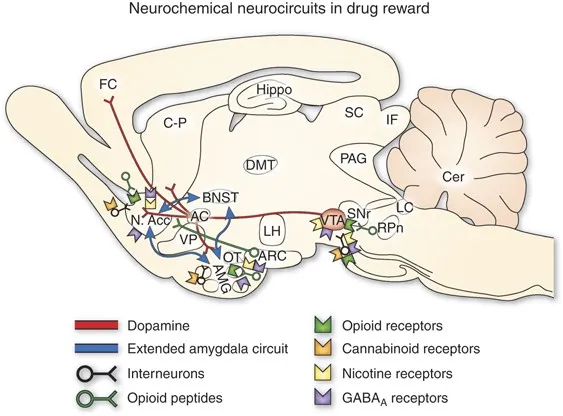
⭐ Buprenorphine is a partial μ-opioid agonist and κ-opioid antagonist, used in opioid de-addiction due to its ceiling effect on respiratory depression and milder withdrawal symptoms compared to full agonists like methadone or heroin. It can precipitate withdrawal if given to a patient on a full μ-agonist due to its high affinity and lower intrinsic activity at the μ-receptor.
OUD Unmasked - Spotting the Signs
- Opioid Intoxication:
- Classic Triad: Coma, pinpoint pupils (miosis), respiratory depression.
- Also: Drowsiness, slurred speech, euphoria, ↓BP, ↓HR.
- ⚠️ Severe respiratory depression can be fatal.
- Opioid Withdrawal: (Distressing, rarely life-threatening)
- Flu-like: Myalgia, fever, lacrimation, rhinorrhea, yawning.
- GI: Nausea, vomiting, diarrhea, cramps.
- CNS arousal: Mydriasis, piloerection ("gooseflesh"), insomnia, restlessness, anxiety.
- Onset: Short-acting (e.g., heroin) 6-12h; Long-acting (e.g., methadone) 24-72h.
- COWS (Clinical Opiate Withdrawal Scale) for severity.
- Diagnosis (DSM-5 for OUD):
- Pattern of use causing significant distress/impairment.
- Requires ≥2 of 11 criteria over 12 months (impaired control, social impairment, risky use, pharmacological).
⭐ Pupil response is a vital diagnostic clue: Miosis (pinpoint) in intoxication, Mydriasis (dilated) in withdrawal.
Crisis Control - Tackling Overdose & Withdrawal
Opioid Overdose
- Immediate: ABCs (Airway, Breathing, Circulation).
- Antidote: Naloxone 0.4-2 mg IV/IM/SC; repeat q2-3min.
- Max 10 mg. No response? Re-evaluate diagnosis.
- ⚠️ Renarcotization risk (naloxone short half-life).
- Supportive: O2, ventilation.
Opioid Withdrawal
- Assess: COWS (Clinical Opiate Withdrawal Scale).
- Mild: 5-12; Mod: 13-24; Mod-Sev: 25-36; Sev: >36.
- Symptomatic Rx:
- Clonidine 0.1-0.3 mg (autonomic; monitor BP).
- NSAIDs (pain), Loperamide (diarrhea), Ondansetron (N/V).
- MAT Start: Buprenorphine (COWS >8-12).
- Day 1: 2-4 mg, up to 8-12 mg.
⭐ Naloxone's short half-life (30-90 min) compared to many opioids (e.g., methadone) necessitates prolonged observation for renarcotization after initial reversal.
Road to Recovery - Long-Term MAT Strategies
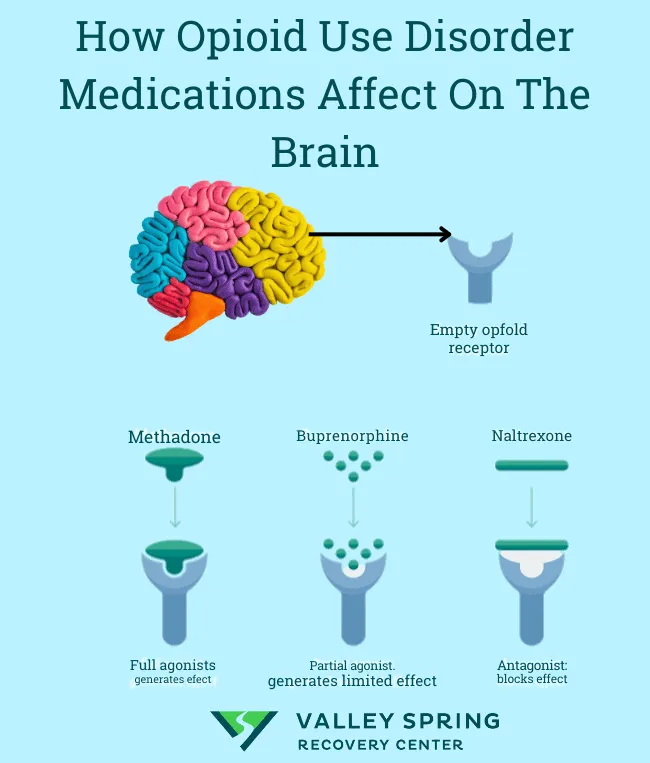
- Methadone:
- Full µ-opioid agonist.
- Daily at Opioid Treatment Programs (OTPs).
- Reduces cravings & withdrawal symptoms.
- ⚠️ Risk: QTc prolongation, interactions.
- Buprenorphine:
- Partial µ-opioid agonist; κ-antagonist.
- Ceiling effect on respiratory depression.
- Sublingual (SL), implant, LAI.
- Often with naloxone to deter IV misuse.
- Naltrexone:
- Opioid antagonist; blocks opioid effects.
- Oral daily or LAI monthly.
- Requires 7-10 days opioid-free period (precipitated withdrawal risk).
- Non-addictive, no diversion risk.
- Psychosocial Support:
- Essential adjunct (counseling, therapies).
- Essential adjunct (counseling, therapies).
⭐ Buprenorphine's availability in office-based settings (unlike methadone for OUD requiring OTPs) improves treatment access.
High‑Yield Points - ⚡ Biggest Takeaways
- Opioid intoxication triad: miosis (pinpoint pupils), respiratory depression, altered mental status. Antidote: Naloxone.
- Opioid withdrawal: severe flu-like symptoms (e.g., piloerection, mydriasis, diarrhea, lacrimation), not life-threatening.
- MAT is first-line: Methadone (long-acting full agonist), Buprenorphine (partial agonist), Naltrexone (antagonist).
- Buprenorphine can precipitate withdrawal if administered before opioid effects wear off.
- Naltrexone (oral/injectable) requires full detoxification; contraindicated in acute liver failure.
- Clonidine helps manage autonomic hyperactivity in withdrawal; Lofexidine is also FDA-approved for this purpose.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

