IAI: Overview - Gut Gone Wrong
- Intra-abdominal Infection (IAI): Inflammation within peritoneal cavity due to microorganisms.
- Types:
- Primary Peritonitis (Spontaneous Bacterial Peritonitis - SBP): No evident intra-abdominal source. Common in liver cirrhosis.
- Secondary Peritonitis: Due to perforation/inflammation of GI tract (e.g., appendicitis, diverticulitis, PUD). Most common type.
- Tertiary Peritonitis: Persistent/recurrent infection after initial treatment, often with resistant organisms.
- Classification:
- Uncomplicated IAI: Infection confined to a single organ.
- Complicated IAI (cIAI): Infection extends beyond organ into peritoneal space; associated with abscess or peritonitis.
- Common Origins: Appendix, colon, stomach/duodenum, biliary tract.
⭐ Most common cause of secondary peritonitis is perforated appendicitis.
IAI: Pathogens & Process - Belly's Bad Bugs
- Key Pathogens (Often Polymicrobial):
- Aerobes:
- Escherichia coli (most frequent Gram-negative)
- Klebsiella spp.
- Enterococcus spp. (Gram-positive cocci)
- Anaerobes:
- Bacteroides fragilis (most frequent anaerobe)
- Clostridium spp.
- Peptostreptococcus
- Fungi (e.g., Candida): Consider in immunocompromised, prolonged antibiotics, or recurrent IAI.
- 📌 Mnemonic: "BECK" - Bacteroides, E.coli, Clostridium, Klebsiella.
- Aerobes:
- Pathogenesis Cascade:
- Source of microbes:
- Perforation (e.g., appendicitis, diverticulitis, Peptic Ulcer Disease)
- Ischemia/Necrosis (e.g., mesenteric ischemia, strangulated bowel)
- Translocation (e.g., severe pancreatitis, shock states)
- Peritoneal contamination → Inflammation (Peritonitis).
- Host defense: Opsonization, phagocytosis, fibrin deposition (walling-off → phlegmon/abscess).
- Source of microbes:
⭐ Escherichia coli is the most common aerobic pathogen, and Bacteroides fragilis is the most common anaerobic pathogen in Intra-abdominal Infections (IAIs).
IAI: Diagnosis - Spotting Sepsis Signs
- Clinical:
- Local: Abdominal pain, tenderness, guarding, rigidity.
- Systemic: Fever, tachycardia, hypotension.
- Labs:
- ↑WBC (left shift), ↑CRP.
- ↑Serum Lactate (>2 mmol/L = hypoperfusion).
- ↑Procalcitonin. Blood cultures (pre-antibiotics).
- Imaging:
- X-Ray (erect): Free air (perforation), air-fluid levels.
- USG: Fluid, abscesses, organ-specific (e.g., appendicitis, cholecystitis).
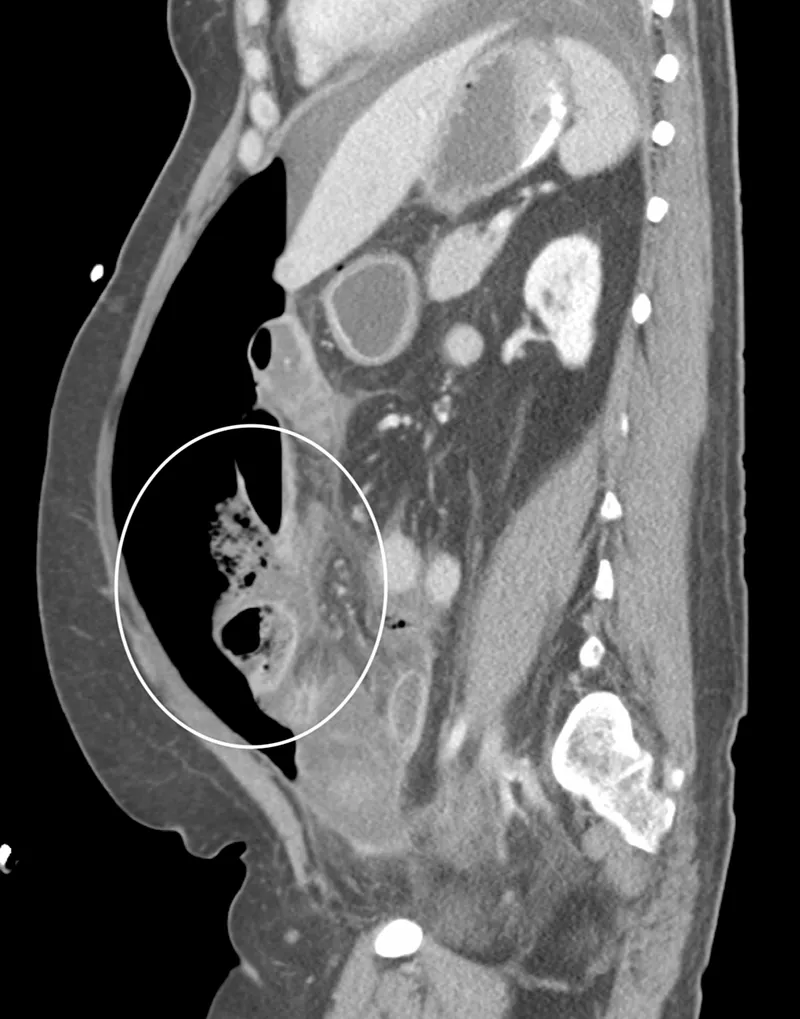
- CT (Contrast): Gold standard for source, extent, complications.
- Sepsis (qSOFA ≥2):
- Respiratory Rate ≥22/min
- Altered Mentation (GCS <15)
- Systolic BP ≤100 mmHg 📌 Mnemonic: HAT (Hypotension, Altered Mental Status, Tachypnea).
⭐ Serum lactate >2 mmol/L is a key indicator of tissue hypoperfusion and adverse outcomes in sepsis. Early qSOFA assessment is vital for timely intervention in IAI cases.
IAI: Treatment - Quelling the Chaos
-
Core Principles (Time-Sensitive):
- Resuscitation: ABCs, IV crystalloids, O2. Target UO > 0.5 ml/kg/hr.
- Early Empiric Antibiotics: Broad-spectrum IV within 1 hour of sepsis/septic shock diagnosis.
- Definitive Source Control: Within 6-12 hours. Critical for outcomes.
-
Antimicrobial Strategy:
- CA-IAI (Community-Acquired):
- Mild-Moderate (e.g., uncomplicated appendicitis, diverticulitis): Ertapenem OR (Ceftriaxone/Cefotaxime + Metronidazole).
- Severe/High-Risk (e.g., diffuse peritonitis): Piperacillin-Tazobactam OR Carbapenem (Imipenem, Meropenem).
- HA-IAI (Hospital/Healthcare-associated):
- Broader coverage for MDROs (Pseudomonas, ESBL): Piperacillin-Tazobactam, Carbapenems. Add Vancomycin/Linezolid if MRSA suspected.
- Duration: Typically 4-7 days after adequate source control.
- CA-IAI (Community-Acquired):
-
Source Control Modalities:
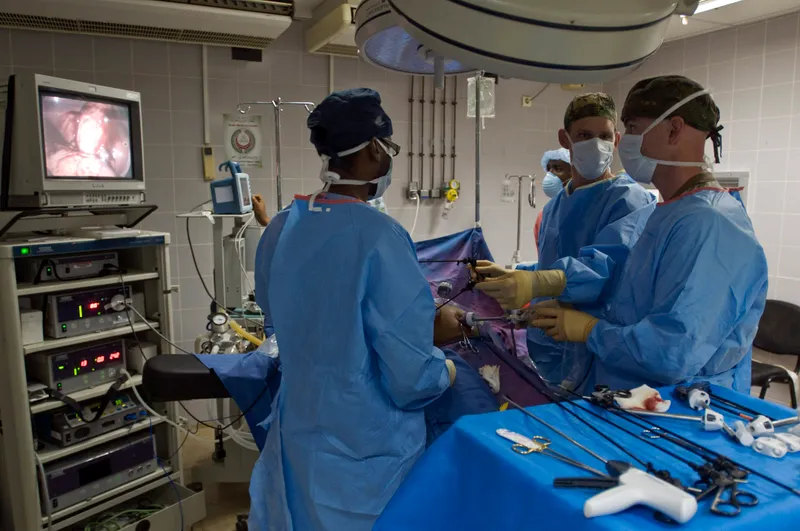
- Surgical: Laparotomy/laparoscopy (e.g., appendectomy, resection, repair of perforation).
- Percutaneous Drainage (PCD): For localized abscesses.
⭐ In complicated IAI (e.g., perforated diverticulitis with abscess), achieving source control within 6 hours is associated with significantly improved survival.
-
Supportive Measures:
- Nutritional support (enteral preferred), DVT & stress ulcer prophylaxis.
High‑Yield Points - ⚡ Biggest Takeaways
- Secondary peritonitis: E. coli (aerobic) & B. fragilis (anaerobic) are most common.
- Tertiary peritonitis: Persistent infection, often resistant organisms or fungi.
- Hinchey classification guides diverticulitis management; Stages III & IV often need surgery.
- Appendicitis: Primarily clinical diagnosis; Alvarado score aids, imaging for equivocal cases.
- Source control (drainage/repair/resection) is key, with antibiotics.
- Empirical antibiotics: Must cover gram-negative bacilli & anaerobes.
- Intra-abdominal abscess: Percutaneous drainage (USG/CT guided) is often treatment.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

