Skin Grafts: Intro & Types - Patch It Up!
- Skin graft: Transfer of epidermis & varying amounts of dermis to a recipient site. Autograft (self), allograft (same species), xenograft (different species).
- Main types: Split-Thickness Skin Graft (STSG) & Full-Thickness Skin Graft (FTSG).
| Feature | STSG | FTSG |
|---|---|---|
| Source | Epidermis + partial dermis | Epidermis + entire dermis |
| Thickness | Variable (0.008-0.012 inches) | Full dermal thickness |
| Donor Sites | Thigh, buttock, abdomen, back | Groin, postauricular, supraclavicular, eyelid |
| Advantages | Large areas, good take, donor site re-epithelializes | Better cosmesis, ↓ secondary contraction |
| Disadvantages | Poor cosmesis, ↑ secondary contraction | Limited size, donor site needs primary closure |
| Contraction | Mainly Secondary | Mainly Primary |
Graft Physiology: Survival Steps - Making It Stick
Graft survival unfolds in three crucial phases: 📌 PIeR.
- Plasmatic Imbibition (Serum Soak): 24-48 hours.
- Graft passively absorbs plasma-like fluid, nutrients, and oxygen from the recipient bed.
- Graft swells slightly; cells remain viable but no active circulation.
- Inosculation (Capillary Kiss): Day 3-5.
- Alignment and direct anastomosis of donor graft capillaries with recipient bed capillaries.
- Establishes initial, fragile blood flow.
- Revascularization (New Pipes): Day 5-7.
- New blood vessels actively grow into the graft from the recipient bed.
- Establishes robust, definitive circulation and lymphatic drainage.
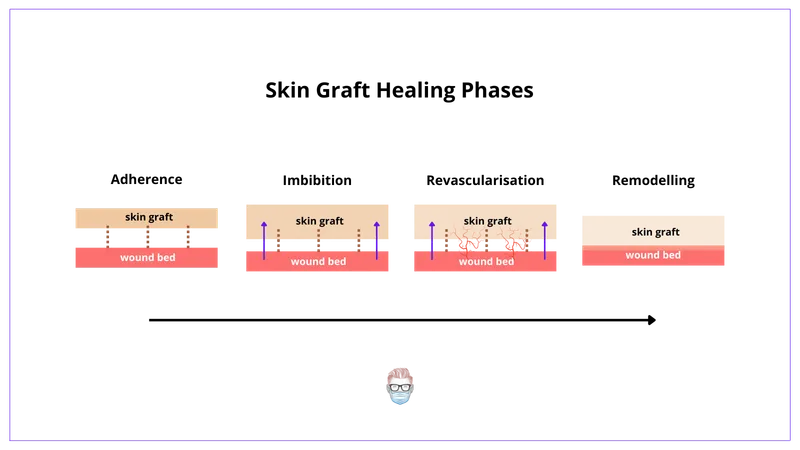
⭐ The 'bridging phenomenon' during inosculation, where recipient and donor capillaries align and connect, is critical for graft survival and typically starts around day 3-4.
Site Management: Donor & Bed - Prime Real Estate
- Donor Site Considerations:
- Split-Thickness Skin Graft (STSG):
- Common Sites: Thigh, buttock, scalp.
- Healing: 7-21 days by re-epithelialization from adnexal structures.
- Care: Occlusive or semi-occlusive dressings (e.g., paraffin gauze, polyurethane film).
- Full-Thickness Skin Graft (FTSG):
- Common Sites: Postauricular, supraclavicular, groin, antecubital fossa.
- Healing: Donor site typically closed primarily.
- Pros: Better cosmesis, less secondary contraction.
- Split-Thickness Skin Graft (STSG):
- Recipient Site Preparation ("Ideal Bed"):
- Vascularity: Must be well-vascularized (e.g., healthy granulation tissue). Avoid avascular beds (bare bone/tendon without peri/paratenon).
- Debridement: Thorough removal of necrotic tissue, eschar, and debris.
- Hemostasis: Meticulous; hematoma or seroma beneath graft is a common cause of failure.
- Bacterial Load: Infection control critical; bacterial count ideally < 10^5 CFU/gram of tissue.
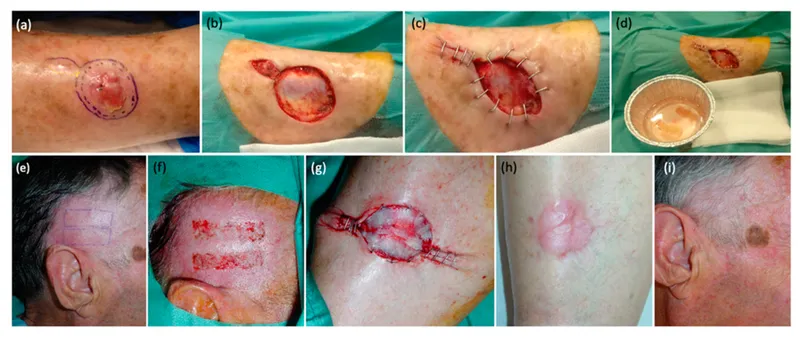
⭐ A well-vascularized recipient bed with bacterial counts below 10^5 organisms per gram of tissue is essential for successful skin graft take.
Graft Issues: Complications - When Patches Pucker
Common Causes of Graft Failure: 📌 HISSS
- Hematoma: Blood clot under graft, lifts it from bed.
- Infection: Bacterial (e.g., Pseudomonas, Staph), fungal.
- Seroma: Lymphatic fluid collection.
- Shearing forces: Mechanical disruption of adherence.
- Systemic factors/Poor bed: Malnutrition, smoking, diabetes, irradiated tissue, poor vascularity.
⭐ Hematoma formation beneath a graft is the most common cause of early graft failure as it physically separates the graft from its nutrient bed.
Other Complications:
- Contracture: Significant functional/cosmetic issue, esp. over joints.
- Pigmentary changes: Mismatch with surrounding skin (hypo/hyper).
- Hypertrophic scarring/Keloids: Abnormal scar tissue.
- Graft breakdown: Ulceration, chronic instability.

High‑Yield Points - ⚡ Biggest Takeaways
- STSG: Better take, ↑contraction, donor heals spontaneously. FTSG: Better cosmesis, ↓take, donor needs closure.
- Graft survival stages: Imbibition (0-48h), inosculation, then revascularization.
- Hematoma is the commonest cause of graft failure; infection & shear are also key.
- Meshing STSGs increases surface area (e.g., 1:1.5 to 1:6) and allows exudate drainage.
- A vascularized, infection-free bed is vital for graft take.
- Wolfe graft = FTSG; Thiersch graft = STSG.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

