HD 101 - Gut's Missing Ganglia
- Congenital aganglionic megacolon causing functional bowel obstruction.
- Embryology: Defective craniocaudal migration of neural crest cells (NCCs) during weeks 4-12 gestation.
- NCCs fail to populate distal bowel.
- RET gene mutations are frequently implicated.
- Pathophysiology: Absence of ganglion cells (Auerbach's & Meissner's plexuses) in distal segment.
- Results in a tonically contracted aganglionic segment.
- Leads to proximal bowel dilatation.
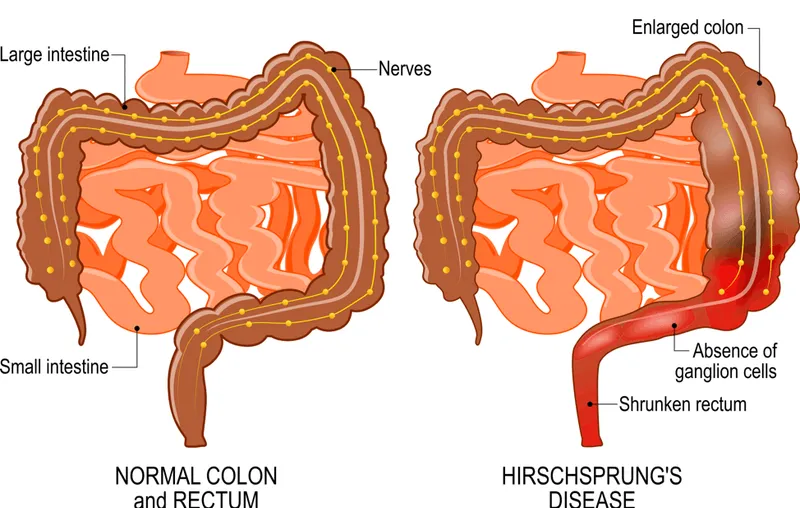
⭐ The aganglionosis always starts at the anus and extends proximally; rectosigmoid is affected in ~80% of cases.
HD Signs - Blocked Baby Blues
| Feature | Neonates | Older Infants/Children |
|---|---|---|
| Meconium | Failure to pass (>24-48h) - cardinal sign | History of delayed passage |
| Vomiting | Bilious | Occasional, may be non-bilious |
| Abdomen | Progressive distension | Chronic distension, palpable fecal masses |
| Stools | Obstipation; explosive on DRE | Chronic constipation, ribbon-like, foul |
| Systemic | Enterocolitis risk (fever, diarrhea) | Failure to thrive (FTT), malnourishment |
HD Detective - Unmasking Aganglionosis
- Suspicion: Failure to pass meconium (>24-48h), bilious emesis, abdominal distension, chronic constipation, enterocolitis episodes.
- Imaging:
- AXR: Dilated proximal bowel loops, paucity of distal gas.
- Contrast Enema (Barium/Gastrografin): Transition zone (key!), narrow spastic distal segment, dilated proximal bowel. Retained contrast >24h.
- Anorectal Manometry: Absence of Rectoanal Inhibitory Reflex (RAIR); useful if enema equivocal or in older children.
- Gold Standard: Rectal Biopsy
- Suction biopsy (2-3 cm above dentate line) or full-thickness.
- Histology: Absence of ganglion cells (submucosal/myenteric plexuses).
- Key: Hypertrophied nerve trunks (Acetylcholinesterase positive staining).
⭐ Gold standard: Full-thickness rectal biopsy showing aganglionosis & hypertrophied, AChE-positive nerve trunks. 📌 HD: Transition Zone, Aganglionic Biopsy. (TZAB)
HD Solutions - Surgical Fixes & Woes
- Core Principle: Resect aganglionic segment, pull-through healthy bowel to anus.
- Key Procedures:
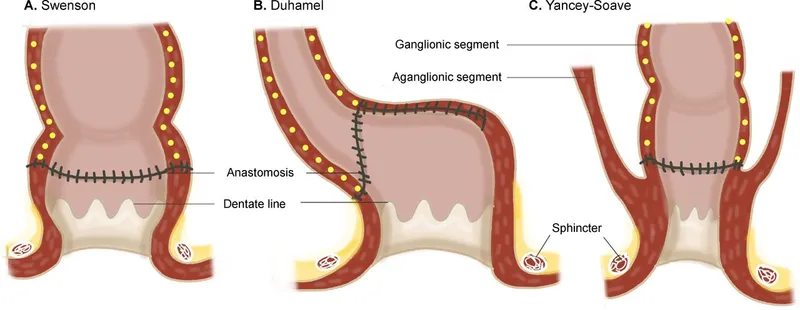
- Swenson: Original pull-through; full-thickness resection.
- Soave: Endorectal mucosectomy, ganglionated bowel pulled through muscular cuff. (📌 Soave = Submucosal/Stripping)
- Duhamel: Retrorectal transanal pull-through; side-to-side anastomosis.
- Minimally Invasive: Laparoscopic or transanal (TEPT).
- Post-Op Woes:
- Hirschsprung-Associated Enterocolitis (HAEC):
- Signs: Fever, distension, explosive foul diarrhea.
- Rx: Aggressive! IV fluids, antibiotics, rectal irrigations.
- Anastomotic stricture/leak.
- Persistent constipation/soiling.
- Hirschsprung-Associated Enterocolitis (HAEC):
⭐ HAEC remains the leading cause of morbidity and mortality in HD patients, occurring in up to 20-30% even after corrective surgery.
High‑Yield Points - ⚡ Biggest Takeaways
- Congenital aganglionosis of the distal bowel, most commonly rectosigmoid.
- Results from failed neural crest cell migration to the hindgut.
- Neonates: delayed meconium passage (>24-48 hours), bilious vomiting, abdominal distension.
- Gold standard diagnosis: Rectal biopsy showing absent ganglion cells.
- Contrast enema: transition zone between narrowed aganglionic and dilated ganglionic bowel.
- Anorectal manometry: absent rectoanal inhibitory reflex (RAIR).
- Treatment: Surgical resection of affected segment; risk of Hirschsprung-Associated Enterocolitis (HAEC).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

