Early Major Complications - Fistula, Bleed, Slow Gut
-
Pancreatic Fistula (POPF) (ISGPS Definition)
- Drain amylase >3x serum on/after POD3.
- Grades:
- BL: No clinical impact.
- B: Intervention (NPO, TPN, antibiotics, drain).
- C: Reoperation, organ failure.
- Mgmt: Conservative → Percutaneous Drainage → ERCP (stent) → Surgery.
⭐ Clinically relevant POPF (Grade B/C) is associated with amylase-rich fluid >3x serum amylase on/after POD3.
-
Post-Pancreatectomy Hemorrhage (PPH) (ISGPS Definition)
- Timing: Early (<24h, technical) vs. Late (>24h, POPF-related, sentinel bleed).
- Severity:
- A: Mild.
- B: Intervention (transfusion, angio/endo).
- C: Re-laparotomy, life-threatening.
- Mgmt Flowchart:
- Delayed Gastric Emptying (DGE) (ISGPS Definition)
- NGT needed >3 days / unable to tolerate oral diet by POD7-10.
- Grades:
- A: NGT 4-7 days / no solids by POD7.
- B: NGT 8-14 days / no solids by POD14.
- C: NGT >14 days / no solids by POD21.
- Mgmt: NGT decompression, prokinetics, nutritional support.
Infections & Other Leaks - Bugs & Bile
- Infections (Common Post-Op):
- Bugs: Gram-negatives (E.coli, Klebsiella), Enterococcus; often polymicrobial.
- Types: Surgical Site Infections (SSI; superficial/deep), Intra-abdominal abscess (IAA; e.g., peripancreatic).
- Dx: Fever, ↑WBC, local signs (erythema, discharge); CT scan for IAA.
- Rx: Broad-spectrum IV Antibiotics, source control (drainage for IAA).

- Bile Leak (ISGPS Definition):
- Manifests: Typically after POD3; persistent drain output, bilious character.
- Causes: Hepaticojejunostomy failure, small duct injury, cystic duct stump.
- Grades: A (no change), B (active Rx, no organ failure), C (re-op/organ failure).
- Rx: Prolonged drainage, ERCP + stent, PTBD; rarely re-operation.
⭐ Bile leak: Bilirubin in drain fluid >3 times serum bilirubin (post-op day 3+).
Systemic & General Issues - Body's Backlash
- Cardiovascular: MI, DVT/PE, arrhythmias, acute heart failure (fluid overload, stress).
- Respiratory: Atelectasis, pneumonia (VAP risk), ARDS, significant pleural effusion.
- Renal: Acute Kidney Injury (AKI); causes: hypovolemia, sepsis, nephrotoxic agents.
- Metabolic & Endocrine:
- Electrolyte shifts: ↓K⁺, ↓Mg²⁺ (arrhythmogenic), ↓Ca²⁺.
- Stress hyperglycemia; new-onset/worsening diabetes post-resection.
- Hematological: Anemia (blood loss, dilutional), coagulopathy (↑risk with sepsis, DIC).
- Gastrointestinal: Prolonged postoperative ileus; stress-related mucosal bleeding.
- Neurological: Postoperative delirium (esp. elderly, ICU, sepsis-associated encephalopathy).
- SIRS/Sepsis/MODS: Systemic inflammation, often from leaks, leading to multi-organ dysfunction.
⭐ Acute Respiratory Distress Syndrome (ARDS) post-pancreatectomy is a severe complication with mortality rates often exceeding 40%.
Late Sequelae - The Long Haul
- Pancreatic Insufficiency:
- Exocrine (EPI): Common post-PD (Pancreaticoduodenectomy). Symptoms: steatorrhea, weight loss. Rx: PERT (Pancreatic Enzyme Replacement Therapy).
- Endocrine (Diabetes Mellitus - Type 3c): ↑ risk with distal/extensive resection. Monitor HbA1c (target <7%). Rx: Diet, OHA (Oral Hypoglycemic Agents), Insulin.
- Biliary Strictures:
- Anastomotic (e.g., hepaticojejunostomy). Symptoms: jaundice, cholangitis. Dx/Rx: ERCP/PTC (stenting/dilation).
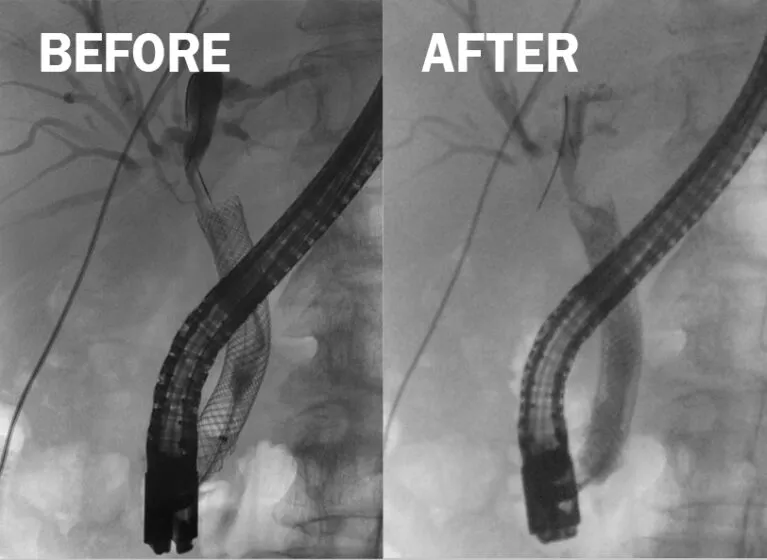
- Anastomotic (e.g., hepaticojejunostomy). Symptoms: jaundice, cholangitis. Dx/Rx: ERCP/PTC (stenting/dilation).
- Nutritional Deficiencies:
- Malabsorption of fat-soluble vitamins (A, D, E, K), B12. Monitor & supplement.
- Chronic Pain:
- Due to chronic pancreatitis in remnant, adhesions, or neuromas.
- Incisional Hernia & Adhesive SBO (Small Bowel Obstruction):
- Long-term surgical site/abdominal risks.
- Malignancy Recurrence:
- Key concern if surgery for cancer; requires surveillance.
⭐ Pancreatic exocrine insufficiency is common after pancreaticoduodenectomy, often requiring pancreatic enzyme replacement therapy (PERT).
High‑Yield Points - ⚡ Biggest Takeaways
- Pancreatic fistula (POPF): Most common & feared complication; ISGPS grading is key.
- Delayed Gastric Emptying (DGE): Frequent post-Whipple, impacts recovery; ISGPS graded.
- Post-pancreatectomy Hemorrhage (PPH): Early (technical) vs. late (e.g., pseudoaneurysm); sentinel bleed is ominous.
- Intra-abdominal infections/abscesses: Major source of sepsis and prolonged stay.
- Endocrine insufficiency: Risk of new/worsening diabetes mellitus (Type 3c).
- Exocrine insufficiency: Causes maldigestion, steatorrhea; often requires PERT (Pancreatic Enzyme Replacement Therapy).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


