SSI Classification & Pathogens - Bug's Life in Wounds
SSIs occur at/near surgical incision within 30 days post-op, or 1 year with an implant.
- CDC Classification:
- Superficial Incisional SSI:
- Involves skin & subcutaneous tissue only.
- Criteria: Pus, positive culture, or surgeon's diagnosis.
- Pathogens: S. aureus (most common), CoNS, Streptococcus spp.
- Deep Incisional SSI:
- Involves deep soft tissues (fascia, muscle layers).
- Criteria: Purulent drainage, dehiscence with fever/pain, abscess, or surgeon's diagnosis.
- Pathogens: S. aureus, Gram-negative bacilli (GNB e.g., E. coli), anaerobes.
- Organ/Space SSI:
- Involves any organ/space (excluding incision sites) manipulated during surgery.
- Criteria: Drain pus, positive culture from aspirate, abscess, or surgeon's diagnosis.
- Pathogens: Site-specific (e.g., E. coli, Enterococcus for intra-abdominal).
- Superficial Incisional SSI:

⭐ Staphylococcus aureus is the leading cause of SSIs, especially for incisional types (superficial and deep).
SSI Risk & Prevention - Dodging Infection Darts
-
Patient Factors: Age, DM (>7% HbA1c), obesity (>30 BMI), smoke, poor nutrition, IC, MRSA.
-
Procedure Factors: Long duration, emergency, implant, poor technique, contamination.
-
Wound Classification & Prophylaxis Strategy:
-
Key Prevention:
- Pre-op: Optimize patient, clip hair (NO shave), CHG-alcohol skin prep.
- Intra-op: Asepsis, gentle handling, normothermia/glycemia.
⭐ Endogenous flora (e.g., S. aureus) = main SSI source.
SSI Diagnosis & Management - Germ Warfare Tactics
Diagnosis:
- Clinical Signs:
- Local: Redness, warmth, swelling, pain, purulent discharge (📌 PUS: Purulence, Undermining, Systemic signs).
- Systemic: Fever >$ extbf{38}$°C, tachycardia >$ extbf{90}$ bpm, ↑WBC >$ extbf{12,000}$/mm³, SIRS.
- Investigations:
- Wound C&S (before Abx). Gram stain aids early choice.
- Blood cultures (if systemic signs/SIRS).
- Imaging (USS/CT) for deep/organ space SSI, abscesses.
Management:
- Source Control (KEY):
- I&D of collections/abscesses.
- Debridement (necrotic tissue).
- Wound lavage. (NPWT if complex).
- Antibiotics:
- Empiric (broad: S. aureus, Strep, GNBs, anaerobes).
- Tailor to C&S; shortest effective duration.
- Supportive: Analgesia, fluids, nutrition, glucose control.
⭐ Most common SSI pathogen: Staphylococcus aureus.
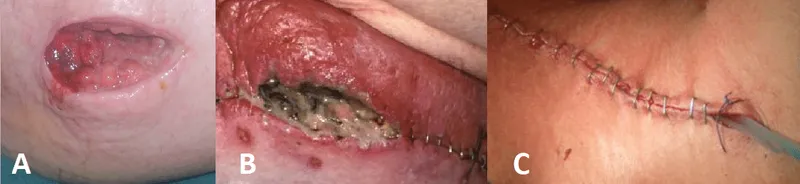
Key Surgical Infections - Nasty Invaders Showdown
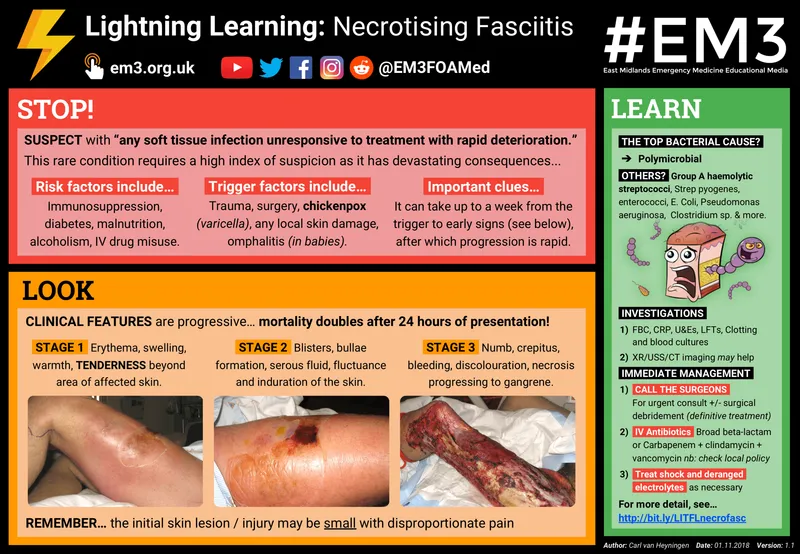
- Necrotizing Soft Tissue Infections (NSTI):
- Rapid spread, pain out of proportion, crepitus, skin necrosis. LRINEC score ≥6 (e.g. CRP >150 mg/L, WBC >15x10⁹/L).
- Tx: Urgent surgical debridement, broad-spectrum Abx.
- Gas Gangrene (Clostridial Myonecrosis):
- C. perfringens. Sudden pain, crepitus, bronze skin, foul discharge. Gram +ve rods.
- Tx: Debridement, Penicillin G + Clindamycin, ± Hyperbaric Oxygen (HBO).
⭐ C. perfringens alpha-toxin (lecithinase) causes massive hemolysis & tissue necrosis.
- Tetanus:
- C. tetani. Trismus (lockjaw), risus sardonicus, opisthotonus, spasms.
- Tx: HTIG (3000-6000 IU), Metronidazole, debridement, spasm control. 📌 SAD ANT (mgt).
- Carbuncle:
- S. aureus. Deep infection of multiple hair follicles (nape of neck common).
- Tx: Incision & Drainage (I&D) if fluctuant, antibiotics.
High‑Yield Points - ⚡ Biggest Takeaways
- Staphylococcus aureus is the most common organism for Surgical Site Infections (SSI).
- Administer prophylactic antibiotics within 1 hour before surgical incision.
- Clean-contaminated wounds carry a higher infection risk than clean wounds.
- Necrotizing fasciitis is a surgical emergency requiring prompt, aggressive debridement.
- Gas gangrene, caused by Clostridium perfringens, presents with crepitus and systemic toxicity.
- Early postoperative fever (within 48 hours) is often due to atelectasis, not necessarily infection.
- Source control (e.g., drainage, debridement) is crucial in managing established surgical infections.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

