Pre-op & Staging - Setting the Stage
- Initial Assessment:
- History (risk factors, family hx), Clinical Breast Exam (CBE).
- Bilateral mammography (MMG) & USG (breast & axilla).
- Diagnosis & Receptor Status:
- Core Needle Biopsy (CNB): Histopathology, ER/PR/HER2.
- FNAC/CNB for suspicious axillary nodes.
- Staging (AJCC TNM):
- Tumor size/invasion, Nodal status, Metastasis.
- Metastatic workup (CT C/A/P, Bone Scan; PET-CT often used) for:
- Locally advanced (≥Stage III).
- Aggressive biology (e.g., Triple Negative).
- Symptoms of metastasis.
- Pre-op Fitness: Routine labs, ECG, CXR (as indicated).
- Counseling: Surgery, reconstruction, neoadjuvant therapy (NACT) options.
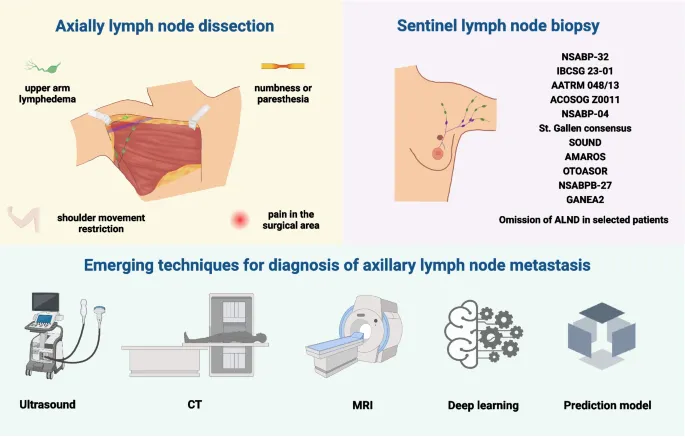
⭐ Sentinel Lymph Node Biopsy (SLNB) is standard axillary staging for clinically node-negative (cN0) early breast cancer.
Surgical Options - Chopping Choices
- Breast Conserving Surgery (BCS): Tumor + margin removal.
- Indications: Unifocal, < 4 cm, good tumor-breast ratio.
- Mandatory post-op Radiotherapy (RT).
- Goal: Negative margins ("no ink on tumor").
- Avoid: Inflammatory Ca, multicentric, prior RT, pregnancy (early).
- Mastectomy (Entire breast removal):
- Simple/Total: Breast, Nipple-Areola Complex (NAC).
- Modified Radical (MRM): Total Mastectomy + Axillary Lymph Node Dissection (ALND I & II).
- Patey: Pectoralis minor spared.
- Skin/Nipple-Sparing (SSM/NSM): For reconstruction.
- Indications: Large/multicentric, RT C/I, patient choice.
- Axillary Staging:
- Sentinel Node Biopsy (SLNB): Standard for cN0 axilla.
- Axillary Dissection (ALND): For cN+ or +SLNB (per criteria).
⭐ ACOSOG Z0011: For T1/T2, 1-2 +SLNs, BCS + Whole Breast RT, ALND omission is often safe.
BCS vs Mastectomy - The Big Debate
- Core Principle: For early-stage invasive cancer, BCS + Radiotherapy (RT) offers equivalent overall survival to Mastectomy.
- BCS: Tumor + margins removed; breast preserved. RT essential.
- Mastectomy: Entire breast removed. RT for high-risk cases.
| Aspect | BCS + RT | Mastectomy |
|---|---|---|
| Local Recurrence | Comparable with RT | Lower |
| Cosmesis | Breast preserved | Breast absent (reconstruction option) |
- Multicentric disease / diffuse calcifications
- Prior chest RT / cannot receive RT
- Persistent +ve margins
- Inflammatory cancer
- Large tumor/small breast (poor cosmesis)
⭐ Overall survival for early-stage breast cancer is similar with BCS + RT versus mastectomy.
Axilla & Complications - Arming Against Issues
- Axillary Staging: Key for prognosis & treatment.
- SLNB (Sentinel Node Biopsy): Standard for cN0. Uses dye + Tc-99m.
- ACOSOG Z0011: May avoid ALND if 1-2 SLN+ (BCS, WBRT, no ENE).
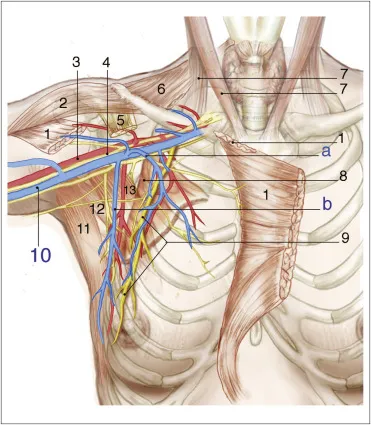
- ALND (Axillary Dissection): For cN+ or SLNB+ (not Z0011). Levels I & II.
- Pectoralis minor: landmark for Levels I (lat), II (post), III (med).
- SLNB (Sentinel Node Biopsy): Standard for cN0. Uses dye + Tc-99m.
- Key Complications:
- Lymphedema: ↑Risk with ALND, RT, obesity. Manage: arm care, physio.
- Seroma: Common. Aspirate if symptomatic.
- Nerve Injury:
* Shoulder stiffness, chronic pain.
⭐ Intercostobrachial nerve is most commonly injured in ALND, causing upper inner arm numbness.
High‑Yield Points - ⚡ Biggest Takeaways
- BCS + Radiotherapy offers survival equivalent to Mastectomy for most early breast cancers.
- SLNB is standard for axillary staging in clinically node-negative (cN0) patients.
- ALND is indicated for positive SLNB or clinically positive axillary nodes.
- Key BCS contraindications: multicentric disease, Inflammatory Breast Cancer (IBC), inability to get negative margins.
- "No ink on tumor" is the standard margin for invasive cancer in BCS.
- Prophylactic mastectomy is an option for high-risk individuals (e.g., BRCA carriers).
- Oncoplastic surgery enhances cosmetic outcomes in BCS while maintaining oncologic safety.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

