AGB Basics - The Squeeze Play
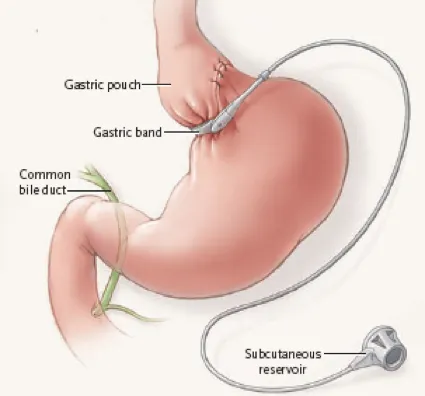
- Purely restrictive bariatric procedure; no malabsorption.
- An inflatable silicone band is placed around the proximal stomach.
- Creates a small gastric pouch (approx. 15-30 mL) above the band.
- A narrow outlet (stoma) limits food passage, inducing early satiety.
- Band tightness is adjustable via a subcutaneous access port (saline injection/removal).
- Mechanism: ↓ food intake, ↑ satiety.
⭐ Band slippage is a common long-term complication, potentially requiring re-operation or removal.
Who Gets Banded? - Gatekeeping Gastric Access
- Indications:
- BMI ≥ 40 kg/m² OR BMI ≥ 35 kg/m² with obesity-related comorbidities (T2DM, HTN, OSA).
- Age 18-65 years.
- Failed ≥6 months conservative weight loss.
- Psychologically stable, motivated, informed.
- Acceptable surgical risk.
- Contraindications:
- Untreated endocrine obesity (Cushing's, hypothyroidism).
- Active substance/alcohol abuse.
- Severe, uncontrolled psychiatric illness.
- Crohn’s disease.
- Pregnancy.
- Poor long-term compliance anticipated.
⭐ AGB shows lower long-term weight loss efficacy & higher re-operation rates compared to sleeve gastrectomy or gastric bypass, significantly limiting its current clinical application.
Banding Blueprint - Surgical Steps
- Technique: Laparoscopic, typically 5 ports.
- Key Dissection: Pars Flaccida technique for safe retrogastric tunnel creation.
- Band Position: Placed ~2 cm below GE junction, creating a small proximal pouch (~15-30 mL).
- Anti-Slippage: Gastrogastric fixation sutures (usually 3-4 anteriorly).
- Adjustment Access: Subcutaneous port connected to band (e.g., anterior abdominal wall).
⭐ Band slippage/pouch dilation: most common late complication needing reoperation.
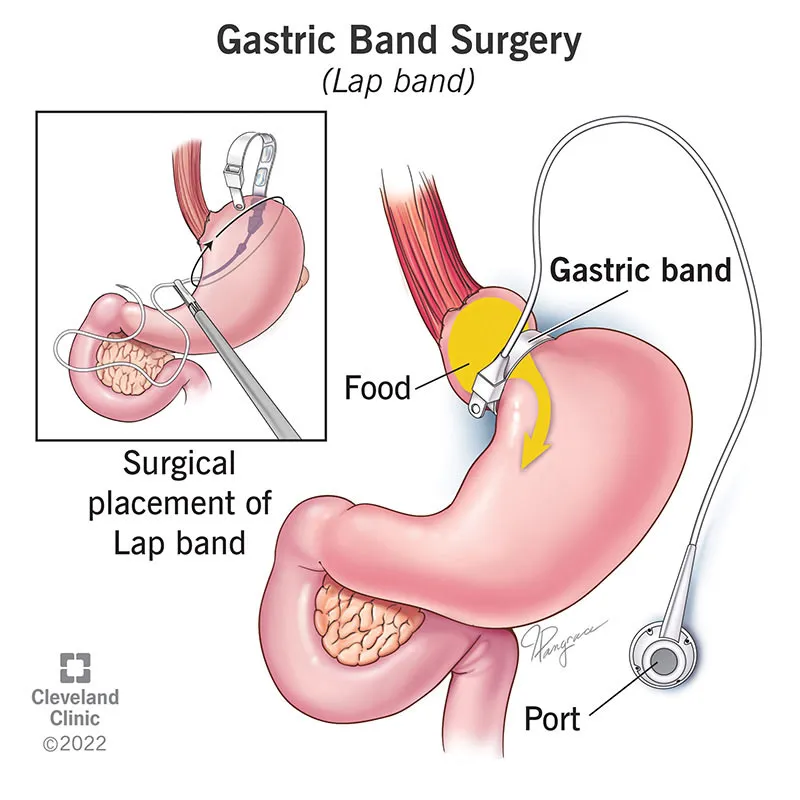
Life with the Band - Adjust & Adapt
- Dietary Progression:
- Clear liquids initially → Full liquids (1-2 wks) → Pureed (2 wks) → Soft (2 wks) → Regular (small, nutrient-dense, ~1/2 cup portions).
- Eating Habits:
- Small bites, chew thoroughly. Eat slowly.
- Separate fluids from meals (~30 min).
- Avoid high-calorie liquids, carbonated drinks.
- Band Adjustments:
- Saline via subcutaneous port.
- Guided by satiety & weight loss.
- Usually 4-6 adjustments in 1st year.
- Lifelong follow-up essential.

⭐ Optimal restriction is achieved when the patient feels satisfied with small meals without experiencing vomiting, significant reflux, or dysphagia to solids.
Pitfalls & Payoffs - Band's Balance Sheet
Pitfalls (Complications):
- Early (<30 days):
- Port site issues (infection, hematoma, pain)
- Acute band slippage/prolapse
- Gastric injury (rare, <1%)
- Late (>30 days):
- Band erosion into stomach (1-4%)
- Chronic slippage, pouch dilation, stomal obstruction
- Esophageal dysmotility, GERD exacerbation
- Port/tubing failure (leak, fracture, flip)
- Inadequate weight loss / weight regain
- High reoperation rate (approaching 50-60% over time)
Payoffs (Outcomes):
- Weight Loss:
- Excess Weight Loss (EWL): 40-60% (gradual)
- Total Body Weight Loss (TBWL): ~15-20%
- Comorbidity Improvement/Resolution:
- T2DM: ~50-60% resolution
- Hypertension: ~40-50% improvement
- Dyslipidemia, Obstructive Sleep Apnea (OSA)
- Key Advantages:
- Adjustable (titratable restriction) & Reversible
- Laparoscopic, no stapling/anastomosis
- Lower initial operative risk; minimal malabsorption

⭐ High long-term reoperation rates, frequently due to band slippage or erosion, represent a significant limitation of AGB.
High‑Yield Points - ⚡ Biggest Takeaways
- Purely restrictive; creates a small proximal gastric pouch (~15-30ml) using an inflatable band.
- Adjustable via a subcutaneous port, allowing titration of stoma size and restriction.
- Reversible procedure; band can be laparoscopically removed if needed.
- Offers lesser weight loss and higher reoperation rates compared to RYGB or sleeve gastrectomy.
- Common complications: band slippage/prolapse, gastric erosion, port/tubing issues, esophageal dilatation.
- No malabsorption; lower initial perioperative risk but requires strict compliance & frequent adjustments.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

