Types & Triggers - Reaction Rundown
Contrast Reaction Classification & Triggers
| Type | Mechanism | Onset | Key Symptoms |
|---|---|---|---|
| Anaphylactoid | Pseudoallergic; Mast cell release | <1 hr (often 5-20 min) | Urticaria, angioedema, bronchospasm, hypotension |
| Physiologic (Chemotoxic) | Dose/osmolality-dependent; Direct organ toxicity | Variable | Nausea, vomiting, warmth, vasovagal, CIN, cardiac |
| Delayed | T-cell mediated (Type IV) | >1 hr - 1 wk | Skin rashes (maculopapular). Rare: SJS/TEN |
- Contrast: HOCM > LOCM > IOCM; Ionic > Non-ionic.
- Patient: Asthma, allergies, anxiety, dehydration, renal/cardiac issues.
⭐ Prior contrast reaction: most significant risk factor (future reaction risk ↑ 5-6x).
Risk & Prevention - Shielding Strategies
- Risk Factors:
- Prior moderate/severe contrast reaction (📌 Strongest)
- Asthma, multiple severe allergies
- Symptomatic cardiac disease
- Meds: β-blockers, NSAIDs, IL-2
- Prevention:
- Identify high-risk patients.
- Use Low-Osmolar (LOCM) or Iso-Osmolar Contrast Media (IOCM).
- Premedicate if indicated.
⭐ Prior allergic-like reaction to same class contrast: ~5-6x ↑ risk.
- Premedication:
| Regimen | Drug | Dose | Route | Timing (Pre-Contrast) |
|---|---|---|---|---|
| Oral | Prednisone | 50mg | PO | 13h, 7h, 1h |
| Diphenhydramine | 50mg | PO/IV | 1h | |
| IV (Emerg.) | Hydrocortisone | 200mg (or Methylprednisolone 40mg) | IV | ASAP, then q4h until procedure |
| Diphenhydramine | 50mg | IV | 1h (or ASAP if urgent) |
Mild to Moderate Mayhem - Calming the Storm
- Always First: STOP contrast, ABCDE assessment, Monitor vitals (BP, HR, SpO2, RR), Reassure patient.
⭐ Most contrast reactions are non-allergic (anaphylactoid) and occur within 5-20 minutes of injection. Always observe patients during this critical window.
Severe Shock Showdown - Code Red Contrast
Anaphylaxis/severe shock post-contrast. 📌 A.S.A.P. I.M. Epi (Alert, Stop contrast, Airway, Position, IM Epinephrine)
- Immediate:
- Stop contrast. Call for HELP (Code Red).
- Airway: High-flow O₂ (10-15 L/min).
- Position: Supine, legs elevated (if hypotensive).
- Meds:
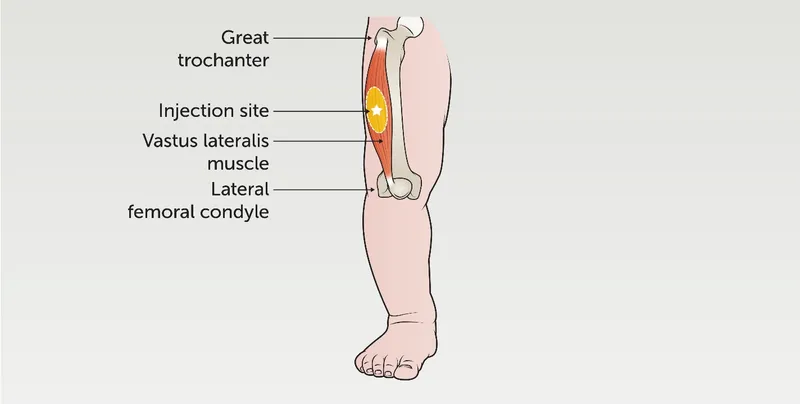
- Epinephrine IM: Adult 0.3-0.5 mg ($1:1000$ solution). Anterolateral thigh. Repeat q5-15min.
- IV Fluids: Normal Saline 1-2 L rapid bolus.
- Antihistamines: Diphenhydramine 25-50 mg IV/IM + Ranitidine 50 mg IV.
- Corticosteroids: Hydrocortisone 100-200 mg IV (prevents biphasic reaction).
- Bronchodilators: Salbutamol nebulized for wheezing.
- Epinephrine IM: Adult 0.3-0.5 mg ($1:1000$ solution). Anterolateral thigh. Repeat q5-15min.
- Refractory Shock:
- IV Epinephrine infusion: $1:10000$ or $1:100000$ dilution. Start 0.1 mcg/kg/min.
- Glucagon 1-2 mg IV (if on β-blockers).
- ICU transfer.
⭐ IM epinephrine (anterolateral thigh) is first-line for anaphylaxis. Delayed administration ↑ mortality.
High‑Yield Points - ⚡ Biggest Takeaways
- Mild reactions (nausea, urticaria): Observation, antihistamines (e.g., diphenhydramine).
- Moderate reactions (diffuse urticaria, bronchospasm): Oxygen, epinephrine (IM/SC), antihistamines, corticosteroids.
- Severe/Anaphylaxis: ABCDE, epinephrine (IM/IV), IV fluids, oxygen, corticosteroids, H1/H2 blockers.
- Epinephrine is key for anaphylaxis: 0.3-0.5 mg (1:1000) IM for adults.
- Pre-treatment for high-risk: Corticosteroids (e.g., Prednisolone) & antihistamines.
- Key risk factors: Previous reaction, asthma, atopy, cardiac disease.
- Delayed reactions (skin rashes) occur hours-days later; manage symptomatically.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more