Basics of Contrast Media - Agent Essentials
- Purpose: Enhance visibility of internal structures.
- Types:
- Positive (radiopaque): ↑ X-ray attenuation.
- Barium Sulfate ($BaSO_4$): GI tract (oral/rectal).
- Iodinated: Vascular, GU, biliary.
- Ionic (HOCM): ↑ Osmolality, ↑ adverse reactions.
- Non-ionic (LOCM/IOCM): ↓ Osmolality, safer. IOCM (e.g., Iodixanol) ≈ 290 mOsm/kg $H_2O$ (iso-osmolar).
- Negative (radiolucent): ↓ X-ray attenuation (Air, $CO_2$).
- Neutral: Bowel distension (Water, Volumen).
- Positive (radiopaque): ↑ X-ray attenuation.
- Key Properties: Atomic number (Z), Concentration, Osmolality, Viscosity. ⭐ > Non-ionic iso-osmolar contrast media (IOCM) like Iodixanol offer the best safety profile, especially regarding CIN.
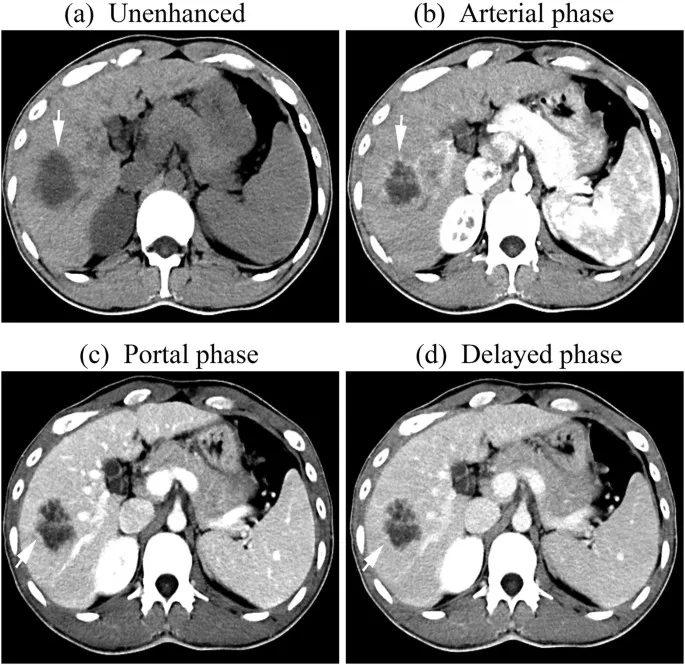
- ⭐ > The portal venous phase (60-90s) is crucial for most routine abdominal CTs, offering optimal solid organ and venous structure enhancement.
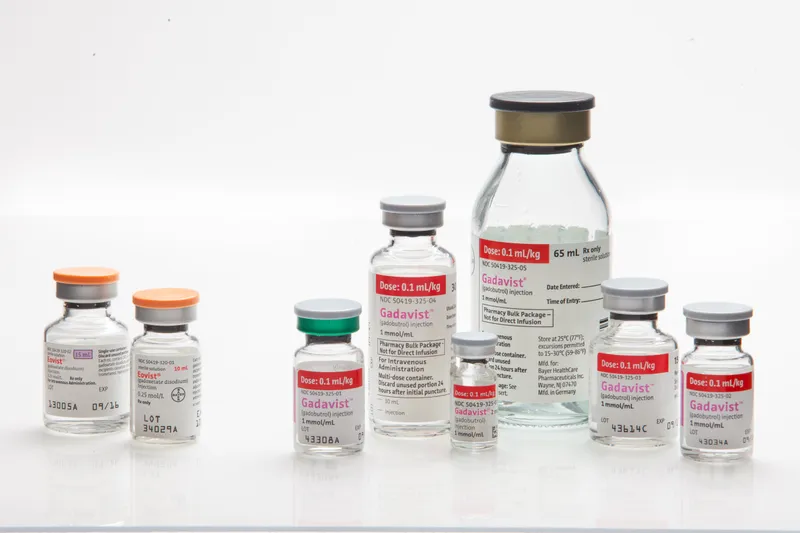
Gadolinium-Based Contrast Agents (GBCA) - MRI Magnet Magic
- Paramagnetic; shorten $T_1$ relaxation, ↑ signal on $T_1$-weighted images.
- Types & Stability:
- Macrocyclic (more stable, preferred): Gadobutrol, Gadoteridol, Gadoterate.
- Linear (less stable, higher NSF risk with some): Gadodiamide, Gadoversetamide.
- Admin: IV. Excretion: Renal.
- ⚠️ Nephrogenic Systemic Fibrosis (NSF):
- Risk with GBCAs in severe renal dysfunction (eGFR < 30 mL/min/1.73m²).
- Especially older, less stable linear agents. Screen eGFR.
- Gadolinium Deposition: Brain (dentate nucleus, globus pallidus), bone, skin; long-term effects studied.
- Precautions: Pregnancy (crosses placenta, use if essential), prior allergic reaction.
⭐ For patients with eGFR < 30 mL/min/1.73m², if GBCA is unavoidable, use lowest dose of a macrocyclic agent and consider prompt dialysis post-MRI in dialysis patients.
Adverse Reactions & Special Considerations - Contrast Safety Net
- Reaction Types & Management:
- Mild: Nausea, urticaria. Tx: Observation, antihistamines.
- Moderate: Bronchospasm, vasovagal. Tx: O2, antihistamines, bronchodilators.
- Severe: Anaphylaxis, arrest. Tx: Epinephrine, ABCs.
- Key Risk Factors: Prior reaction, asthma, eGFR < 30 mL/min/1.73m², metformin.
- Premedication (High-Risk): Corticosteroids (e.g., Prednisolone 50mg PO 13h, 7h, 1h prior) + Antihistamine (e.g., Diphenhydramine 50mg 1h prior).
- Contrast-Induced Nephropathy (CIN):
- Risk ↑ if eGFR < 30 mL/min/1.73m².
- Prevention: Hydration, LOCM/IOCM.
⭐ CIN: Serum creatinine ↑ by > 25% or > 0.5 mg/dL from baseline (48-72h).
- Special Cases:
- Pregnancy: Iodinated if essential; Gadolinium avoided.
- Lactation: Iodinated - consider stopping feeds 12-24h.
- Metformin: Hold; resume 48h post if renal function OK.
- Emergency Cart: Essential & readily available.
High‑Yield Points - ⚡ Biggest Takeaways
- Pre-medicate for prior severe allergic reactions to contrast.
- Check eGFR before iodinated contrast; <30 mL/min/1.73m² is high risk for CIN.
- Hold Metformin for 48h post-contrast if eGFR <60 mL/min/1.73m² or in AKI.
- Adequate hydration (oral/IV) is crucial, especially for at-risk patients.
- Use non-ionic low-osmolar or iso-osmolar contrast media (LOCM/IOCM).
- Manage extravasation with elevation, cold compresses, and observation.
- Iodinated contrast is safe during lactation; gadolinium has minimal breast milk excretion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

