Adverse Reactions to Contrast Media: Introduction & Types - Contrast Reaction Primer
- Adverse reactions: Undesirable effects post-contrast media (CM) administration, ranging from mild to life-threatening.
- Reaction Types:
- Idiosyncratic (Anaphylactoid): Unpredictable, not dose-dependent, mimic allergy.
- Examples: Urticaria, angioedema, bronchospasm, anaphylaxis.
- Non-idiosyncratic (Chemotoxic/Physiologic): Dose-dependent, predictable, due to CM properties.
- Examples: Warmth, nausea/vomiting, vasovagal reaction, CIN, cardiac arrhythmias.
- Idiosyncratic (Anaphylactoid): Unpredictable, not dose-dependent, mimic allergy.
- Major CM Classes:
- Iodinated (X-ray/CT): High Osmolar (HOCM), Low Osmolar (LOCM), Iso-osmolar (IOCM).
- Gadolinium-Based Contrast Agents (GBCAs) for MRI.
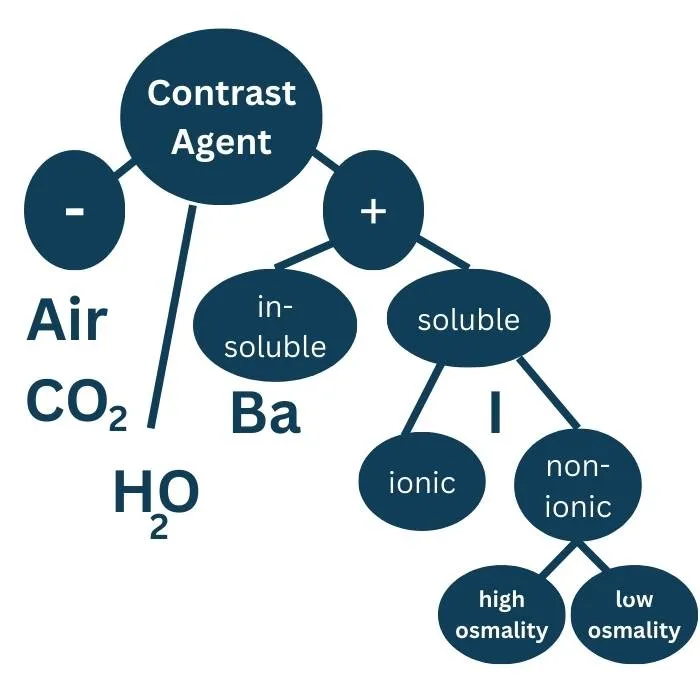
⭐ Non-ionic LOCM show ~5-fold ↓ idiosyncratic reaction risk vs. HOCM.
Adverse Reactions to Contrast Media: Risk Factors & Pathophysiology - Danger Zones Unmasked
-
Key Risk Factors:
- Previous contrast reaction (highest risk)
- Asthma, severe allergies (atopy)
- Renal impairment (e.g., eGFR < 30 mL/min/1.73m² for CIN)
- Cardiac disease (e.g., heart failure)
- Medications: Beta-blockers, NSAIDs, Metformin, IL-2
- Contrast type: HOCM > LOCM > IOCM
-
Pathophysiology:
- Idiosyncratic (Anaphylactoid): Pseudoallergic. Direct mast cell/basophil degranulation. Not IgE-mediated (mostly). Dose-independent.
- Non-idiosyncratic (Chemotoxic): Dose-dependent. Direct organ toxicity (e.g., CIN, cardiac effects). Due to osmolality, viscosity.

⭐ A prior moderate/severe contrast reaction increases repeat reaction risk by ~5-fold.
Adverse Reactions to Contrast Media: Acute Reaction Management - Code Red Contrast
CODE RED: Life-threatening reaction. Activate emergency protocol. Prioritize ABCs.
- Adjunctive Therapy (Post-stabilization/symptom-specific):
- Corticosteroids: Hydrocortisone 100-200 mg IV.
- Antihistamines: Diphenhydramine 25-50 mg IV/IM.
⭐ Epinephrine is the cornerstone for severe anaphylaxis; IM (anterolateral thigh) preferred initially for rapid effect.
Adverse Reactions to Contrast Media: Specific Syndromes & Prevention - Delayed Dangers & Defenses
- Contrast-Induced Nephropathy (CIN)
- Path: AKI post-iodinated contrast. ↑SCr >25% or >0.5 mg/dL from baseline in 48-72 hrs.
- Prevention:
- Hydration: Isotonic saline (0.9% NaCl) 1-1.5 mL/kg/hr pre- & post-procedure.
- Use Low-Osmolar (LOCM) or Iso-Osmolar Contrast Media (IOCM); minimize volume.
- Hold nephrotoxic drugs (e.g., Metformin for 48 hrs if eGFR <60 mL/min/1.73m² or AKI).
- Nephrogenic Systemic Fibrosis (NSF)
- Path: Rare, severe fibrosing disorder post-Gadolinium-Based Contrast Agents (GBCAs) in renal impairment (eGFR <30 mL/min/1.73m²).
- Features: Symmetrical skin thickening, hardening, joint contractures.
- Prevention: Screen eGFR. Avoid high-risk (Group I, linear) GBCAs if eGFR <30. Prefer macrocyclic GBCAs.
⭐ NSF is strongly associated with Group I (linear) GBCAs, like gadodiamide, in patients with eGFR <30 mL/min/1.73m².
- Iodine-Induced Thyroid Dysfunction
- Jod-Basedow effect (hyperthyroidism) or Wolff-Chaikoff effect (hypothyroidism).
- Risk: Pre-existing thyroid disease, iodine deficiency.
- Delayed Cutaneous Reactions
- E.g., maculopapular rash, urticaria; typically 1 hour to 1 week post-contrast.
:max_bytes(150000):strip_icc()/Health-rash-vs-hives-composite-4a286f584cc44609a212e5305b9a0698.jpg)
- E.g., maculopapular rash, urticaria; typically 1 hour to 1 week post-contrast.
High‑Yield Points - ⚡ Biggest Takeaways
- Anaphylactoid: IgE-independent, common. Chemotoxic: dose-dependent.
- Highest risk: Previous moderate/severe reaction. Also asthma, atopy.
- Severe anaphylactoid reactions (bronchospasm, hypotension): Treat with epinephrine.
- CIN: ↑SCr >25% or >0.5 mg/dL in 48-72h. Prevent: IV hydration.
- NSF: Risk with GBCAs (esp. Group I) in severe renal impairment (eGFR <30).
- Premedication (steroids, H1-blockers) for prior moderate/severe reactions.
- Delayed reactions: Cutaneous (maculopapular rash), hours to 1 week later.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

