Other Neurocognitive Disorders - Cognitive Conundrums & Acute Alarms
- Delirium: Acute, fluctuating syndrome of disturbed consciousness, attention, and cognition. A medical emergency.
- 📌 Causes (I WATCH DEATH): Infection, Withdrawal, Acute metabolic, Trauma, CNS pathology, Hypoxia, Deficiencies, Endocrinopathies, Acute vascular, Toxins/Drugs, Heavy metals.
| Feature | Delirium | Major NCD (Dementia) |
|---|---|---|
| Onset | Acute (hours-days) | Insidious (months-years) |
| Course | Fluctuating | Progressive |
| Consciousness | Impaired, clouded | Clear (early) |
| Attention | Markedly impaired | Intact (early) |
| Reversibility | Often reversible | Usually irreversible |
| Sleep-Wake | Disrupted | Variable |
Other Neurocognitive Disorders - Brain Blood Blockades
- Vascular Neurocognitive Disorder (VaD): Cognitive loss from cerebrovascular disease (CVD).
- Types: Multi-infarct, strategic infarct, subcortical (Binswanger's), mixed (VaD+AD).
- Clinical Features:
- Onset: Abrupt, stepwise (multi-infarct) OR gradual (subcortical).
- Focal neurological signs present.
- Executive dysfunction, slow processing prominent.
- Mood: Depression, apathy common.
- Risk Factors:
- HTN, DM, dyslipidemia, smoking, AF, prior stroke/TIA.
- Diagnosis:
- Clinical + CVD evidence (history, signs).
- Neuroimaging: MRI/CT shows infarcts, leukoaraiosis.
- Hachinski Score > 7 supportive.
- Management:
- Control vascular risk factors.

- Control vascular risk factors.
⭐ Stepwise decline classic for multi-infarct; subcortical VaD often gradual with executive dysfunction.
Other Neurocognitive Disorders - Protein Problems & Parkinson's Plus
-
Alpha-synucleinopathies (LBD & PDD): Characterized by Lewy body pathology.
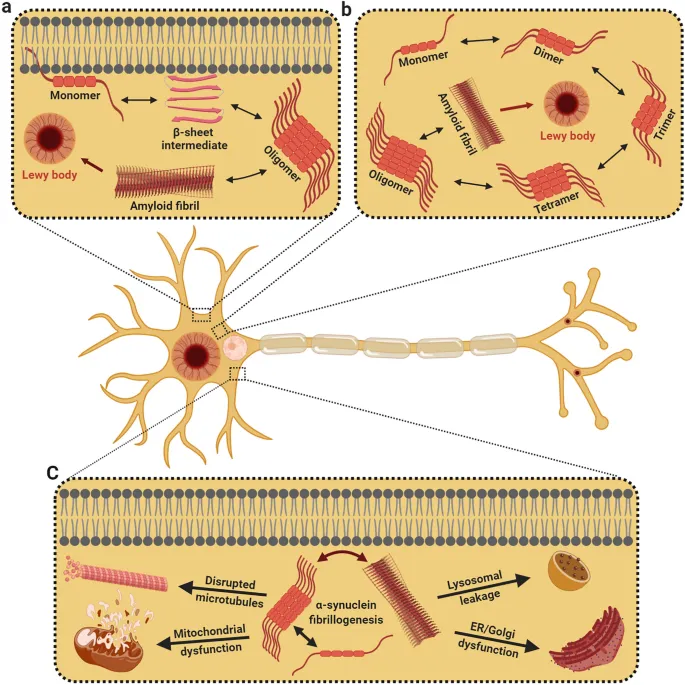
-
Dementia with Lewy Bodies (LBD)
- Core (📌 Foul Play Has Rules):
- Fluctuating cognition (attention/alertness)
- Parkinsonism (spontaneous: bradykinesia, rest tremor, rigidity)
- Hallucinations (recurrent visual)
- REM sleep behavior disorder (RBD)
- Supportive: Severe neuroleptic sensitivity, repeated falls, syncope, autonomic dysfunction.
- Core (📌 Foul Play Has Rules):
-
Parkinson's Disease Dementia (PDD)
- Dementia developing in established Parkinson's Disease.
| Feature | Dementia with Lewy Bodies (LBD) | Parkinson's Disease Dementia (PDD) |
|---|---|---|
| Timing of Onset | Dementia < 1 year before/with parkinsonism (1-year rule) | Dementia > 1 year after motor PD |
| Early Symptoms | Cognitive/psychiatric prominent; VH common | Motor PD symptoms precede cognitive decline |
| Neuroleptic Sens. | High sensitivity common | Less common/severe |
- Other Parkinson's Plus Syndromes:
- PSP: Vertical gaze palsy, postural instability.
- MSA: Autonomic failure, cerebellar signs, parkinsonism.
- CBD: Asymmetric apraxia, alien limb.
Other Neurocognitive Disorders - Frontal Flips & Rare Riddles
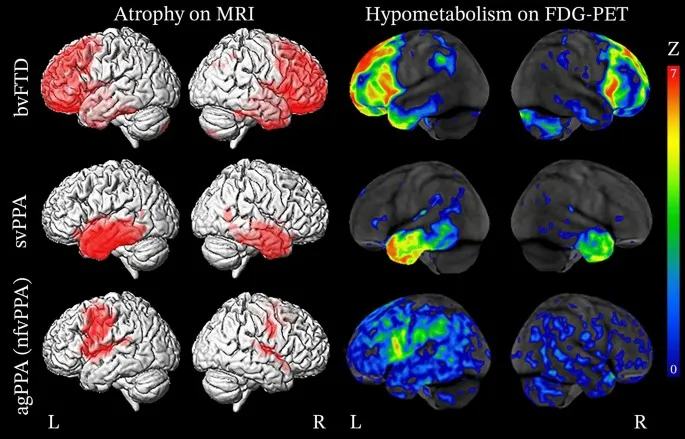
- Frontotemporal Dementia (FTD): Progressive neurodegeneration of frontal and/or temporal lobes.
- Behavioral Variant (bvFTD): Early personality/behavioral changes (disinhibition, apathy, stereotypies), executive dysfunction. Memory relatively spared initially.
⭐ Behavioral variant FTD (bvFTD) often presents with early personality changes and executive dysfunction, with memory relatively spared initially.
- Primary Progressive Aphasia (PPA): Language-led dementias.
- Semantic Variant (svPPA/SD): Loss of word meaning, anomia, impaired object knowledge.
- Nonfluent/Agrammatic Variant (nfvPPA/PNFA): Speech apraxia, agrammatism, effortful speech.
- Behavioral Variant (bvFTD): Early personality/behavioral changes (disinhibition, apathy, stereotypies), executive dysfunction. Memory relatively spared initially.
- Creutzfeldt-Jakob Disease (CJD): Rapidly progressive dementia, myoclonus, ataxia. Prion disease; 14-3-3 protein in CSF.
- Huntington's Disease: Subcortical dementia, chorea, psychiatric symptoms. Autosomal dominant, CAG repeat.
- HIV-Associated Neurocognitive Disorder (HAND): Cognitive, motor, behavioral symptoms in HIV infection. Spectrum from asymptomatic impairment to dementia.
High-Yield Points - ⚡ Biggest Takeaways
- Amnestic NCD: Anterograde amnesia is key; often from thiamine deficiency (Wernicke-Korsakoff) or hypoxia.
- Delirium: Acute onset, fluctuating consciousness, and inattention distinguish from dementia.
- NCD due to TBI: Severity linked to LOC duration; post-concussive symptoms are frequent.
- Substance-Induced NCD: Commonly from alcohol/sedatives; reversibility is possible.
- NCD due to HIV: Features subcortical dementia with motor slowing and apathy.
- CJD: Rapid dementia, myoclonus, characteristic EEG/CSF (14-3-3 protein).
- NPH: Triad: gait apraxia, cognitive decline, urinary incontinence; potentially reversible.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

