Prevention Basics - Laying the Groundwork
- Primary Prevention: Aims to ↓ incidence of new Eating Disorder (ED) cases.
- Targets: General population, high-risk groups (e.g., adolescents, athletes).
- Methods: Psychoeducation on healthy eating & body image, media literacy, promoting self-esteem.
- Secondary Prevention: Focuses on early detection & intervention to ↓ duration & severity.
- Targets: Individuals with early signs/symptoms of EDs.
- Methods: Screening (e.g., SCOFF), prompt referral, early treatment initiation.
- Tertiary Prevention: Aims to reduce relapse, disability & complications in established EDs.
- Targets: Patients with diagnosed EDs.
- Methods: Relapse prevention strategies, managing comorbidities, rehabilitation.
⭐ Universal prevention programs in schools, focusing on media literacy and body acceptance, are crucial for primary prevention of eating disorders.
Risk & Protective Factors - Know Your Battlefield
- Risk Factors:
- Individual: Female gender, adolescence/young adulthood, genetic predisposition (family history), personality traits (e.g., perfectionism, impulsivity, neuroticism), body image dissatisfaction/disturbance, history of dieting, low self-esteem, comorbid anxiety/depression.
- Familial: Parental emphasis on weight/appearance, family history of eating disorders, mood disorders, or substance abuse, critical family environment, parental obesity.
- Socio-cultural: Internalization of societal thin ideal (promoted by media, peers), weight stigma/teasing, participation in aesthetic-focused sports or professions (e.g., gymnastics, modeling).
- Protective Factors:
- Individual: High self-esteem, positive body image, effective coping skills & stress management, assertiveness, critical thinking regarding media messages.
- Familial: Supportive family environment, regular shared family meals, open communication, less parental focus on weight.
- Socio-cultural: Societal acceptance of diverse body shapes and sizes, strong positive peer relationships.
⭐ Family history is a significant risk factor; first-degree relatives of individuals with anorexia nervosa have an approximately 10-fold increased risk of developing the disorder compared to the general population.
Prevention Programs - Action Plans Unveiled
Strategies aim to ↓ risk factors & ↑ protective factors.
- Universal: For entire population.
- School-based: Healthy eating, body positivity.
- Media literacy: Critically analyze media messages.
- Selective: For at-risk groups (e.g., family Hx, athletes).
- Workshops: Body image, self-esteem enhancement.
- Targeted psychoeducation.
- Indicated: For early signs (e.g., weight concerns, initial dieting).
- Cognitive Dissonance (CD) based programs.
- Early screening & brief, focused interventions.
⭐ School-based programs incorporating media literacy, self-esteem building, and peer support are effective in reducing ED risk factors.
Indian Context & Roles - Desi Prevention Angles
- HCPs: Primary care screening (GPs, pediatricians), esp. high-risk. Culturally adapted counseling. Prompt specialist referral.
- Family: Foster healthy, non-dieting eating. Discourage weight-based teasing. Open communication. Body positivity. Recognize early signs.
- Schools: Integrate nutrition & body image education. Peer support programs. Accessible counselors. Anti-bullying measures.
- Media: Promote responsible reporting & diverse body representations. Counter thin-idealization. Public service messages.
- Policy: National prevention strategies. Integrate mental health into primary healthcare. Community awareness drives.
⭐ In India, eating disorders may present atypically or masked by somatic complaints, delaying diagnosis.
- Cultural Nuances: Involve family elders. Use vernacular. Address societal pressures (e.g., marriageability).
High‑Yield Points - ⚡ Biggest Takeaways
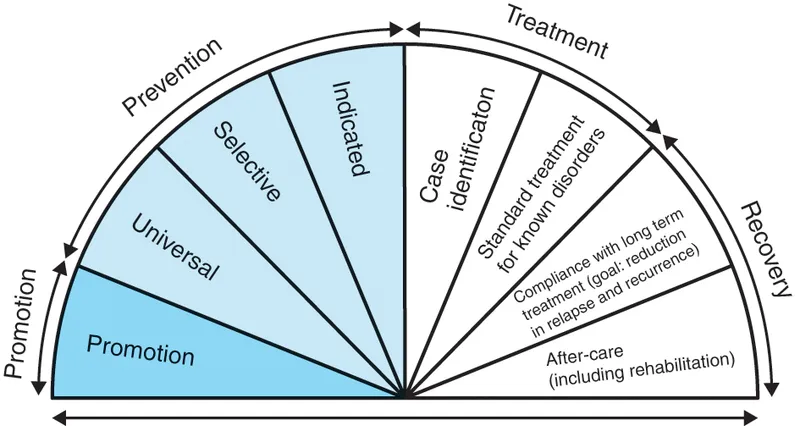
- Universal prevention targets entire populations; selective prevention targets at-risk groups.
- Indicated prevention is for individuals showing early signs of eating disorders.
- Promote media literacy, body positivity, and healthy, balanced eating habits.
- Counteract sociocultural pressures for thinness and weight-related teasing.
- School-based programs are effective for psychoeducation and resilience.
- Early identification and prompt intervention are key to better prognosis.
- Involve families in prevention efforts, especially for adolescents.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

