Psychocardiology - Heart & Mind Link
- Studies interplay between psychological factors & cardiovascular disease (CVD).
- Key Psychological Risk Factors:
- Depression, anxiety disorders (e.g., GAD, Panic).
- Chronic stress, PTSD.
- Type D Personality (distressed: negative affectivity + social inhibition).
- Impact: ↑ CVD incidence & prevalence, poorer prognosis, ↑ cardiac events & mortality.
- Mechanisms:
- Behavioral: Smoking, poor diet, sedentary lifestyle, medication non-adherence.
- Physiological: HPA axis dysregulation, ↑ inflammation (e.g., CRP), autonomic dysfunction, endothelial dysfunction.
⭐ Depression after Myocardial Infarction (MI) significantly increases risk of re-infarction and mortality by 2-2.5 times.
Psychocardiology - Shrink-ing Hearts
- Examines interplay between psychological factors & cardiovascular health (mind-heart connection).
- Key psychological risk factors:
- Depression: ↑ CVD risk & mortality.
- Anxiety disorders: can mimic or exacerbate cardiac symptoms.
- Chronic stress: contributes via HPA axis, inflammation.
- Type D Personality (distressed): negative affectivity, social inhibition.
- Mechanisms: Autonomic dysfunction, ↑ inflammatory markers (e.g., CRP, IL-6), endothelial dysfunction, unhealthy lifestyle choices.
- Specific links:
- Takotsubo cardiomyopathy (stress-induced).
- Post-MI depression (affects ~20% of patients, worsens prognosis).
- Management: Screening, psychotherapy (CBT), psychopharmacology (e.g., SSRIs generally safe post-MI).
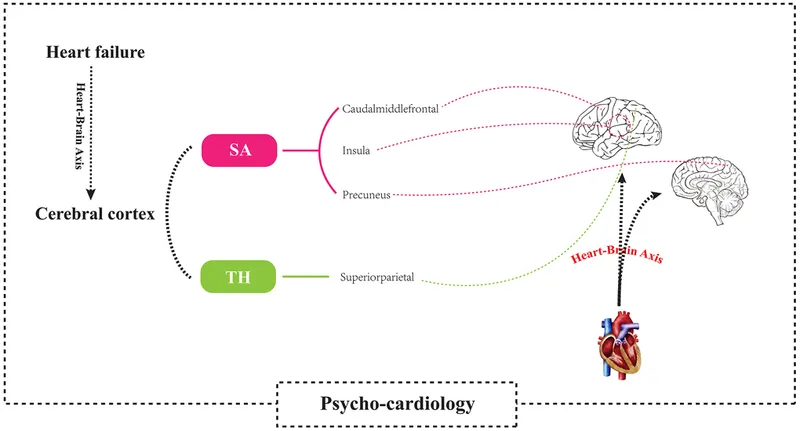
⭐ Depression is an independent risk factor for developing coronary artery disease and is associated with poorer outcomes and increased mortality post-myocardial infarction (MI).
Psychocardiology - Psyche Meds, Heart Effects
- Antipsychotics (APs)
- QTc Prolongation:
- High risk: Thioridazine, Ziprasidone, IV Haloperidol.
- Monitor ECG.
- Orthostatic Hypotension:
- Low-potency FGAs (Chlorpromazine), Risperidone, Clozapine.
- Myocarditis:
- ⚠️ Clozapine (baseline/regular ECG, Troponin, CRP).
- Tachycardia: Clozapine, Olanzapine.
- QTc Prolongation:
- Antidepressants
- TCAs (e.g., Amitriptyline):
- QTc prolongation, orthostatic hypotension, arrhythmias.
- 📌 Tri-Cyclics = Tri-Cardiac effects.
- SSRIs:
- Citalopram (max 40mg), Escitalopram (max 20mg) → QTc prolongation.
- SNRIs (Venlafaxine): ↑BP, ↑HR.
- TCAs (e.g., Amitriptyline):
- Mood Stabilizers
- Lithium: T-wave changes, bradycardia, SA dysfunction.
- Carbamazepine: Bradycardia, AV block.
- Stimulants
- Methylphenidate, Amphetamine: ↑BP, ↑HR.
⭐ Clozapine carries a risk of myocarditis, typically in first 2 months of treatment; monitor with ECG, troponin, and CRP.
Psychocardiology - Broken Hearts, Troubled Minds
- Bidirectional link: heart disease ↔ mental health. Focus: psychiatric sequelae in cardiac patients.
- Common: Depression (20-40% post-MI), Anxiety (GAD, Panic), PTSD (post-MI/CABG), Delirium.
- Impact: ↑ morbidity & mortality, ↓ QoL & adherence.
- Key Syndromes:
- Takotsubo Cardiomyopathy ("Broken Heart Syndrome"): Acute stress-induced.
- Type D Personality: Negative affectivity, social inhibition → poor cardiac prognosis.
- Management: Screening, psychotherapy (CBT), SSRIs (cardiac safety crucial), lifestyle changes.
⭐ Depression is an independent risk factor for adverse cardiovascular outcomes in patients with established heart disease.
Psychocardiology - Healing Heart & Soul
- Interface of cardiology & psychiatry; manages psychological distress in cardiac patients.
- Common conditions: Depression (post-MI), anxiety disorders, Type D personality (distressed).
- Impact: Affects medication adherence, Quality of Life (QoL), morbidity, & mortality.
- Management:
- Pharmacotherapy: SSRIs (e.g., Sertraline, Escitalopram) generally safe.
- Psychotherapy: Cognitive Behavioral Therapy (CBT), supportive therapy.
- Lifestyle: Stress management, cardiac rehabilitation.
⭐ Depression is an independent risk factor for adverse cardiovascular outcomes, including mortality, especially post-Myocardial Infarction (MI).
High‑Yield Points - ⚡ Biggest Takeaways
- Depression is an independent risk factor for CAD and worsens post-MI prognosis.
- Anxiety disorders, especially panic disorder, can mimic cardiac symptoms.
- SSRIs (e.g., Sertraline) are first-line antidepressants in cardiac patients due to cardiac safety.
- TCAs and some antipsychotics risk QTc prolongation and arrhythmias.
- Takotsubo cardiomyopathy is precipitated by intense emotional/physical stress.
- Type D personality (negative affectivity, social inhibition) is linked to poorer cardiovascular outcomes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


