Ventilation Dynamics - Breath Power Up
- Minute Ventilation ($V_E$) = Tidal Volume ($V_T$) × Respiratory Rate ($f_R$).
- Resting $V_E$ ≈ 5-8 L/min.
- During exercise, $V_E$ ↑ significantly:
- Initially, ↑ $V_T$ (up to ~50-60% of Vital Capacity).
- At higher intensities, ↑ $f_R$ (can reach 40-50 breaths/min; >60 in elite athletes) becomes the primary driver as $V_T$ plateaus.
- Overall $V_E$ can increase 15-25 times resting values.
- Ventilatory Threshold (VT): The point during incremental exercise where $V_E$ begins to ↑ out of proportion to the ↑ in oxygen consumption ($V_{O_2}$).
- Often linked to the lactate threshold.

⭐ During maximal, strenuous exercise, $V_E$ can reach values exceeding 100 L/min, and in elite endurance athletes, it can be over 200 L/min.
Control Mechanisms - Lungs on Command

- Neural Control (Rapid Onset):
- Central Command: Feedforward from motor cortex & hypothalamus; anticipatory ↑ ventilation.
- Peripheral Reflexes: Afferents from muscle mechanoreceptors (e.g., spindles) & metaboreceptors (e.g., K⁺, H⁺).
- Humoral Control (Slower Adjustment & Fine-tuning):
- Peripheral Chemoreceptors (Carotid/Aortic Bodies): Sense ↓ PaO₂, ↑ PaCO₂, ↑ [H⁺].
- Central Chemoreceptors (Medulla): Sense ↑ CSF [H⁺] (indirectly from ↑ PaCO₂).
- Other factors: ↑ Body temperature, ↑ catecholamines.
- Integration: Respiratory centers in medulla & pons process inputs.
⭐ Central command can increase ventilation within seconds of exercise onset, even before changes in blood gases are detected by chemoreceptors.
Gas Exchange - Oxygen Express
- ↑ Alveolar Ventilation ($V_A$): Boosts O₂ supply to alveoli.
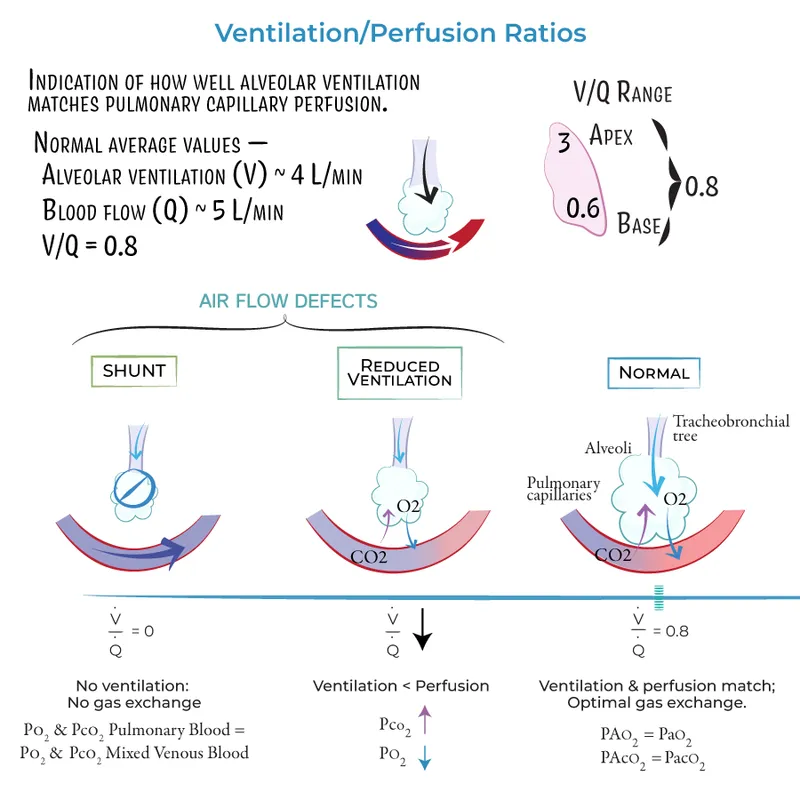
- Improved V/Q Matching:
- Better perfusion of lung apices; more uniform V/Q ratio throughout the lungs.
- ↑ Diffusion Capacity ($DL_{O2}$):
- Up to 3x increase from rest to maximal exercise.
- Due to ↑ capillary recruitment (↑ surface area) & ↑ pulmonary capillary blood volume.
- O₂-Hb Dissociation Curve Shift:
- Rightward shift (Bohr effect: ↑Temperature, ↑PCO₂, ↓pH) enhances O₂ unloading at active tissues.
- Alveolar-Arterial O₂ Gradient ($P(A-a)O_2$):
- Rest: $5-10 \text{ mmHg}$.
- Exercise: May widen ($>\textbf{20} \text{ mmHg}$), especially in elite athletes, due to diffusion limitation and very short RBC transit times.
⭐ Exercise-Induced Arterial Hypoxemia (EIAH) can occur in some highly trained athletes, where $PaO_2$ falls significantly (e.g., by $>\textbf{10-15} \text{ mmHg}$) during maximal exercise.
 oka
oka
Limits & Training - Beyond the Breath

- Ventilatory Limits:
- Ventilatory Thresholds (VT1, VT2/RCP): Ventilation ↑ disproportionately to $V_O2$.
- Exercise-Induced Arterial Hypoxemia (EIAH): $PaO_2$ ↓ > 10-15 mmHg; elite athletes; V/Q mismatch, diffusion limits at high Cardiac Output.
- Respiratory muscle fatigue: Limits prolonged, intense exercise.
- Training Adaptations:
- ↑ Respiratory muscle strength & endurance.
- ↓ $V_E/V_O2$ at submaximal exercise (↑ efficiency).
- Delayed onset of VT and OBLA (Onset of Blood Lactate Accumulation).
- ↑ Maximal sustainable ventilation ($V_{Emax}$).
- Static lung volumes (FVC, FEV1) largely unchanged.
⭐ Highly trained: respiratory system (diffusion capacity) can limit $V_{O2max}$ ("pulmonary ceiling").
High‑Yield Points - ⚡ Biggest Takeaways
- Ventilation (VE) ↑ linearly with VO2, then disproportionately above ventilatory threshold (VT).
- Tidal Volume (TV) plateaus; further VE ↑ relies on Respiratory Rate (RR) at high intensities.
- Pulmonary diffusion capacity (DLCO) ↑ due to ↑ pulmonary blood flow & capillary recruitment.
- Arterial PO2 (PaO2) is maintained; may ↓ in elite athletes (EIAH).
- Arterial PCO2 (PaCO2) ↓ at high intensities due to compensatory hyperventilation.
- Training ↓ VE at submaximal workloads & ↑ maximal sustainable ventilation (MSV).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

