Fatigue Fundamentals - Defining the Drain
- Exercise-Induced Fatigue: Reversible ↓ in force/power output or task performance.
- Classification:
- Central Fatigue: CNS origin (Brain, Spinal Cord).
- Mechanism: ↓ neural drive to muscles; altered neurotransmission (e.g., serotonin, dopamine).
- Peripheral Fatigue: Muscle/NMJ origin.
- Sites: NMJ, sarcolemma, T-tubules, SR, contractile proteins.
- Mechanism: Impaired muscle cell function (e.g., E-C coupling, ATP supply).
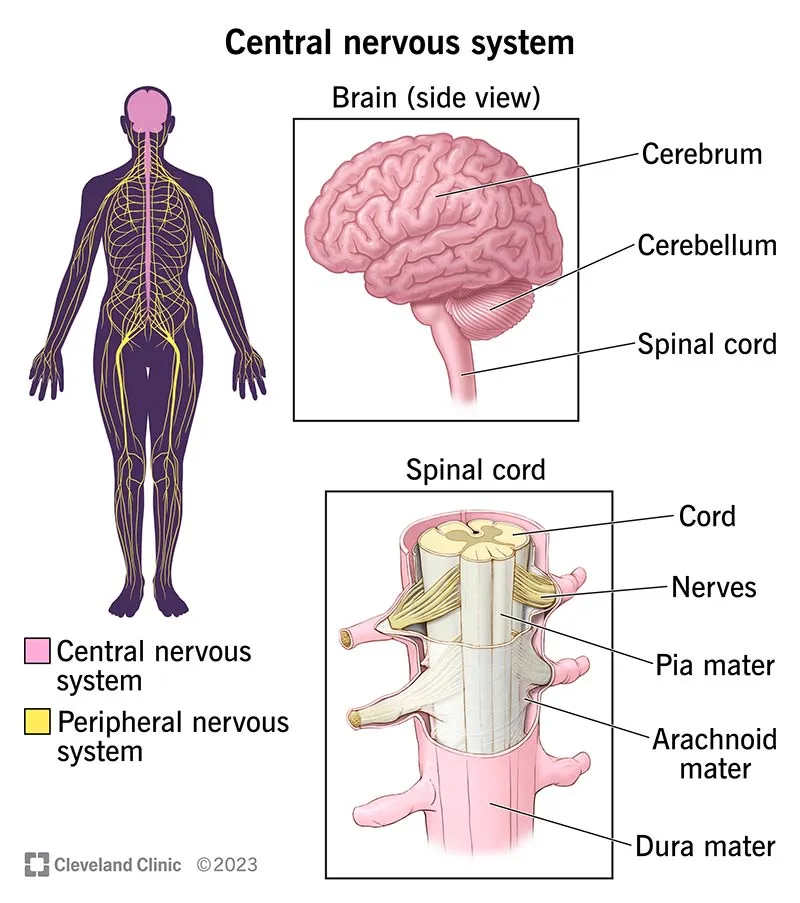 vs Peripheral fatigue (NMJ/Muscle Fiber) sites diagram)
vs Peripheral fatigue (NMJ/Muscle Fiber) sites diagram)
- Central Fatigue: CNS origin (Brain, Spinal Cord).
⭐ Central fatigue involves decreased voluntary activation of muscles, often influenced by psychological factors and brain neurotransmitter changes.
Brain's Burden - Central Command Quits
- Neurotransmitter Shifts:
- ↑ Serotonin (5-HT)/Tryptophan ratio: Promotes fatigue. 📌 Serotonin SLOWS.
- ↓ Dopamine: Reduces motivation/drive. 📌 Dopamine DRIVES.
- Acetylcholine: Central roles beyond NMJ.
- BCAAs: Branched-Chain Amino Acids compete with tryptophan for brain entry, may ↓ central fatigue.
- Afferent Signals: Group III/IV muscle afferents signal metabolic stress (e.g., H⁺, K⁺) to CNS, inhibiting central motor drive.
- Energy Crisis: Hypoglycemia impairs CNS function, ↓ arousal & motor output.
- Psychological Factors: Perceived exertion (RPE), motivation, cognitive state modulate fatigue.
⭐ Central fatigue is significantly influenced by an increased brain serotonin (5-HT) to dopamine ratio, affecting mood and drive.
Muscle Muddle - Peripheral Power‑Failures

- Energy Substrate Depletion:
- ATP-PCr: Rapidly depleted (<30s) in maximal intensity efforts. $PCr + ADP + H^+ \rightleftharpoons ATP + Cr$
- Glycogen: Muscle stores vital for prolonged/high-intensity exercise; liver glycogen maintains blood glucose.
- Metabolic Byproduct Accumulation:
- $H^+$ ions: From ATP hydrolysis & glycolysis. ↓pH; inhibits PFK, glycogen phosphorylase; ↓Ca²⁺ binding to troponin C.
- $P_i$ (Inorganic Phosphate): From ATP/PCr breakdown. Impairs SR Ca²⁺ release; ↓myofibrillar Ca²⁺ sensitivity & cross-bridge force.
- Lactate: Not direct fatigue cause; co-accumulates with $H^+$; can be a fuel source.
- ROS (Reactive Oxygen Species): Exercise-induced; high levels impair enzyme function & E-C coupling.
- Excitation-Contraction (E-C) Coupling Failure:
- NMJ (Neuromuscular Junction): ↓ACh release or sensitivity (rarely limiting in healthy individuals).
- Sarcolemma excitability: Altered $Na^+/K^+$ pump activity; $K^+$ accumulation in T-tubules; impaired AP propagation.
- SR $Ca^{2+}$ Handling: ↓$Ca^{2+}$ release (e.g., $P_i$, ROS effects); impaired $Ca^{2+}$ reuptake by SERCA.
⭐ $P_i$ accumulation is a key factor in fatigue during high-intensity exercise, directly impairing both SR Ca²⁺ release and cross-bridge force production.
Fatigue Factors & Fixes - Modulating Mechanisms
- Exercise Characteristics:
- Intensity: High (↑$P_i$, ↓pH) vs. Prolonged (↓glycogen). Critical Power concept.
- Duration: Longer → ↑substrate depletion, ↑dehydration, ↑hyperthermia.
- Type: Endurance (central, metabolic) vs. Sprint/Strength (peripheral: $P_i$, $H^+$).
- Environmental Factors:
- Heat Stress: ↑Glycogenolysis, ↑CV strain, ↑dehydration; hyperthermia → central fatigue.
- Altitude (Hypoxia): ↓$O_2$ availability → impairs aerobic ATP, earlier fatigue.
- Individual Status:
- Training: Adaptations (↑mitochondria, ↑capillarization, ↑glycogen, ↑buffering) delay fatigue.
- Nutrition: Pre-exercise CHO & hydration levels vital. Ergogenic aids (e.g., caffeine, creatine) may aid.
⭐ Critical Power is the highest exercise intensity sustainable primarily by aerobic metabolism before fatigue rapidly ensues.
High‑Yield Points - ⚡ Biggest Takeaways
- Central fatigue: CNS-mediated ↓ neural drive to muscles, influenced by psychological factors.
- Peripheral fatigue: Impairment at the muscle fiber level, including E-C coupling and NMJ.
- Glycogen depletion: Critical in prolonged exercise, limits ATP resynthesis via glycolysis.
- H+ accumulation (lactic acidosis): Inhibits key enzymes (e.g., PFK) and Ca2+ binding to troponin.
- Pi accumulation (ATP hydrolysis): Impairs cross-bridge function (power stroke) & SR Ca2+ handling.
- K+ accumulation (extracellular): Depolarizes sarcolemma, reducing muscle fiber excitability and force output.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

