Definition & Scope - Pill Overload Perils
- Polypharmacy: Simultaneous use of multiple medications.
- Commonly defined as ≥5 drugs.
- Major polypharmacy: ≥10 drugs.
- Scope: Highly prevalent in elderly due to multiple chronic conditions, a key geriatric challenge.
- Pill Overload Perils:
- ↑ Risk of Adverse Drug Reactions (ADRs) & drug-drug interactions (DDIs).
- ↓ Medication adherence.
- Risk of prescribing cascades.
- ↑ Healthcare utilization & costs.
- ↑ Geriatric syndromes (e.g., falls, frailty, cognitive decline).
⭐ Inappropriate polypharmacy is a major contributor to hospital admissions in the elderly.
Age-Related Changes & Drugs - Age-Altered Actions
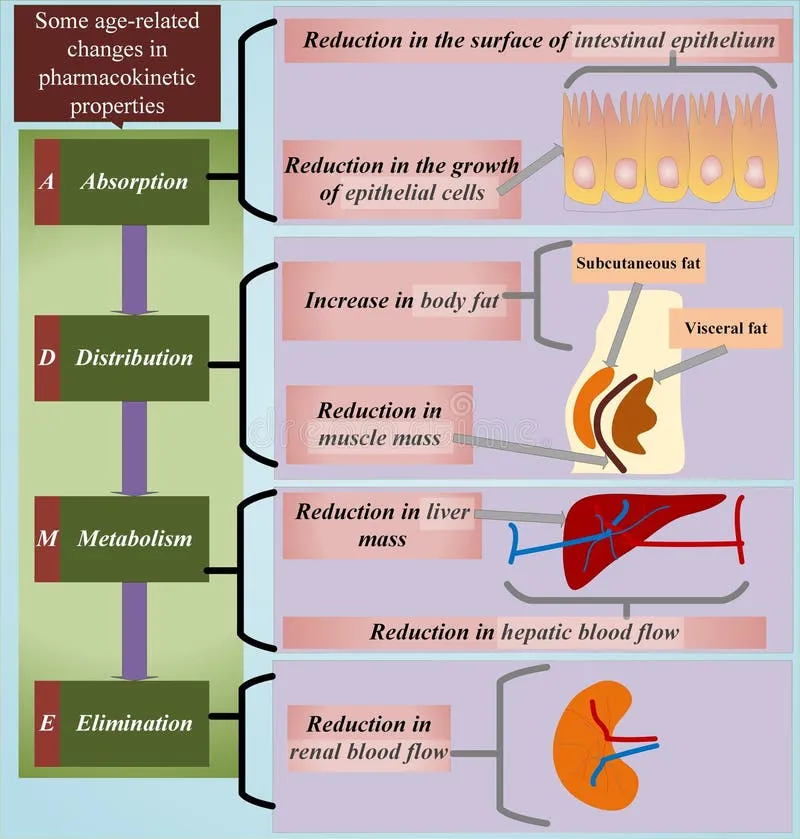
Pharmacokinetic (PK) Changes:
| PK Parameter | Change in Elderly | Implication |
|---|---|---|
| Absorption | Variable; ↓ gastric acid/motility | Often minor clinical impact |
| Distribution | ↓ Body water/albumin; ↑ Body fat | ↑ Conc. water-soluble drugs; ↑ free acidic drugs; ↑ Vd lipid-soluble drugs |
| Metabolism | ↓ Hepatic blood flow, ↓ Phase I (CYP450) | ↓ Clearance (e.g., diazepam); Phase II preserved |
| Excretion | ↓ GFR, ↓ Renal blood flow ($CrCl \downarrow$) | Accumulation of renal drugs (e.g., digoxin, aminoglycosides) |
Pharmacodynamic (PD) Changes:
- ↑ Sensitivity: Benzodiazepines, opioids, anticholinergics, warfarin.
- ↓ Response: β-blockers, β-agonists.
- ↑ Risk: Orthostatic hypotension, CNS effects.
⭐ Elderly show ↑ sensitivity to benzodiazepines: ↑ risk of falls, confusion, sedation.
 in elderly and impact on drug levels)
in elderly and impact on drug levels)
Risks & Consequences - The Domino Effect
- Increased Adverse Drug Reactions (ADRs): Each added drug exponentially ↑ ADR risk.
- Drug-Drug Interactions (DDIs): Synergistic/antagonistic effects, altered metabolism.
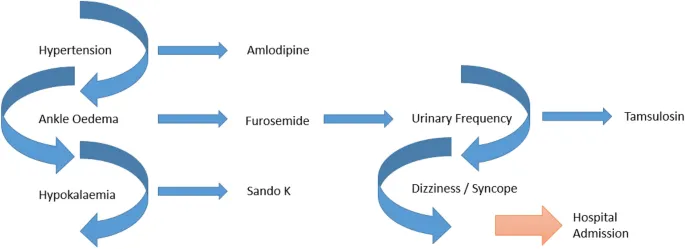
- Prescribing Cascade: An ADR is misinterpreted as a new medical condition, leading to another prescription. (Illustrated below)
- Non-Adherence: Complex regimens (≥5 drugs often cited) ↓ compliance, ↑ errors.
- Functional Decline: ↑ Falls (major risk), confusion, frailty, leading to ↓ ADLs.
- Cognitive Impairment: Especially with anticholinergics, sedatives (📌 BEERS list).
- Increased Morbidity, Mortality & Hospitalizations.
- Higher Healthcare Costs: Due to drugs, managing ADRs, hospital stays.
⭐ The "prescribing cascade" is a key domino effect: an adverse drug reaction is mistaken for a new illness, prompting further prescriptions and escalating polypharmacy.
Prevention & Management - Smart Prescribing Strategies
- Key Strategies:
- Regular medication review (e.g., "brown bag review") at each visit or annually.
- Apply Beers Criteria, STOPP/START tools.
- Avoid prescribing cascades (treat side effects with more drugs).
- "Start low, go slow."
- Prioritize non-pharmacological options.
- Shared decision-making with patient.
⭐ STOPP (Screening Tool of Older Persons' Prescriptions) criteria aim to reduce Potentially Inappropriate Prescriptions (PIPs), while START (Screening Tool to Alert to Right Treatment) criteria aim to identify indicated medications that are omitted in elderly patients.
High‑Yield Points - ⚡ Biggest Takeaways
- Polypharmacy is defined as the concurrent use of ≥5 medications, common in elderly.
- Significantly ↑ risk of Adverse Drug Reactions (ADRs), drug-drug interactions, and non-adherence.
- Primarily driven by multiple comorbidities and age-related pharmacokinetic/pharmacodynamic alterations.
- Beware of the prescribing cascade, where new drugs treat side effects of others.
- Essential management includes regular medication review and deprescribing inappropriate medications.
- Employ tools like Beers Criteria and STOPP/START criteria for optimization_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

