Thrombolysis Basics - Clot Busters 101
- Goal: Rapidly dissolve intravascular thrombi (clots) to restore perfusion & limit infarct size.
- Mechanism: Convert inactive Plasminogen $\rightarrow$ active Plasmin.
- Plasmin degrades fibrin (clot matrix) $\rightarrow$ Fibrin Degradation Products (FDPs).
- "Clot Busters": Drugs that achieve this enzymatic conversion.
- Key Principle: "Time is tissue" - earlier administration yields better outcomes.
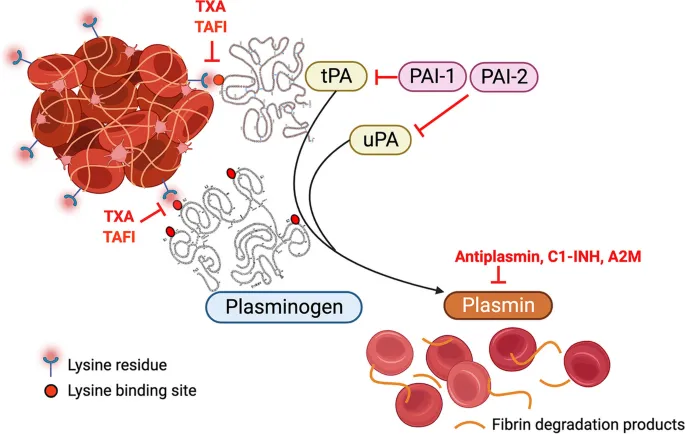
⭐ The primary goal of thrombolysis is the rapid restoration of blood flow to ischemic tissue, thereby minimizing organ damage.
The Drug Arsenal - Clot-Dissolving Crew
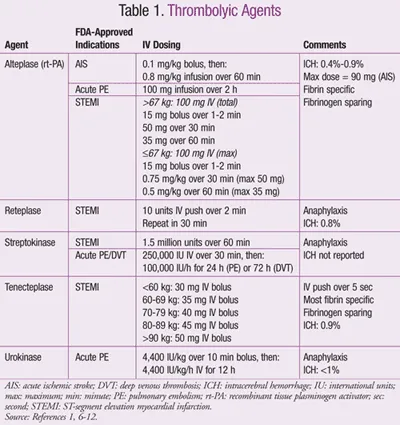
These drugs dissolve clots by activating plasminogen to plasmin, which degrades fibrin. Common agents: 📌 SUART (Streptokinase, Urokinase, Alteplase, Reteplase, Tenecteplase).
| Agent | Generation | Fibrin Specificity | Half-life (IV) & Dosing | Antigenicity | Cost |
|---|---|---|---|---|---|
| Streptokinase (SK) | 1st | Low (non-specific, systemic lysis) | ~20-30 min (infusion) | High (allergic reactions, prior exposure issues) | Lowest |
| Urokinase (UK) | 1st | Low (non-specific, systemic lysis) | ~15-20 min (infusion) | Low (human source, less than SK) | Moderate |
| Alteplase (t-PA) | 2nd | High (clot-specific) | ~4-6 min (bolus + infusion) | Low (recombinant human t-PA) | High |
| Reteplase (r-PA) | 3rd | Moderate (better fibrin penetration) | ~13-16 min (double bolus) | Low (recombinant) | High |
| Tenecteplase (TNK-tPA) | 3rd | Higher (most specific, PAI-1 resistant) | ~20-24 min (single bolus) | Low (recombinant) | Highest |
When to Bust Clots - Emergency Go-Signals
Key indications for thrombolysis:
- ST-Elevation Myocardial Infarction (STEMI)
- Symptom onset <12 hours (ideal: <3 hours).
- ECG: ST ↑ in ≥2 contiguous leads.
- Acute Ischemic Stroke (AIS)
- Symptom onset <4.5 hours.
- Disabling neurological deficit.
- CT excludes hemorrhage.
- BP <185/110 mmHg.
- Massive Pulmonary Embolism (PE)
- Life-threatening: Sustained hypotension (e.g., SBP <90 mmHg).
- Or cardiac arrest.
⭐ 'Time is Brain' in acute ischemic stroke and 'Time is Muscle' in STEMI; efficacy of thrombolysis is highly time-dependent.
AIS Thrombolysis Pathway:
Danger Zones & Pitfalls - Clot Busting Risks
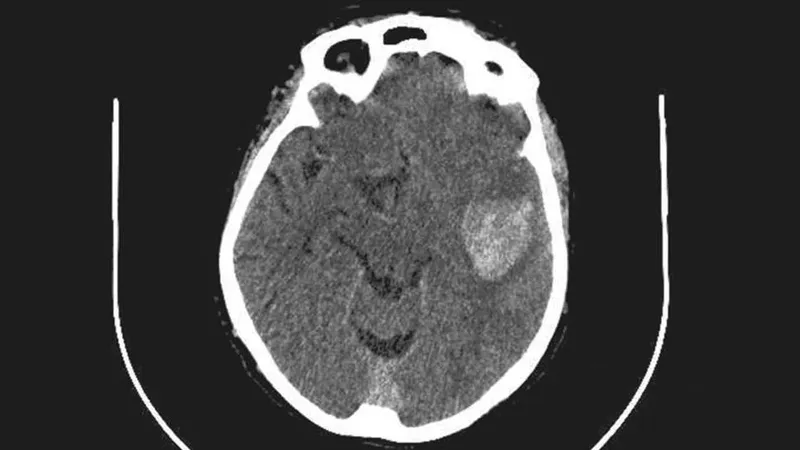 Key Risks: Bleeding (ICH most feared), allergic reactions, hypotension.
Key Risks: Bleeding (ICH most feared), allergic reactions, hypotension.
-
Absolute Contraindications (⚠️ High Risk):
- Any prior Intracranial Hemorrhage (ICH); known cerebral AVM/neoplasm
- Ischemic stroke within 3 months (unless current acute stroke <4.5h)
- Suspected aortic dissection
- Active bleeding (excluding menses); significant bleeding disorder
- Significant head/facial trauma within 3 months
- Intracranial/intraspinal surgery within 2 months
- Severe uncontrolled hypertension (e.g., BP >185/110 mmHg for stroke; >180/110 mmHg for MI/PE if unresponsive)
-
Relative Contraindications (Caution Advised):
- Age >75 years
- Current anticoagulant use (e.g., Warfarin with INR >1.7)
- Recent major surgery (<3 weeks)
- Recent internal bleeding (2-4 weeks)
- Pregnancy
- Severe, chronic, poorly controlled hypertension history
⭐ Intracranial hemorrhage (ICH) is the most feared and life-threatening complication of thrombolytic therapy.
High‑Yield Points - ⚡ Biggest Takeaways
- Thrombolytics (e.g., Alteplase, Tenecteplase) convert plasminogen to plasmin, dissolving fibrin clots.
- Key indications: STEMI (within 12h), ischemic stroke (within 3-4.5h), massive PE.
- Major contraindications: Active bleeding, recent major surgery/trauma, prior ICH, severe uncontrolled HTN.
- Most feared complication: Intracranial Hemorrhage (ICH); monitor for neurological changes.
- Streptokinase: Antigenic, risk of hypotension and allergic reactions.
- Observe for reperfusion signs (e.g., arrhythmias in MI) and bleeding manifestations post-administration.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

