DIKI: Intro & Mechanisms - Kidney Under Siege
- Drug-Induced Kidney Injury (DIKI): Adverse renal events from drugs/diagnostic agents, impairing kidney function. Often reversible if detected early.
- Primary Mechanisms:
- Altered Hemodynamics: NSAIDs, ACEi affect renal blood flow/filtration.
- Acute Tubular Necrosis (ATN): Direct tubular cell toxicity (aminoglycosides, contrast).
- Acute Interstitial Nephritis (AIN): Allergic inflammation (penicillins, PPIs).
- Crystal Nephropathy: Drug precipitation in tubules (sulfonamides, acyclovir).
- Osmotic Nephrosis: High osmolar agents, tubular swelling (mannitol).
⭐ Acute Tubular Necrosis (ATN) is the most common form of drug-induced kidney injury.
DIKI: Culprit Drugs - Nephrotox Hit Parade
| Drug/Class | Common DIKI Pattern(s) | Key Mechanism/Notes |
|---|---|---|
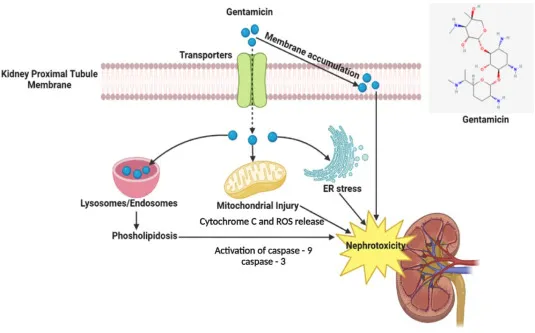
| Aminoglycosides | ATN (non-oliguric) | Proximal tubule damage; accumulation; delayed. |
| NSAIDs | AIN, Papillary Necrosis, Hemodynamic AKI | ↓PGE₂ (afferent constrict.); hypersensitivity. |
| ACEi/ARBs | Hemodynamic AKI | Efferent dilation (↓GFR); risk: RAS, dehydration. |
| Contrast Media | ATN (CIN) | Direct toxicity, vasoconstriction, ROS. Hydrate. |
| Amphotericin B | ATN, Distal RTA, ↓K⁺, ↓Mg²⁺ | Direct tubular damage; vasoconstriction. Dose-related. |
| Cisplatin | ATN, ↓Mg²⁺ | Proximal tubule injury. Cumulative. Amifostine. |
| Vancomycin | AIN (often with pip-tazo), ATN (rare) | Immune (AIN); "cast nephropathy". Troughs. |
| Sulfonamides | AIN, Crystal Nephropathy | Hypersensitivity; drug precipitation. Hydrate. |
| Acyclovir (IV) | Crystal Nephropathy | Tubular precipitation. Risk: dehydration, rapid IV. |
| Tenofovir (TDF) | Proximal Tubulopathy (Fanconi) | Mitochondrial toxicity. TAF safer. |
DIKI: Clinical & Diagnosis - Detective Work DIKI
- History is Key: Meticulous drug history (timing, dose, recent changes).
- Clinical Clues: Often asymptomatic. May see ↑SCr, oliguria.
- AIN: Fever, rash, arthralgia, eosinophilia.
- ATN: Muddy brown casts.
- Investigations:
- Urinalysis: Proteinuria, hematuria, specific casts.
- Urine Eosinophils: For suspected AIN.
- Serum Creatinine: Monitor trends (e.g., rise of ≥0.3 mg/dL or ≥50% from baseline).
- Renal Ultrasound: Rule out obstruction.
- Kidney Biopsy: Gold standard if diagnosis unclear.
⭐ Eosinophiluria is a classic, though not pathognomonic (found in ~70% cases), finding in drug-induced Acute Interstitial Nephritis (AIN).
DIKI: Management & Prevention - Kidney Guardian Guide
- General Management:
- Discontinue offending drug(s) immediately.
- Optimize hemodynamics: ensure adequate hydration (IV fluids if needed).
- Correct electrolyte imbalances (e.g., hyperkalemia).
- Adjust dosages of other renally excreted drugs.
- Renal replacement therapy (RRT) if severe (e.g., uremic symptoms, refractory hyperkalemia/acidosis).
- Prevention Strategies:
- Identify high-risk patients (e.g., pre-existing CKD, elderly, diabetes, volume depletion).
- Avoid nephrotoxic drug combinations.
- Ensure adequate hydration, especially before/after contrast media or nephrotoxic drugs.
- Monitor renal function (serum creatinine, eGFR, urine output) regularly.
- Use a_lternative non-nephrotoxic agents when possible.
⭐ For preventing Contrast-Induced Nephropathy (CIN), isotonic saline hydration is key; N-acetylcysteine use is controversial but sometimes considered.
High‑Yield Points - ⚡ Biggest Takeaways
- Acute Tubular Necrosis (ATN) is the most common DIKI, often from aminoglycosides, contrast media, and cisplatin.
- Acute Interstitial Nephritis (AIN) is an allergic reaction (e.g., penicillins, NSAIDs, PPIs), presenting with eosinophilia, rash, and fever.
- Prerenal AKI can be induced by ACE inhibitors/ARBs or NSAIDs (by ↓ prostaglandin synthesis).
- Chronic Interstitial Nephritis is linked to long-term lithium or analgesic abuse (e.g., phenacetin).
- Crystalline Nephropathy may be caused by drugs like acyclovir, sulfonamides, and methotrexate.
- Rhabdomyolysis (e.g., from statins, especially with fibrates) can also precipitate AKI by myoglobinuria.
- Key diagnostic clues include temporal drug exposure, urinalysis findings (muddy brown casts in ATN, WBC casts/eosinophiluria in AIN), and renal function tests (↑ serum creatinine, ↑ BUN).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

