Classification & Targets - Lipid Landscape
-
Dyslipidemia Types:
- Hypercholesterolemia: Elevated LDL-C
- Hypertriglyceridemia: Elevated TG
- Mixed Dyslipidemia: Elevated LDL-C & TG
-
Lipoprotein Classes & Apolipoproteins:
- Chylomicrons (CM): Transport dietary TGs; ApoB-48.
- VLDL: Transports endogenous TGs; ApoB-100.
- IDL: VLDL remnant; precursor to LDL.
- LDL ("Bad"): Major cholesterol carrier to tissues; ApoB-100.
- HDL ("Good"): Reverse cholesterol transport; ApoA-I.
| Drug Class | Primary Target | Key Effect(s) |
|---|---|---|
| Statins | HMG-CoA Reductase | LDL↓↓, HDL↑, TG↓ |
| Fibrates | PPAR-α activation | TG↓↓, HDL↑, LDL↔/↓ |
| Niacin | ↓VLDL production, ↓Lipolysis | LDL↓, HDL↑↑, TG↓ |
| Bile Acid Sequestrants | Bind bile acids (intestine) | LDL↓, HDL↔, TG↑ (⚠️) |
| Cholesterol Absorp. Inhib. | NPC1L1 (gut) | LDL↓ |
| PCSK9 Inhibitors | PCSK9 | LDL↓↓ |
Statins - Plaque Busters
- Mechanism (MoA): HMG-CoA reductase inhibitors.
- Inhibit cholesterol synthesis (rate-limiting step).
- Upregulate hepatic LDL receptors → ↑ LDL clearance.
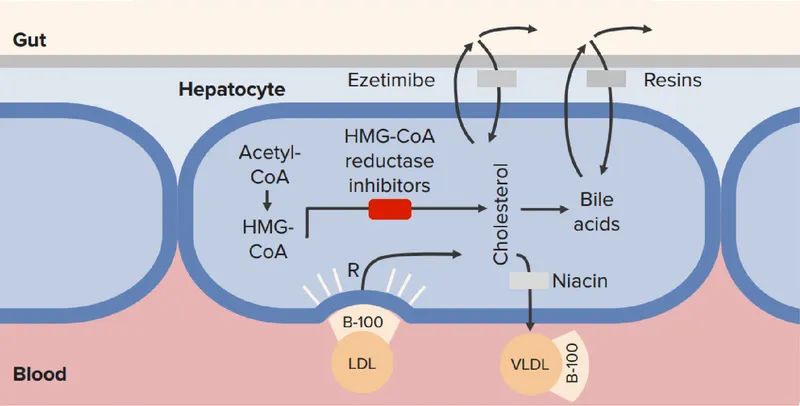
- Pleiotropic Effects: Anti-inflammatory, plaque stabilization, improved endothelial function.
- Key Statins & Doses:
Intensity Drug High-Intensity Dose High Atorvastatin 40-80mg Rosuvastatin 20-40mg Moderate doses: Atorvastatin 10-20mg, Rosuvastatin 5-10mg. - ADRs: 📌 Statins: Hepatotoxicity, Myopathy, Glucose ↑ (New Diabetes).
- Myopathy, rhabdomyolysis (monitor CK).
- Hepatotoxicity (monitor LFTs).
- New-onset diabetes mellitus.
- Contraindications (CIs):
- Pregnancy (teratogenic).
- Active liver disease.
- Interactions:
- CYP3A4 inhibitors (e.g., macrolides, azoles) ↑ toxicity of simvastatin, lovastatin, atorvastatin.
- Pravastatin, Rosuvastatin: Less CYP3A4 interaction.
⭐ Statins are best given in the evening/night as cholesterol synthesis is maximal then (except long-acting Atorvastatin/Rosuvastatin, which can be taken anytime).
Fibrates & Niacin - TG & HDL Tune-Up
Fibrates (e.g., Fenofibrate, Gemfibrozil)
- MoA: PPAR-α agonists → ↑LPL activity → ↓VLDL, ↑HDL.
- Use: Severe hypertriglyceridemia (TG >500 mg/dL) to prevent pancreatitis.
- ADRs: Myopathy (risk ↑ with statins), cholelithiasis (gallstones), GI upset.
⭐ Gemfibrozil + statin = higher myopathy risk vs. fenofibrate + statin.
Niacin (Vitamin B3)
- MoA: Inhibits lipolysis in adipose tissue → ↓hepatic VLDL synthesis.
- Effects: ↓LDL, ↓TG, ↑↑HDL (most potent HDL elevator).
- ADRs: Cutaneous flushing (PG-mediated; ↓ with aspirin/NSAID), pruritus, hyperuricemia (gout), hyperglycemia, hepatotoxicity.
- 📌 Niacin ADRs: Nice And Hot (Flushing), HyperGlycemia, HyperUricemia.
Other Key Players - Lipid Diversifiers
- Ezetimibe
- MoA: Inhibits dietary & biliary cholesterol absorption (NPC1L1 protein).
- Use: Monotherapy or adjunct to statins.
- ADRs: Generally well-tolerated; diarrhea, rare myopathy/hepatitis.
- PCSK9 Inhibitors (Evolocumab, Alirocumab)
- MoA: Monoclonal antibodies, prevent LDL receptor degradation → ↑LDL clearance.
- Use: Familial hypercholesterolemia, statin-intolerant, very high-risk ASCVD.
- Route: Subcutaneous injection.
- ADRs: Injection site reactions, nasopharyngitis.
⭐ PCSK9 inhibitors can achieve >50-60% additional LDL-C reduction when added to maximally tolerated statin therapy.
- Bile Acid Sequestrants (Resins) (Cholestyramine, Colestipol, Colesevelam)
- MoA: Bind bile acids in intestine, prevent reabsorption → ↑hepatic conversion of cholesterol to bile acids, ↑LDL receptors.
- ADRs: GI distress (constipation, bloating), ↓absorption of fat-soluble vitamins & other drugs (take other drugs 1h before or 4h after). May ↑TGs.
- Colesevelam: Fewer GI effects & drug interactions, safe in pregnancy.
- Omega-3 Fatty Acids (Fish Oil) (EPA, DHA)
- Use: Adjunct for severe hypertriglyceridemia (>500 mg/dL).
- MoA: ↓TG synthesis, ↑TG clearance.
- ADRs: GI upset, fishy aftertaste, bleeding risk (high doses).

High‑Yield Points - ⚡ Biggest Takeaways
- Statins (HMG-CoA reductase inhibitors) are first-line for ↑LDL; major side effect: myopathy.
- Fibrates primarily ↓ triglycerides by activating PPAR-α; risk of gallstones & myopathy with statins.
- Ezetimibe inhibits cholesterol absorption (NPC1L1); used with statins to further ↓LDL.
- Bile acid sequestrants (e.g., cholestyramine) cause GI distress and can ↑ triglycerides.
- Niacin causes cutaneous flushing (prostaglandin-mediated); effectively ↑HDL.
- PCSK9 inhibitors (evolocumab) are potent LDL reducers; injectable administration.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

