MOA & Basics - Inflammation Busters
- Synthetic analogs of endogenous cortisol; potent anti-inflammatory & immunosuppressive.
- Primary MOA (Genomic):
- Bind cytosolic Glucocorticoid Receptors (GR).
- GC-GR complex translocates to nucleus.
- Modulates gene expression:
- ↑ Synthesis of anti-inflammatory proteins (e.g., Lipocortin-1/Annexin A1, $I\kappa B\alpha$).
- ↓ Synthesis of pro-inflammatory proteins (cytokines, chemokines, $COX_2$, $PLA_2$).
- Net effect: ↓ Leukocyte migration, adhesion, phagocytosis; ↓ Mast cell degranulation.
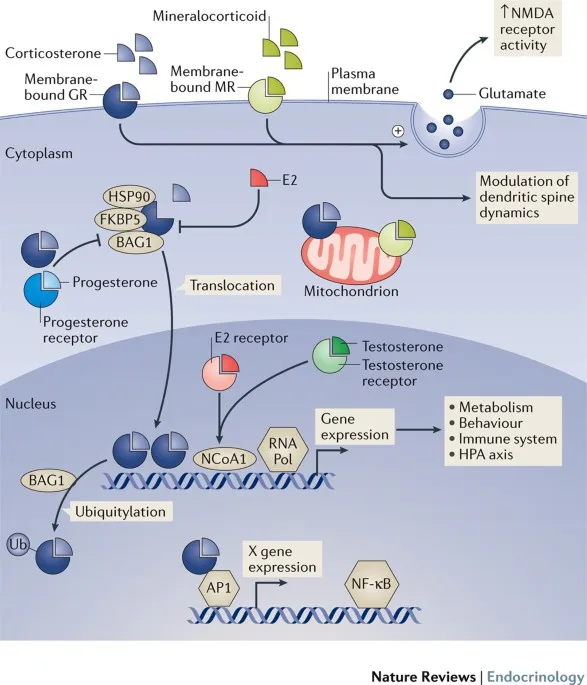
⭐ Glucocorticoids upregulate Annexin A1 (Lipocortin-1), which inhibits Phospholipase A2, thereby blocking arachidonic acid release and subsequent eicosanoid synthesis.
Classification & PK - Steroid Spectrum
- Duration of Action (DOA):
- Short (8-12h): Hydrocortisone, Cortisone
- Intermediate (12-36h): Prednisolone, Triamcinolone, Methylprednisolone
- Long (36-72h): Dexamethasone, Betamethasone
- Potency (AI / MC):
- Hydrocortisone: AI 1, MC 1 (Ref)
- Prednisolone: AI 4, MC 0.8
- Triamcinolone: AI 5, MC 0
- Dexamethasone: AI 25-30, MC 0
- Betamethasone: AI 25-30, MC 0
- Pharmacokinetics (PK):
- Absorption: Oral, IV, IM, topical.
- Metabolism: Hepatic. Prodrugs: Cortisone→Hydrocortisone, Prednisone→Prednisolone.
- Excretion: Renal. High protein binding. Cross placenta.
⭐ Dexamethasone & Betamethasone: potent AI, negligible MC effect; preferred in cerebral edema.
Anti-inflammatory Uses - Clinical Toolkit
- Rheumatic Disorders: Rheumatoid arthritis, SLE, vasculitis, polymyalgia rheumatica, acute gout.
- Allergic States: Severe asthma, anaphylaxis, angioedema, drug hypersensitivity reactions.
- Respiratory Diseases: COPD exacerbations, sarcoidosis, aspiration pneumonitis.
- Gastrointestinal: Inflammatory bowel disease (Crohn's, UC).
- Renal Disorders: Nephrotic syndrome (esp. minimal change disease).
- Dermatological: Pemphigus vulgaris, severe contact dermatitis, exfoliative dermatitis.
- Ophthalmic: Uveitis, optic neuritis, allergic conjunctivitis.
- Neurological: Cerebral edema (vasogenic), multiple sclerosis acute flares.
- Organ Transplantation: Immunosuppression to prevent graft rejection.
- Hematological: Autoimmune hemolytic anemia (AIHA), idiopathic thrombocytopenic purpura (ITP).
⭐ In bronchial asthma, inhaled corticosteroids (ICS) are cornerstone long-term controllers; systemic steroids for acute severe exacerbations.
Adverse Effects - Steroid Perils
Many effects are dose & duration-dependent:
- Metabolic: Hyperglycemia, weight gain (central obesity), Cushingoid features (moon facies, buffalo hump), osteoporosis, dyslipidemia.
- CNS: Mood swings (euphoria, psychosis), insomnia.
- GI: Peptic ulcer, GI bleeding.
- CV: Hypertension, fluid retention, hypokalemia.
- Immune: Immunosuppression (↑ infections, latent TB reactivation), impaired wound healing.
- MSK: Myopathy (proximal), aseptic necrosis (femoral head).
- Ocular: Posterior subcapsular cataracts, glaucoma.
- Skin: Thinning, striae, acne, hirsutism.
- Endocrine: HPA axis suppression (tapering vital!), growth retardation (children).
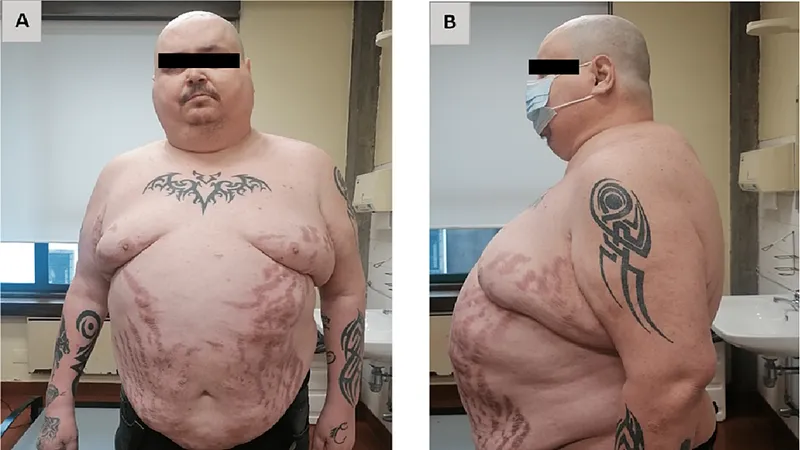
⭐ Aseptic necrosis of the femoral head is a serious, often irreversible, complication of chronic steroid therapy.
Clinical Guidelines - Smart Steroids
- Routes: Oral, IV, IM, topical, intra-articular.
- Dosing: Lowest effective dose, shortest duration. Alternate-day therapy (ADT) for long-term use (↓ side effects).
- Interactions: Enzyme inducers (e.g., rifampicin) ↓ efficacy. NSAIDs ↑ GI bleed risk.
- Withdrawal: Taper gradually if used > 2-3 weeks to prevent adrenal insufficiency.
⭐ HPA axis suppression necessitates gradual tapering after prolonged use to prevent adrenal crisis.
High‑Yield Points - ⚡ Biggest Takeaways
Error: Failed to generate content for this concept group.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

