Radiation Basics - Tiny Rays, Big Concerns
- Ionizing Radiation: High energy; removes electrons from atoms, causing ionization.
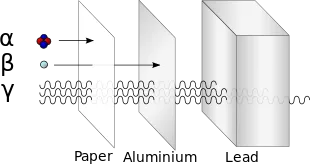
- Types: Alpha ($\alpha$), Beta ($\beta$), Gamma ($\gamma$), X-rays, Neutrons.
- Sources:
- Natural: Radon (major contributor), cosmic rays, terrestrial (soil/rocks).
- Man-made: Medical (X-rays, CT scans, radiotherapy), industrial, nuclear fallout.
- Key Units:
- Absorbed Dose: Gray (Gy). Energy deposited/mass. (1 Gy = 100 rad).
- Equivalent Dose: Sievert (Sv). $H = D \times W_R$ (Radiation Weighting Factor). (1 Sv = 100 rem).
- Effective Dose: Sievert (Sv). $E = \sum_T (W_T \times H_T)$ (Tissue Weighting Factor).
⭐ Radon gas is the largest natural source of radiation exposure for the general public, contributing significantly to background radiation levels globally.
Biological Effects - Growing Bodies, Greater Risks
- Children: ↑ vulnerability due to rapid cell division, longer lifespan for effects to manifest.
- Effects:
- Deterministic: Dose-dependent, threshold exists (e.g., skin burns, cataracts). Severity ↑ with dose.
- Stochastic: Probability-dependent, no threshold (e.g., cancer, genetic effects). Probability ↑ with dose.
- Highly Radiosensitive Tissues: Bone marrow, thyroid, gonads, lens, developing brain, breast.
- Influencing Factors: Age (younger ↑risk), dose, dose rate, radiation type.
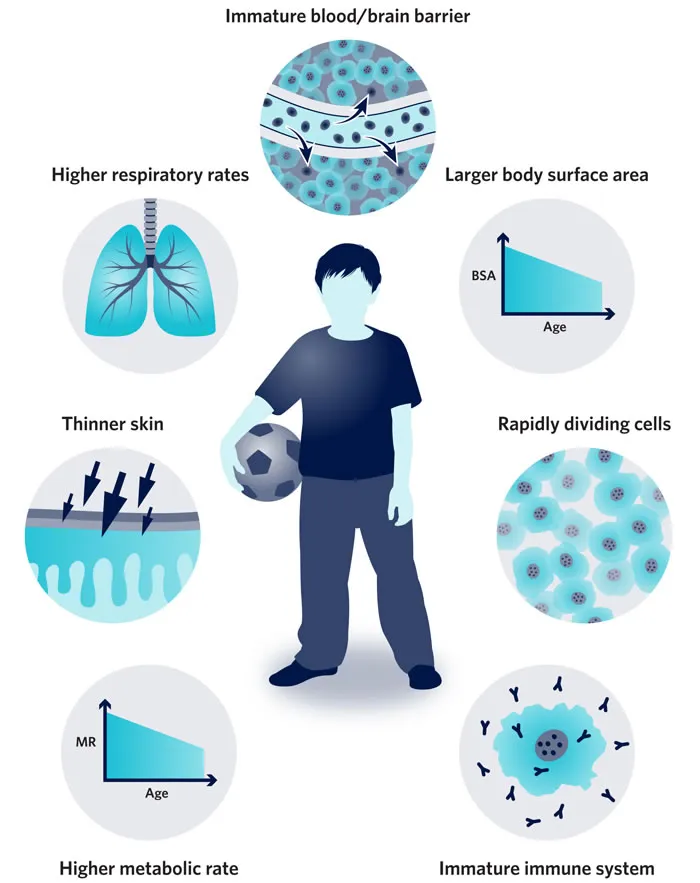
⭐ Children have a 2-3 times higher lifetime risk of developing radiation-induced solid cancers compared to adults exposed to the same dose.
Clinical Features - Sickness Spectrum
- Acute Radiation Syndrome (ARS): Dose-dependent, progresses through distinct phases.
- ARS Syndromes (Manifest Illness Phase):
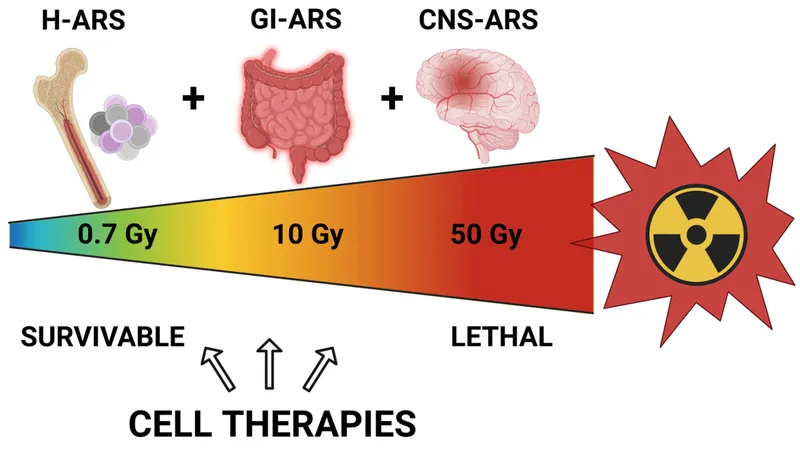
- Hematopoietic (Bone Marrow) Syndrome: 1-6 Gy. Lymphopenia (early indicator), pancytopenia. ↑Infection, hemorrhage.
- Gastrointestinal (GI) Syndrome: 6-10 Gy. Severe N/V/D, mucosal denudation, dehydration, sepsis. Often fatal.
- Neurovascular/CNS Syndrome: >10 Gy (often >20 Gy). Rapid onset: ataxia, seizures, coma. Uniformly fatal.
- Chronic Effects:
- Carcinogenesis (leukemia, thyroid, solid tumors), genetic mutations, cataracts, pediatric growth retardation.
⭐ Lymphocyte count drop within 24-48 hours is a key early biological dosimeter for exposure severity.
Diagnosis & Management - Action Plan Alpha
- Triage & Decontaminate: Secure scene, ABCs. Remove clothes, wash skin. Consider internal decorporation.
- Estimate Dose (Biodosimetry): Lymphocyte kinetics (nadir at ~48h), dicentric chromosomes.
- Supportive Care: Fluids, antiemetics, infection prophylaxis if ANC < 500/µL.
- Management Flowchart:
- Specific Agents: KI (thyroid block), Prussian Blue (Cs, Tl), DTPA (transuranics), G-CSF (neutropenia).
- Follow-up: Monitor for ARS, late effects.
⭐ Absolute lymphocyte count at 48h is a key prognosticator for Acute Radiation Syndrome (ARS).
Prevention & Protection - Kid-Safe Shielding
- 📌 ALARA Principle: As Low As Reasonably Achievable.
- Core Principles:
- ↓ Time: Minimize exposure duration.
- ↑ Distance: Maximize distance from source.
- Shielding: Use lead aprons, thyroid/gonadal shields.
- Pediatric Focus:
- Always use child-sized shielding.
- Effective immobilization to prevent repeat exposures.
- Justify all radiologic procedures.
- Prefer USG/MRI when possible.
- Nuclear Emergencies:
- Potassium Iodide (KI) for thyroid gland protection.

- Potassium Iodide (KI) for thyroid gland protection.
⭐ Children have ↑ radiosensitivity (cells rapidly divide) & longer life expectancy for stochastic effects to manifest; 2-10x more sensitive than adults.
High-Yield Points - ⚡ Biggest Takeaways
- Children exhibit ↑ radiosensitivity; ALARA principle (As Low As Reasonably Achievable) is crucial in pediatric imaging.
- Deterministic effects (e.g., skin erythema, epilation) are dose-dependent with a threshold.
- Stochastic effects (e.g., malignancy, genetic changes) are probabilistic, with no threshold.
- Thyroid cancer is a significant concern post-exposure; Potassium Iodide (KI) for thyroid blocking.
- Acute Radiation Syndrome (ARS) phases: prodromal, latent, manifest illness, and recovery/death.
- Fetal radiation: highest risk during organogenesis (2-15 weeks gestation); doses < 50 mGy generally not linked to deterministic effects in utero.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

