RMS Primer - Tiny Tumors
- Definition: A malignant mesenchymal tumor characterized by rhabdomyoblastic differentiation (cells resembling striated muscle).
- Epidemiology: The most common soft tissue sarcoma in children.
- Peak Incidence: Bimodal distribution, with peaks at 2-6 years and 14-18 years.
- Associated Syndromes: Li-Fraumeni syndrome, NF1, Beckwith-Wiedemann syndrome, Costello syndrome.
⭐ Rhabdomyosarcoma is the most common soft tissue sarcoma in children.
RMS Patho & Types - Cellular Culprits
- Origin: Primitive mesenchymal cells (skeletal muscle lineage).
- Histological Subtypes:
- Embryonal (ERMS): ~60-70%, better prognosis. Variants: Botryoid (best prognosis), Spindle cell (includes Sclerosing RMS).
- Alveolar (ARMS): ~20-30%, worse prognosis. Translocations: t(2;13) PAX3-FOXO1 (commoner, poorer), t(1;13) PAX7-FOXO1.
- Pleomorphic: Rare in children.
⭐ Alveolar RMS: PAX-FOXO1 fusions; t(2;13) PAX3-FOXO1 (common, aggressive).
oka
RMS Sites & Signs - Location Clues
Presentation: Often painless mass; varies by site.
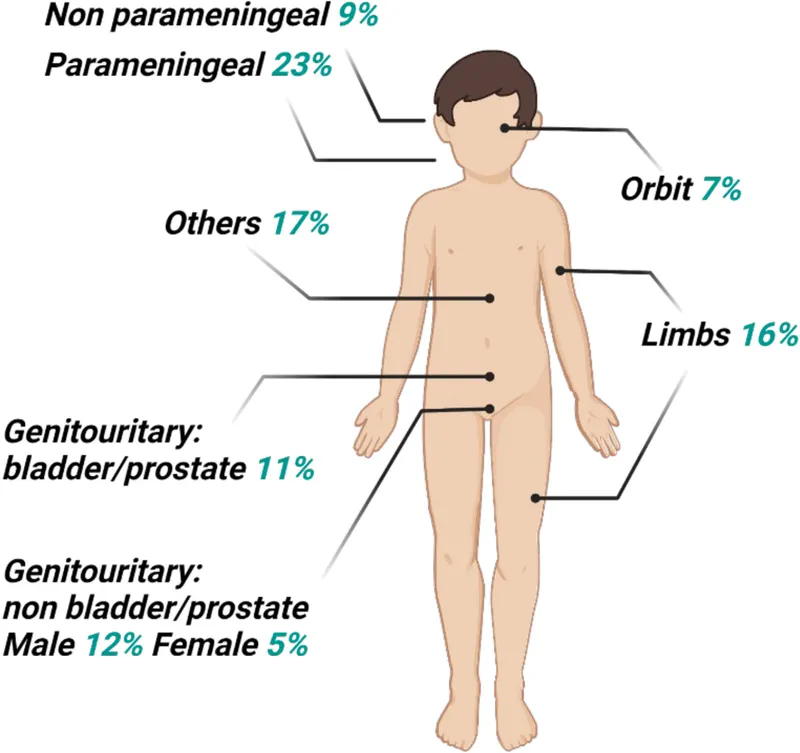
Favorable Sites:
- Orbit: Proptosis, diplopia.
- Non-parameningeal Head & Neck (H&N): Painless mass.
- GU (non-Bladder/Prostate): Paratesticular, vaginal, uterine masses.
Unfavorable Sites:
- Parameningeal H&N (nasopharynx, middle ear, paranasal sinuses): Cranial nerve palsies, proptosis; CSF spread risk.
- Bladder/Prostate: Hematuria, obstruction.
- Extremities/Trunk: Swelling, pain.
⭐ Sarcoma botryoides (embryonal RMS variant): grape-like mass in vagina/bladder.
 oka
oka
RMS Diagnosis & Staging - Pinpointing the Foe
- Biopsy: Essential (incisional/excisional/core). Histopathology + IHC.
- IHC Markers: Desmin, Myogenin (Myf4), MyoD1 (Myf3) - highly specific.
- Imaging:
- Primary: MRI (preferred), CT.
- Metastasis: CT Chest, PET-CT, Bone scan.
- Staging Workup: Bone marrow aspiration & biopsy. CSF cytology (parameningeal).
- Staging Systems: IRS Clinical Group (I-IV), TNM Pre-treatment.
⭐ Myogenin and MyoD1 are nuclear transcription factors crucial for myogenic differentiation and are highly specific immunohistochemical markers for RMS.
RMS Treatment - Multimodal Attack
- Standard: Aggressive multimodal therapy (Chemotherapy, Surgery, Radiotherapy).
- Risk-adapted strategy guides intensity: Low, Intermediate, High-risk groups.
- Chemotherapy:
- Core: VAC (Vincristine, Actinomycin D, Cyclophosphamide) or IVA.
- High-risk: Dose intensification.
- Surgery: Wide local excision aiming for negative margins. Organ preservation is key.
- Radiotherapy (RT): Crucial for local control, especially if unresectable or positive margins. Proton therapy considered.
⭐ VAC (Vincristine, Actinomycin D, Cyclophosphamide) is the cornerstone chemotherapy regimen.
RMS Prognosis & Genetics - Future Outlook
- Overall survival: ~70-80%; varies by risk group.
- Key Prognostic Factors:
- Histology: Embryonal (favorable) vs. Alveolar (unfavorable).
- Site: Favorable (e.g., orbit) vs. Unfavorable.
- Stage & IRS Group (resectability, extent).
- Age: <1 yr or >10 yrs may have worse outcomes.
- Response to initial therapy.
- Genetics:
⭐ PAX3-FOXO1 fusion (esp. in Alveolar RMS) = poor prognosis.
- Long-term sequelae: Growth impairment, endocrine dysfunction, secondary malignancies (↑ risk).
High‑Yield Points - ⚡ Biggest Takeaways
- Most common pediatric soft tissue sarcoma; bimodal age peak (2-6 yrs, teens).
- Key sites: Head & Neck (orbit, parameningeal), Genitourinary (sarcoma botryoides), Extremities.
- Embryonal (common, better prognosis) vs. Alveolar (aggressive, PAX-FOXO1 fusion).
- Histologically a "small round blue cell tumor".
- Multimodal therapy (surgery, chemotherapy, radiotherapy) is standard.
- Parameningeal sites: high CNS extension risk, mandating CNS evaluation.
- Prognosis: Alveolar histology worse; depends on site, stage, resectability.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

