Leukemia Basics - Tiny Troublemakers
- Uncontrolled proliferation of abnormal white blood cells (WBCs) in bone marrow.
- "Liquid tumors" that crowd out normal blood cell production (anemia, infections, bleeding).
- Most common childhood cancer.
- Major Types:
- Acute Lymphoblastic Leukemia (ALL): Most frequent (~75-80%). Peak: 2-5 yrs.
- Acute Myeloid Leukemia (AML): Accounts for ~15-20%.

⭐ Down syndrome confers a 10-20 fold ↑ risk for developing acute leukemia (both ALL & AML).
ALL Unmasked - Lympho‑Blast Off!
- Most common childhood cancer; peak 2-5 yrs.
- Presentation: Fever, pallor, bleeding, bone pain. Lymphadenopathy, hepatosplenomegaly. CNS/testicular involvement possible.
- Diagnosis:
- Bone Marrow: >25% lymphoblasts (WHO).
- Immunophenotyping:
- B-ALL (~85%): CD19, CD10 (CALLA), TdT+.
- T-ALL (~15%): CD3, CD7, TdT+. Often mediastinal mass.
- Cytogenetics (Prognostic):
- Good: Hyperdiploidy, t(12;21) [ETV6-RUNX1].
- Poor: Hypodiploidy, t(9;22) [BCR-ABL1], MLL rearrangements (11q23).
- Crucial: CNS prophylaxis (intrathecal MTX) for all.
⭐ T-ALL often presents with a large anterior mediastinal mass causing respiratory distress or SVC syndrome.
ALL Combat Plan - Victory Blueprint
- Treatment Phases (Multi-agent Chemo):
- Induction (VCR, Prednisolone, L-Asparaginase ± Daunorubicin): Achieve remission.
- Consolidation: Eradicate residual cells.
- Interim Maintenance.
- Delayed Intensification.
- Maintenance (6-MP, MTX): Total 2-3 yrs.
- CNS Prophylaxis: Mandatory; Intrathecal (IT) Methotrexate.
- NCI Risk Stratification (B-ALL):
- Standard Risk (SR): Age 1-9.99 yrs & WBC < 50,000/µL.
- High Risk (HR): Age <1 yr / ≥10 yrs or WBC ≥ 50,000/µL.
- Key Prognostic Factors:
- Good: Age 1-9 yrs, WBC <50K, t(12;21) ETV6-RUNX1, hyperdiploidy.
- Poor: Age <1 yr, Ph+ t(9;22) BCR-ABL1, MLL rearranged, hypodiploidy, CNS disease.
⭐ Minimal Residual Disease (MRD) status post-induction is the most powerful prognostic indicator in ALL.
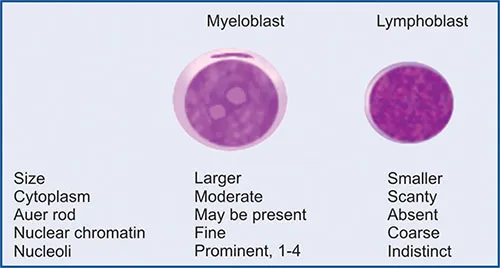
AML Alert - Myeloid Mayhem
- Predominantly adults, but occurs in children; poorer prognosis than ALL.
- Diagnosis: >20% myeloblasts in bone marrow.
- Markers: Myeloperoxidase (MPO), Sudan Black B.
- 📌 Auer rods: Pathognomonic, especially in APL (M3).
- Clinical: Gingival hypertrophy, leukemia cutis, DIC (esp. APL).
- Key Cytogenetics:
- APL (M3): t(15;17) (PML-RARA); treat with ATRA.
- Good prognosis: t(8;21), inv(16).
- Poor prognosis: Monosomy 5 or 7.
⭐ APL (Acute Promyelocytic Leukemia), a subtype of AML, is uniquely responsive to All-Trans Retinoic Acid (ATRA) therapy, which induces differentiation of leukemic promyelocytes.
Leukemia Crisis Mode - Code Red!
- Tumor Lysis Syndrome (TLS): Oncologic emergency from rapid cell death. Key labs: ↑K, ↑PO4, ↑Uric Acid, ↓Ca.
- Management: Aggressive IV fluids, Allopurinol or Rasburicase.
- Monitor: Strict I/O, electrolytes. Cairo-Bishop criteria for diagnosis.
- Hyperleukocytosis: Extreme WBC count >100,000/µL. High risk of leukostasis (CNS, respiratory distress).
- Management: Urgent cytoreduction (Hydroxyurea, Leukapheresis), hydration.
- Febrile Neutropenia: Fever (T >38.3°C single, or >38°C for 1hr) + ANC <500/µL. Life-threatening!
- Management: Immediate empiric broad-spectrum IV antibiotics.
⭐ Rasburicase is contraindicated in G6PD deficiency due to risk of hemolysis and methemoglobinemia.
High‑Yield Points - ⚡ Biggest Takeaways
- ALL is the most common childhood malignancy; peak incidence 2-5 years.
- Good prognostic factors in ALL: Age 1-9 years, WBC < 50,000/μL, t(12;21).
- Poor prognostic factors in ALL: Age <1yr/>10yrs, WBC >50,000/μL, t(9;22) (Philadelphia), MLL gene.
- CNS prophylaxis (intrathecal chemotherapy) is crucial in ALL.
- AML: Auer rods are pathognomonic. APL (M3) with t(15;17), treat with ATRA; risk of DIC.
- Down syndrome confers ↑ risk of ALL and AML (especially megakaryoblastic).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

