NTD Basics - Tube Troubles
- Definition: Neural Tube Defects (NTDs) are congenital anomalies of the developing brain and spinal cord.
- Embryology: Arise from failure of the neural tube to close completely during the 3rd-4th week of gestation (days 21-28).
- Two Main Categories:
- Open NTDs: Neural tissue is exposed externally. E.g., anencephaly, myelomeningocele.
- Closed NTDs: Neural defect is covered by skin. E.g., spina bifida occulta, meningocele.
- Primary Prevention: Periconceptional folic acid supplementation is crucial for reducing NTD risk.
⭐ Neural tube closure occurs by the 28th day post-conception (end of 4th week), often before pregnancy is confirmed.
oka
Causes & Prevention - Defect Defense
- Causes:
- Folate/B12 deficiency; Maternal diabetes, obesity.
- Drugs: Valproate, Carbamazepine.
- Genetics: Family Hx, Trisomies.
- Maternal hyperthermia.
- Prevention:
- Folic Acid:
- Low risk: 0.4 mg/day (preconception to 1st trimester).
- High risk (prior NTD, AEDs): 4 mg/day (3 months prior to 1st trimester). 📌 Four Always for High Risk!
- Control diabetes; Avoid teratogens.
- Folic Acid:
⭐ Maternal valproate use is a significant risk factor for NTDs.
Cranial NTDs - Head Cases
- Cranial neural tube defects involve failure of anterior neuropore closure (day 25).
| Feature | Anencephaly | Encephalocele |
|---|---|---|
| Defect | Absence of brain, skull, scalp | Herniation of cranial contents through skull defect |
| Presentation | 'Frog-eye'/'Mickey Mouse' on USG; polyhydramnios | Sac-like protrusion, often occipital |
| Contents | Rudimentary brain tissue, no bony covering | Meninges, CSF, +/- brain tissue |
| Prognosis | Incompatible with life | Variable; depends on brain tissue in sac |
⭐ Anencephaly: Most common NTD globally. Associated with maternal diabetes, folate deficiency. 'Frog-eye' or 'Mickey Mouse' appearance on USG is characteristic due to absent cranial vault and exposed neural tissue. Incompatible with life.
- 📌 ACE Mnemonic for Encephalocele sites: Anterior (frontal, nasofrontal), Cranial vault (parietal, occipital), External (basal, transsphenoidal). Occipital is most common overall (75%).
Spinal NTDs - Spine Signs
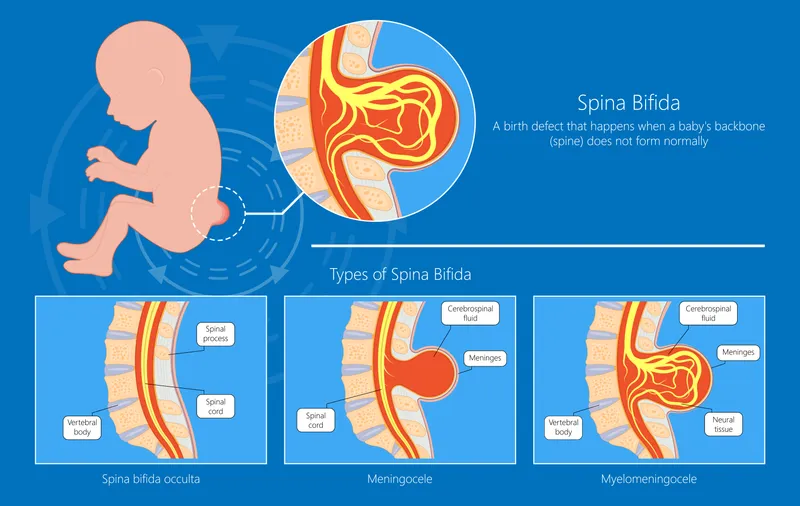
| Feature | Spina Bifida Occulta | Meningocele | Myelomeningocele (MMC) |
|---|---|---|---|
| Defect | Vertebral arch defect | Defect with sac protrusion | Defect with sac protrusion |
| Sac Content | None | Meninges, CSF | Meninges, CSF, Cord, Nerves |
| Spinal Cord | Normal position | Usually normal position | Displaced into sac, dysplastic |
| Skin Cover | Intact; may have tuft of hair, dimple | Intact skin | Thin membrane or open (Rachischisis) |
| Neuro Deficit | Usually none; tethered cord possible | Rare; depends on associated lesions | Common; motor, sensory, bladder/bowel |
📌 SAM: Skin (Occulta), Arachnoid/CSF (Meningocele), Medulla/Cord (Myelomeningocele) in sac (simplified).
Diagnosis & Management - Scan & Plan
Diagnosis:
- Antenatal:
- ↑MSAFP (>2.0-2.5 MoM).
- USG: 1st/2nd trimester, lemon/banana signs (spina bifida), anencephaly.
- Amniotic AFP & AChE (confirmatory).
- Postnatal:
- Clinical exam: Visible lesion, neuro deficits.
- Imaging: X-ray, USG, MRI.
Management:
- Antenatal: Counseling, planned delivery, ?in-utero repair.
- Postnatal:
- Immediate: Sterile dressing, prone.
- Surgical repair: 24-72 hrs (open NTDs).
- Long-term: Multidisciplinary team (VP shunt for hydrocephalus, urology, ortho, physio).
⭐ 'Lemon sign' (frontal bone scalloping) and 'banana sign' (cerebellar distortion) are classic USG markers for spina bifida, often associated with Chiari II malformation.
High‑Yield Points - ⚡ Biggest Takeaways
- Folic acid (0.4mg daily; 4mg for high-risk) is crucial for NTD prevention.
- ↑ Maternal serum AFP & amniotic fluid AFP are key diagnostic markers (except in spina bifida occulta).
- ↑ Amniotic fluid acetylcholinesterase is a highly specific marker for open NTDs.
- Myelomeningocele, the most common severe NTD, is strongly linked to Chiari II malformation & hydrocephalus.
- Anencephaly presents with "frog-eye" appearance, polyhydramnios, and is incompatible with life.
- Major risk factors include maternal valproate or carbamazepine use, pre-gestational diabetes, and ↓folate levels.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

