UTI Basics - Tiny Patients, Big Bugs
- Urinary Tract Infection (UTI): Microbial invasion of urinary tract structures.
- Significant bacteriuria criteria:
- Suprapubic aspirate (SPA): Any gram-negative bacilli or >1,000 CFU/mL gram-positive cocci.
- Catheter specimen: ≥104 CFU/mL (often ≥5x104 CFU/mL).
- Clean-catch midstream urine (toilet-trained child): ≥105 CFU/mL of a single uropathogen.
- Common Risk Factors:
- Age <1 year (esp. uncircumcised males <3 months, then ↑ female incidence).
- Vesicoureteral reflux (VUR).
- Posterior urethral valves (PUV).
- Neurogenic bladder, dysfunctional voiding.
- Constipation.
- Etiology:
⭐ E. coli is the most common uropathogen, accounting for ~80-90% of pediatric UTIs.
- Others: Klebsiella, Proteus, Enterococcus, S. saprophyticus (adolescent females).
Symptom Spotting - Age Matters
- Neonates (<1 month):
- Non-specific: fever, hypothermia, poor feeding, vomiting
- Lethargy, jaundice, irritability, poor weight gain
- Sepsis-like picture, abdominal distension
- Infants (1 month - 2 years):
- Fever (often sole symptom), irritability, crying on micturition
- Poor feeding, vomiting, diarrhea, abdominal pain/distension
- Strong/foul-smelling urine
⭐ Unexplained fever is the most common presentation of UTI in infants and young children (<2 years).
- Preschoolers (2-5 years):
- Classic lower UTI: dysuria, urgency, frequency, hesitancy
- New-onset incontinence (enuresis), suprapubic pain
- Foul-smelling urine, hematuria, fever, vomiting
- School-aged Children & Adolescents (>5 years):
- Cystitis: dysuria, urgency, frequency, suprapubic pain, incontinence
- Pyelonephritis: flank/loin pain, CVA tenderness, high fever, chills, malaise
Diagnosis Deep Dive - Labs & Scans
- Urinalysis (UA): Rapid screen.
- Positive: Pyuria (>5 WBCs/hpf or +Leukocyte Esterase), Nitrites (+ for Gram-neg, e.g., E.coli).
- Microscopy: Bacteriuria, WBC casts (suggest pyelonephritis).
- Urine Culture (Gold Standard): Essential for diagnosis & sensitivity.
- Clean catch (mid-stream): ≥10^5 CFU/mL (single organism).
- Catheter specimen: ≥5 x 10^4 CFU/mL.
- Suprapubic Aspiration (SPA): Any Gram-neg growth; ≥10^3 CFU/mL Gram-pos. (Most sterile sample).
- Blood Tests (if ill, <3 months, or suspected pyelonephritis): CBC (leukocytosis), CRP/ESR (↑inflammation), Blood Culture, Renal Function Tests (RFTs).
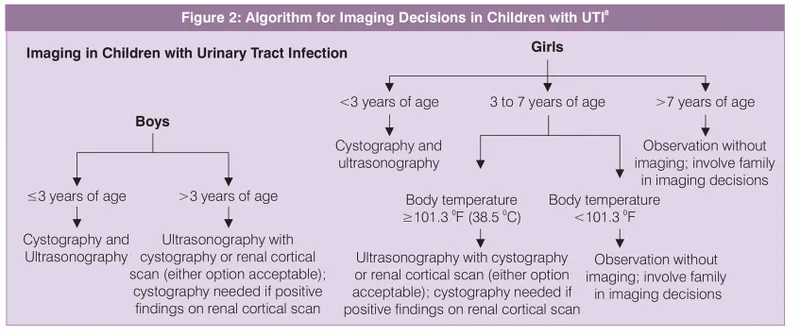
- Imaging Protocol:
> ⭐ For a child <**2** years with a first febrile UTI, a renal and bladder **ultrasound (RBUS)** should be performed.
- RBUS: Initial scan. Detects renal size, hydronephrosis, abscess, gross anomalies.
- VCUG (MCU): Gold standard for Vesicoureteral Reflux (VUR) diagnosis and grading.
- DMSA Scan: Most sensitive for acute pyelonephritis & permanent renal cortical scarring; perform 4-6 months post-UTI to assess permanent damage.
Treatment & Guard - UTI Combat
- Goals: Eradicate infection, prevent renal damage & recurrence.
- Management:
- Cystitis (Afebrile): Oral Abx (Co-trimoxazole, Nitrofurantoin) for 3-7 days.
- Pyelonephritis (Febrile):
- Oral intake OK: Oral Abx (Cefixime) for 7-14 days.
- Toxic/<3mo/Vomiting: IV Abx (Ceftriaxone), then oral. Total 7-14 days.
- Prophylaxis: For recurrent UTI/VUR Gr III-V (Nitrofurantoin/Co-trimoxazole).
- Supportive: Hydration, timed voiding. Imaging (USG, MCU/DMSA) as indicated.
⭐ Oral antibiotics are as effective as parenteral antibiotics for febrile UTIs in children who are non-toxic and can tolerate oral intake; typical duration for pyelonephritis is 7-14 days.
High‑Yield Points - ⚡ Biggest Takeaways
- E. coli is the most common pathogen in pediatric UTIs.
- Urine culture is gold standard for diagnosis; suprapubic aspirate is preferred in infants.
- Febrile UTI in infants (<2 years) requires renal ultrasound; consider MCU/VCUG for VUR.
- Vesicoureteral reflux (VUR) is a key risk factor for recurrent UTIs and renal scarring.
- Prompt antibiotics are vital to prevent long-term renal damage.
- DMSA scan best detects renal scars and acute pyelonephritis_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

