GN Basics - Filter Failure Fiesta
- Glomerulonephritis (GN): Inflammation of glomeruli, kidney's primary filtration units.
- Core Pathology: "Filter Failure Fiesta" - breakdown of glomerular filtration barrier.
- Barrier components: Endothelium, Glomerular Basement Membrane (GBM), Podocytes (visceral epithelial cells).
- Damage → ↑permeability → leakage of RBCs & proteins.
- Key Manifestations:
- Hematuria (RBCs in urine): Often "cola-colored" or smoky urine.
- Proteinuria (protein, esp. albumin, in urine): Leads to frothy urine, edema.
- Classification (Simplified):
- Mechanism: Immune-mediated (most common), Pauci-immune, Anti-GBM disease, Non-immune.
- Origin: Primary (kidney-limited) vs. Secondary (systemic disease association).
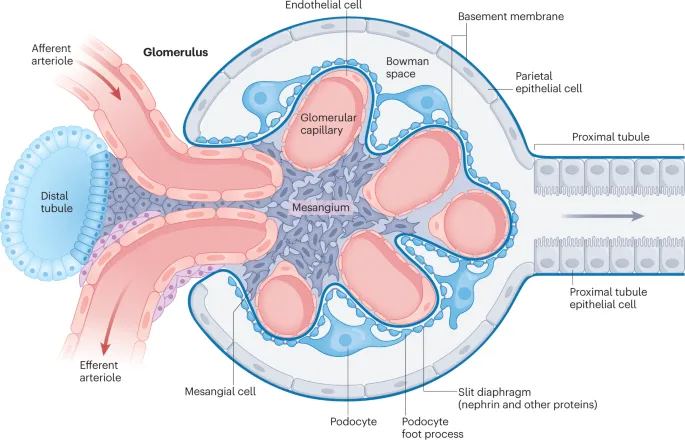
⭐ Glomerular damage in most GNs is primarily immune-mediated, involving antibodies, complement activation, and cellular immune responses.
Clinical Clues - Spotting the Swell
- Key presentation: Acute Nephritic Syndrome.
- Edema:
- Periorbital edema (classic, esp. morning), often pitting.
- Progresses to dependent edema (pedal, sacral), ascites, anasarca.
- Hematuria:
- Microscopic (RBCs, significant RBC casts in urine sediment).
- Macroscopic: Characteristic 'Coca-Cola' or 'smoky' colored urine.
- Hypertension: Acute onset; may be severe (e.g., hypertensive encephalopathy).
- Oliguria: ↓ urine output (typically < 1 mL/kg/hr in children).
- Proteinuria: Present, usually sub-nephrotic range.
- Systemic symptoms: Malaise, fever, flank or abdominal pain.
⭐ The classic triad of nephritic syndrome is hematuria, hypertension, and edema; 'Coca-Cola' or 'smoky' urine is a hallmark of gross hematuria.
Diagnostic Drill-Down - Unmasking the Culprit
- Urinalysis: Key initial test!
- Hematuria, Proteinuria
- RBC casts: Pathognomonic.
⭐ Presence of RBC casts in urine sediment is pathognomonic for glomerulonephritis, indicating glomerular bleeding.
- Blood Tests:
- KFT: ↑ Urea, ↑ Creatinine, ↓ eGFR.
- Serum electrolytes.
- Complements: ↓ C3 (PSGN, MPGN), ↓ C4 (Lupus Nephritis).
- Serology: ASLO (post-strep), ANA (lupus), ANCA (vasculitis).
- Imaging:
- USG KUB: Kidney size, echogenicity; rule out other causes.
- Renal Biopsy: Gold standard for diagnosis & therapy guidance.
- Indications: Atypical, RPGN, steroid-resistant nephrotic syndrome, unclear Dx.

Major GN Types - Rogues' Gallery
- Post-Streptococcal GN (PSGN)
- 📌 "Post-Strep GN: 1-3 wks post-pharyngitis, 3-6 wks post-impetigo; Low C3; ASO positive."
- Acute nephritic syndrome (edema, HTN, hematuria).
- Labs: ↓C3, ↑ASO/Anti-DNase B. Biopsy (if atypical): Subepithelial "humps".
- Prognosis: Excellent in children.
- IgA Nephropathy (Berger's Disease)
- Most common primary GN. Episodic gross hematuria (often synpharyngitic).
- Labs: Normal C3, Serum IgA often ↑. Biopsy: Mesangial IgA deposits.
- Prognosis: Variable; 20-30% progress to ESRD in 20 yrs.
- Henoch-Schönlein Purpura (HSP) Nephritis / IgA Vasculitis
- Systemic: palpable purpura, arthritis, abdominal pain, renal disease.
- Renal: Mesangial IgA (histologically similar to IgA nephropathy). Labs: Normal C3.
- Prognosis: Generally good; monitor renal function & BP.
- Rapidly Progressive GN (RPGN) / Crescentic GN
- Clinical emergency: Rapid ↓ GFR (days-weeks). Severe oliguria.
- Biopsy: Extensive crescent formation (>50% of glomeruli).
- Prognosis: Poor without urgent, aggressive immunosuppression.
⭐ Post-streptococcal glomerulonephritis (PSGN) is the most common cause of acute nephritic syndrome in children worldwide and typically has an excellent prognosis with supportive care.
High‑Yield Points - ⚡ Biggest Takeaways
- PSGN: Cola-colored urine, edema, HTN 1-2 weeks post-strep; low C3, ↑ASO.
- IgA Nephropathy (Berger's): Most common primary GN; recurrent gross hematuria with URTI. Normal C3.
- HSP Nephritis: Systemic vasculitis; palpable purpura, arthritis, abdominal pain, renal (IgA) involvement.
- RPGN: Crescents on biopsy, rapid renal function decline; requires urgent management.
- Alport Syndrome: X-linked; hematuria, sensorineural deafness, ocular defects (e.g., lenticonus).
- RBC casts in urine indicate glomerular bleeding; biopsy for definitive diagnosis_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

