Intro & Epidemiology - Tiny Targets, Big Threat
- Mycobacterium tuberculosis infection in individuals < 15 years.
- India: Highest global pediatric TB burden (approx. 27% of world's cases); a major public health concern.
- Transmission: Primarily airborne droplets from an adult with active pulmonary TB.
- Risk factors: Malnutrition, HIV, household contact, age < 5 yrs.
- Young children (< 5 yrs) are more prone to rapid progression and severe forms like TBM or miliary TB.
⭐ Globally, an estimated 1.2 million children develop TB annually, with India contributing significantly to this burden (around 25-30%).
Pathogenesis & Clinical Forms - TB's Tiny Takeover
- Infection Pathway: Inhalation of MTB → Alveolar macrophages → Regional lymph nodes (hilar/mediastinal).
- Ghon Focus: Initial lung lesion.
- Ghon Complex: Ghon focus + lymphadenopathy.
- Ranke Complex: Calcified (healed) Ghon complex.
- Immune Response: Cell-mediated immunity (CMI) critical; develops in 2-10 weeks. Granuloma formation contains bacilli.
- Progression Risk: ↑ in <5 yrs, malnutrition, HIV → active disease.
- Clinical Forms in Children:
- Pulmonary TB (PTB): Primary complex common; cavitation rare. Miliary TB (hematogenous).
- Extrapulmonary TB (EPTB) - More common than in adults:
- Lymph Node TB: Most common EPTB (e.g., scrofula).
- TB Meningitis (TBM): High mortality. Staged 1-3 (MRC).
- Bone & Joint (Pott's spine), Abdominal, Disseminated.
⭐ Lymph node TB (especially cervical - scrofula) is the most common form of extrapulmonary TB in children.
- 📌 Primary complex, Extrapulmonary, Disseminated disease common in PEDiatric TB (vs. adult apical cavitation).
Diagnosis in Children - Cracking Kid Cases
- Challenges: Paucibacillary nature, non-specific symptoms, sputum collection difficulty.
- Key Pillars:
- History: TB contact (crucial!), persistent cough >2wks, unexplained fever >1wk, weight loss/failure to thrive.
- TST (Mantoux): Induration ≥10mm positive (irrespective of BCG); ≥5mm positive if HIV-infected, severely malnourished, immunosuppressed, or close contact with sputum-positive case. 📌 BCG Can Give Positive Test.
- IGRAs (Interferon-Gamma Release Assays): More specific than TST, especially in BCG-vaccinated. Not routinely recommended for <5 yrs by IAP (Indian Academy of Pediatrics), consider if TST ambiguous.
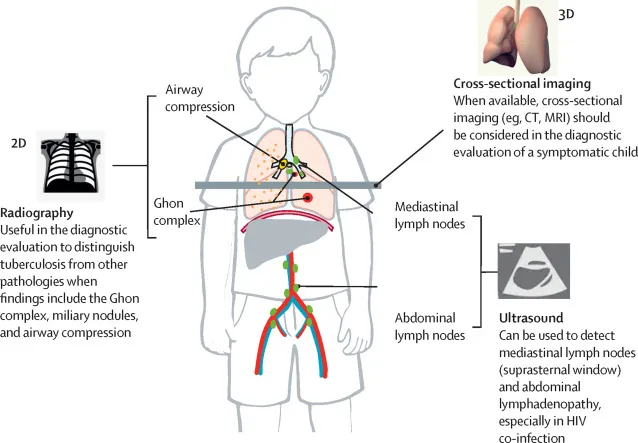
- Chest X-ray (CXR): Persistent hilar/paratracheal lymphadenopathy (commonest), miliary TB, consolidation, pleural effusion.

- Microbiological Confirmation (Aim for this!):
- Specimens: Gastric aspirate (GA) (≥2, ideally 3 consecutive morning samples), induced sputum, BAL, lymph node aspirate (FNA), pleural fluid, CSF, biopsy.
- CBNAAT (Xpert MTB/RIF or Ultra): WHO-recommended initial test for pulmonary & EPTB. Detects M.tb & Rifampicin resistance rapidly.
- AFB Smear: Low sensitivity in children (paucibacillary).
- Culture (Solid/Liquid): Gold standard, highest sensitivity; drug susceptibility testing (DST).
- Scoring Systems: IAP Pediatric TB Guidelines Score useful when microbiological proof is lacking.
- Extra-pulmonary TB (EPTB): Diagnosis often relies on imaging (USG, CT, MRI) & microbiological/histopathological exam of specimen from affected site.
⭐ CBNAAT (Xpert MTB/RIF or Ultra) is the WHO-recommended initial diagnostic test for both pulmonary and most forms of extra-pulmonary TB in children, significantly improving case detection.
Treatment & Prevention - Kicking TB Out
- Strategy: DOTS essential. Pediatric weight-band FDCs.
- Drug-Sensitive TB (DS-TB) - Children:
- IP: 2 months HRZE (Isoniazid, Rifampicin, Pyrazinamide, Ethambutol).
- CP: 4 months HRE.
- Drug-Resistant TB (DR-TB) - Children:
- Longer, complex regimens (e.g., shorter oral MDR-TB: 9-11 months).
- Follow current NTEP guidelines.
- Adjunctive: Corticosteroids (TBM, pericardial TB).
- Prevention:
- BCG Vaccine: At birth. Dose: 0.05 mL ID (<1mo), 0.1 mL ID (≥1mo). Protects vs severe TB.
- TB Preventive Treatment (TPT):
- Isoniazid (H) 6 months for contacts & high-risk (HIV+).
- Shorter: 3HP (H+Rifapentine weekly x3mo), 3RH (H+R daily x3mo).
⭐ Rifampicin: potent CYP450 inducer (↓ OCP, ARV efficacy).

High‑Yield Points - ⚡ Biggest Takeaways
- BCG vaccine prevents severe TB forms (miliary, TBM), not primary infection.
- Mantoux test (TST): >10 mm positive; >5 mm in HIV/immunocompromised/malnourished children.
- Gastric aspirate/induced sputum for bacteriological confirmation in young children.
- Primary progressive disease is common in children under 5 years.
- Most common: Intrathoracic TB (hilar/paratracheal lymphadenopathy).
- Extrapulmonary TB (EPTB) is frequent; lymph node TB (scrofula) is most common EPTB.
- Standard regimen: 2HRZE + 4HR (DOTS); watch for Ethambutol ocular toxicity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

