HA Overview & Types - Red Cell Rundown
- Hemolytic Anemia (HA): Premature RBC destruction (lifespan < 100-120 days); anemia if marrow compensation fails.
- Key Markers: Reticulocytosis, ↑LDH, ↑Indirect Bilirubin, ↓Haptoglobin (more in IVH).
- Classification:
- Site:
- Intravascular (IVH): In circulation; severe; schistocytes.
- Extravascular (EVH): In spleen/liver; common; spherocytes.
- Cause:
- Intrinsic: Defect within RBC (e.g., membrane, enzyme, Hb).
- Extrinsic: External factor damaging RBC (e.g., immune, mechanical).
- Site:
⭐ Extravascular hemolysis (e.g., in spleen, liver) is more common and generally less severe than intravascular hemolysis.
HA Diagnosis - Spotting the Signs
- Clinical Clues: Pallor, jaundice (icterus), splenomegaly, dark urine (hemoglobinuria).
- Initial Labs (The "Hemolysis Panel"):
- CBC: ↓Hb, ↓Hct.
- Peripheral Smear: Key for morphology (e.g., spherocytes, schistocytes).
- Reticulocyte Count: ↑ (Reticulocyte Production Index, RPI > 2-3).
- LDH: ↑ (marker of cell breakdown).
- Indirect Bilirubin: ↑.
- Haptoglobin: ↓ (binds free Hb).
- Urine: Hemoglobinuria, hemosiderinuria.
- Specific Tests:
- Direct Antiglobulin Test (DAT/Coombs): Positive in AIHA.
⭐ A reticulocyte count corrected for anemia (Reticulocyte Production Index, RPI > 2-3) is the hallmark of hemolytic anemias, indicating appropriate bone marrow response.
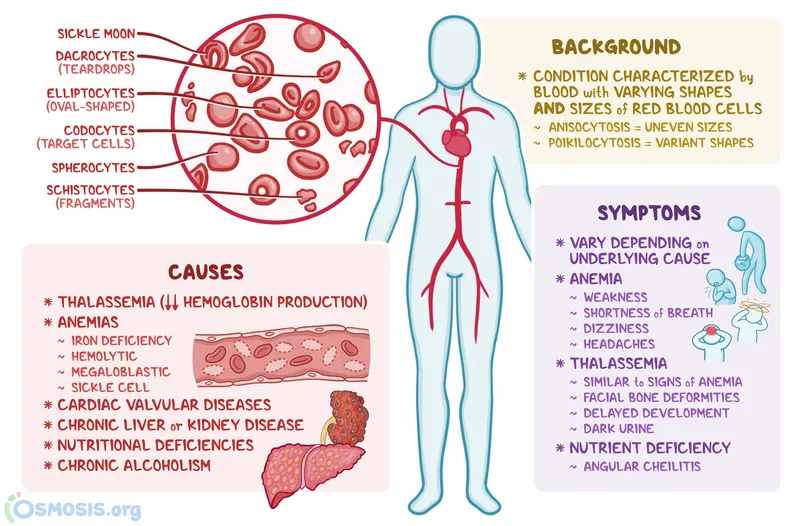
Inherited HA - Born This Way
- RBC Membrane Defects: Structural abnormalities leading to premature RBC destruction.
- Hereditary Spherocytosis (HS): Most common inherited HA in Northern Europeans. Autosomal Dominant (AD) typically (75%). Defects in ankyrin, spectrin, band 3, or protein 4.2.
- Clinical Triad: Anemia, jaundice, splenomegaly. Gallstones common. Aplastic crisis (Parvovirus B19).
- Labs: Spherocytes (↓MCV, ↑MCHC), reticulocytosis. Osmotic fragility test (+), EMA binding test (flow cytometry) is diagnostic.
- Rx: Folic acid. Splenectomy for moderate/severe cases (usually after age 5-6 years) cures hemolysis but spherocytes persist.
- Hereditary Elliptocytosis (HE) & Pyropoikilocytosis (HPP): Spectrin defects. HE often asymptomatic or mild; HPP is severe.
- Hereditary Spherocytosis (HS): Most common inherited HA in Northern Europeans. Autosomal Dominant (AD) typically (75%). Defects in ankyrin, spectrin, band 3, or protein 4.2.
- RBC Enzyme Defects: Impaired RBC metabolism.
- G6PD Deficiency: X-linked recessive. Most common enzyme defect. ↓G6PD → ↓NADPH → oxidative stress vulnerability.
⭐ In G6PD deficiency, acute hemolysis is typically triggered by oxidative stress (e.g., drugs like primaquine, infections, fava beans), leading to Heinz body formation.
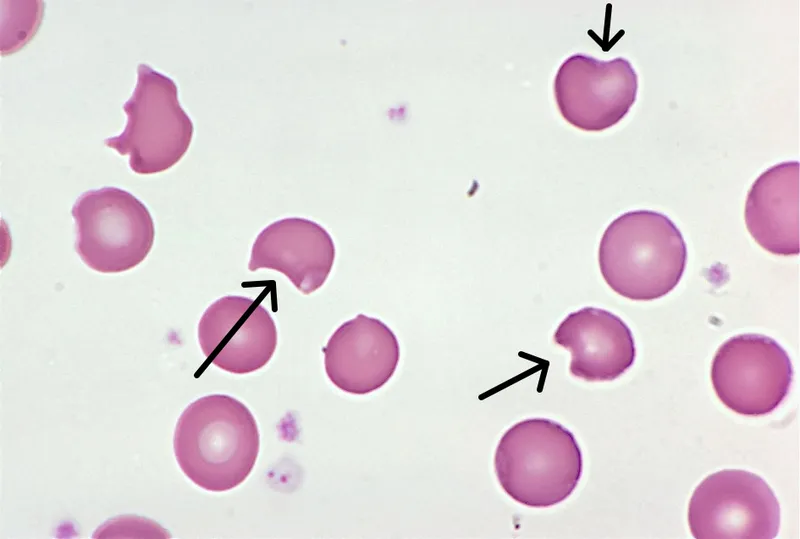
- Labs: Heinz bodies (denatured Hb, visible with crystal violet/supravital stain), bite cells. G6PD enzyme assay (NB: perform weeks after acute episode as young RBCs have higher G6PD).
- Pyruvate Kinase (PK) Deficiency: Autosomal Recessive (AR). ↓ATP → rigid RBCs → extravascular hemolysis. Second most common enzyme defect.
- Clinical: Neonatal jaundice, chronic hemolysis, splenomegaly. No specific crisis triggers like G6PD.
- Labs: Echinocytes (burr cells). PK enzyme assay.
- G6PD Deficiency: X-linked recessive. Most common enzyme defect. ↓G6PD → ↓NADPH → oxidative stress vulnerability.
Acquired HA - Attack from Outside
- Immune-Mediated:
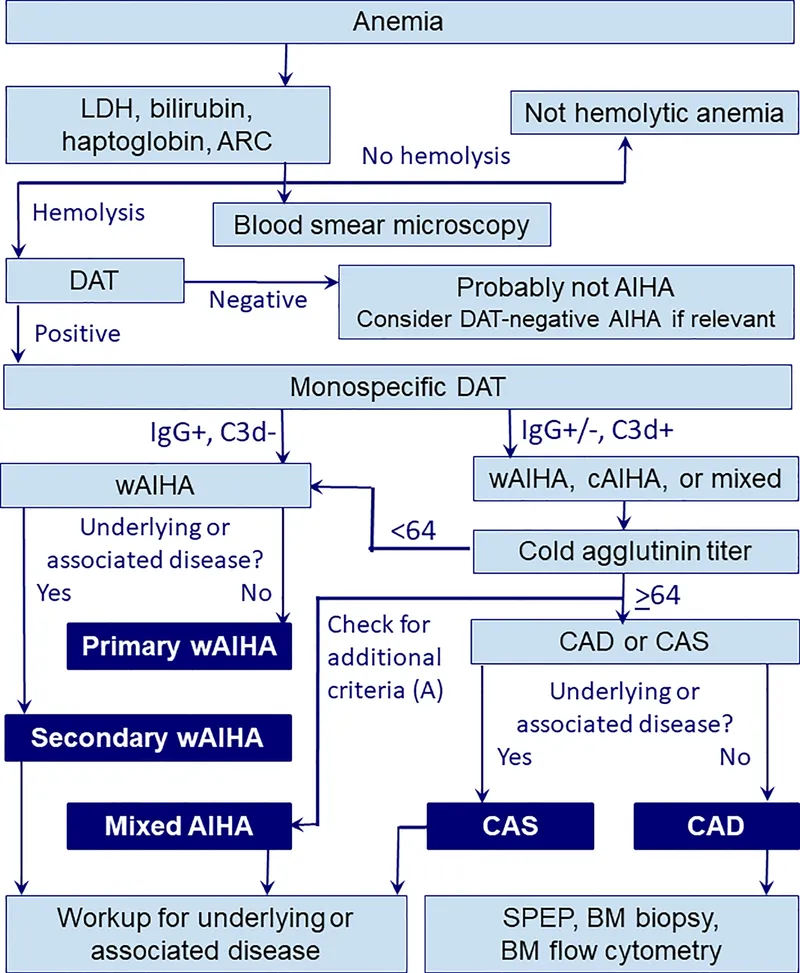
- Autoimmune (AIHA):
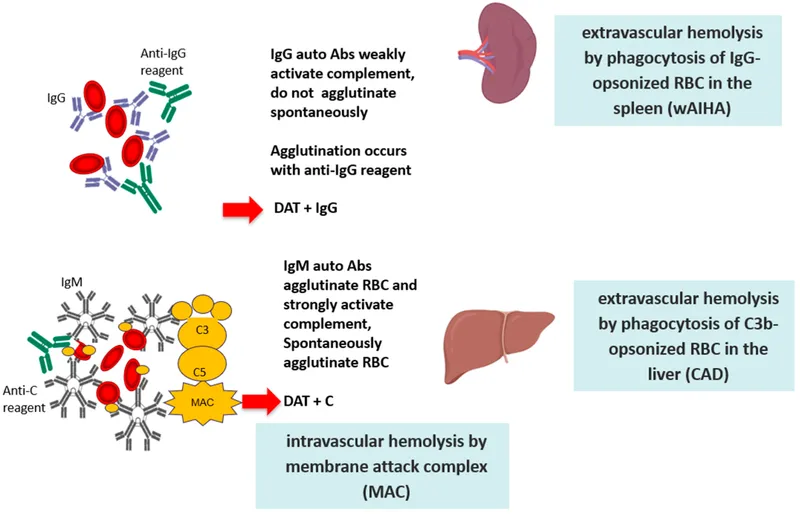
- Warm AIHA (IgG, extravascular hemolysis; DAT: IgG ± C3)
- Cold Agglutinin Disease (IgM, complement, intravascular hemolysis; DAT: C3)
- Paroxysmal Cold Hemoglobinuria (PCH; Donath-Landsteiner Ab, IgG)
- Alloimmune: Hemolytic Disease of Fetus & Newborn (HDFN; maternal IgG), Transfusion reactions.
- Autoimmune (AIHA):
- Non-Immune Mediated:
- Microangiopathic Hemolytic Anemia (MAHA): TTP, HUS, DIC; Schistocytes.
- Infections: Malaria, Clostridia, Babesia.
- Drugs/Toxins: e.g., Penicillin (immune), Dapsone (oxidative), Lead.
- Mechanical Trauma: Prosthetic valves, March hemoglobinuria.
- Paroxysmal Nocturnal Hemoglobinuria (PNH): Acquired GPI-anchor defect (↓CD55/CD59); intravascular hemolysis, thrombosis.
- Hypersplenism.
⭐ Warm AIHA is typically IgG-mediated and extravascular, while Cold Agglutinin Disease is IgM-mediated and can cause intravascular hemolysis upon cold exposure.
High‑Yield Points - ⚡ Biggest Takeaways
- Hereditary Spherocytosis: AD, spectrin defect; ↑ MCHC, positive osmotic fragility test.
- G6PD Deficiency: X-linked, episodic hemolysis from oxidant stress (drugs, fava); Heinz bodies, bite cells.
- Sickle Cell Anemia: HbS (Glu→Val); vaso-occlusion, autosplenectomy, Parvovirus B19 aplastic crisis.
- Beta-Thalassemia Major: Severe anemia, hepatosplenomegaly, "chipmunk facies" (extramedullary hematopoiesis), transfusion-dependent.
- AIHA: Warm (IgG) vs Cold (IgM); Direct Coombs Test is key diagnostic.
- PNH: Acquired PIGA mutation, CD55/CD59 deficiency; causes intravascular hemolysis, thrombosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more