Inflammatory Bowel Disease: Overview - Gut Feeling Gone Wrong
- Inflammatory Bowel Disease (IBD): Chronic, immune-mediated inflammation of the GI tract.
- Two main forms: Crohn's Disease (CD) and Ulcerative Colitis (UC).
- Pediatric peak incidence: 10-19 years.
- Key Differentiators:
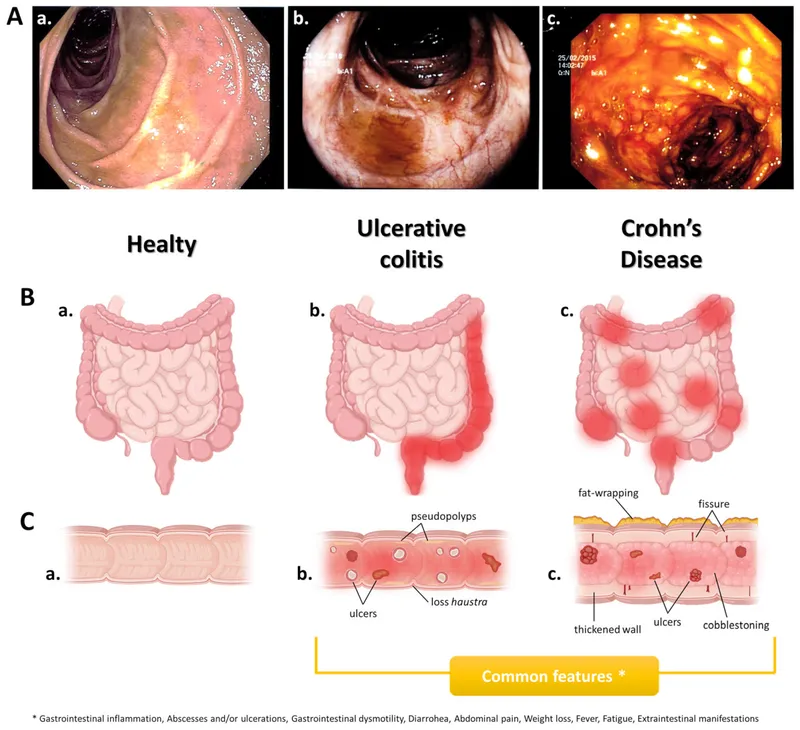
- CD: Any part of GIT (mouth to anus); transmural inflammation; skip lesions; "cobblestone" appearance; fistulas/strictures common.
- UC: Limited to colon (starts in rectum, extends proximally); mucosal/submucosal inflammation; continuous lesions; crypt abscesses.
⭐ Smoking is a risk factor for Crohn's Disease but is paradoxically protective for Ulcerative Colitis.
Inflammatory Bowel Disease: Etiopathogenesis - The Inside Story
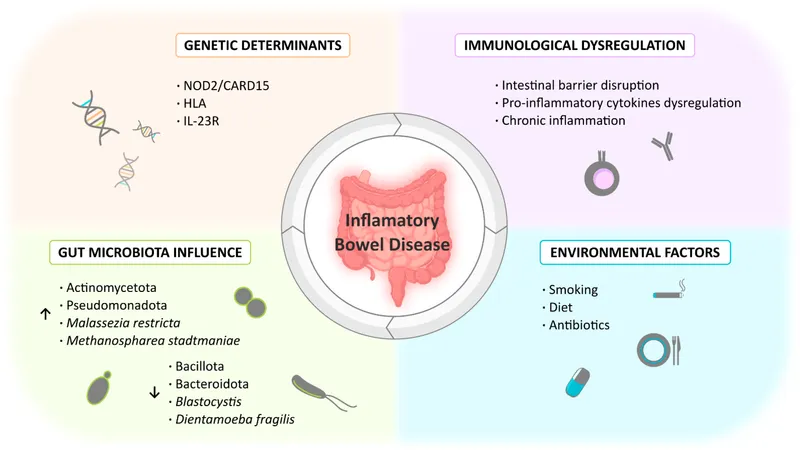
- Genetic Factors: Key genes include NOD2/CARD15 (Crohn's), IL23R, ATG16L1.
- Immune Dysregulation:
- Crohn's Disease (CD): Driven by Th1/Th17 pathways.
- Ulcerative Colitis (UC): Involves atypical Th2 response.
- Gut Microbiome: Dysbiosis (imbalance of gut bacteria) is a significant contributor.
- Environmental Triggers: Smoking (↑CD risk, ↓UC risk), diet, infections, NSAIDs.
⭐ NOD2/CARD15 gene mutations are the strongest genetic risk factor for Crohn's disease, particularly ileal involvement.
Inflammatory Bowel Disease: Clinical Features - Spotting the Signs
- Pediatric Hallmarks: Insidious onset common. Abdominal pain, chronic/nocturnal diarrhea (± blood), weight loss/poor gain, profound growth failure (key!). Unexplained fever, fatigue.
- CD vs. UC Comparison:
Feature Crohn's Disease (CD) Ulcerative Colitis (UC) Diarrhea Often non-bloody Usually bloody, urgent Abd. Pain RLQ, crampy LLQ, tenesmus Growth Failure Frequent, severe Less frequent Perianal Lesions Common (tags, fistulae) Rare Rectal Bleeding Less common Hallmark - Common Extraintestinal Manifestations (EIMs):
- Arthritis (peripheral > axial)
- Uveitis, episcleritis
- Erythema nodosum
- PSC (esp. with UC)
- Aphthous stomatitis

⭐ Growth failure may be the only sign of pediatric Crohn's Disease, often preceding GI symptoms.
Inflammatory Bowel Disease: Diagnosis - Unmasking IBD
- Key Labs: ↑ Fecal Calprotectin (FC >250 µg/g indicative), ↑CRP, ↑ESR. Anemia, hypoalbuminemia.
- Serology: ASCA (+ve CD), pANCA (+ve UC) - supportive; limited standalone utility.
- Endoscopy (Ileocolonoscopy + Upper GI) & Biopsy:
- CD: Skip lesions, aphthous ulcers, cobblestoning. Histo: Transmural inflammation, non-caseating granulomas.
- UC: Continuous inflammation (rectum proximally), superficial erosions. Histo: Crypt abscesses, cryptitis.
- Pediatric Activity: PCDAI (CD), PUCAI (UC) for severity.
⭐ Non-caseating granulomas on biopsy are highly specific for Crohn's Disease, though found in only ~30% of cases, guiding diagnosis.
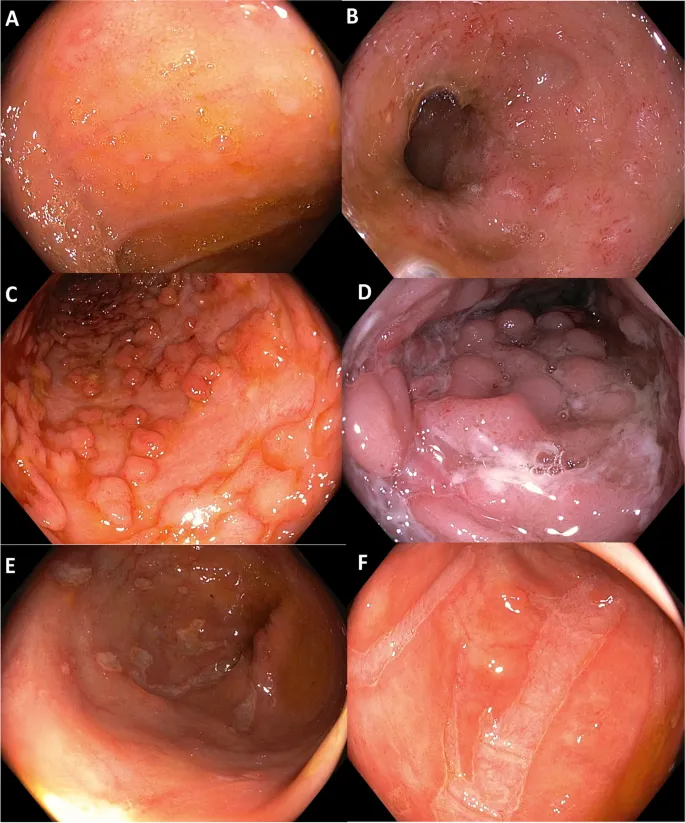 vs Ulcerative Colitis (continuous inflammation, crypt abscess))
vs Ulcerative Colitis (continuous inflammation, crypt abscess))
Inflammatory Bowel Disease: Management - Managing the Mayhem
Goals: Achieve clinical remission, mucosal healing, normal growth & Quality of Life (QoL).

- Nutrition: Crucial. EEN for CD induction. Nutritional support vital for growth & healing.
- 5-ASA (Mesalamine): Key in UC (induction/maintenance); limited role in pediatric CD.
- Surgery: For complications (e.g., strictures, fistulae, perforation) or failed medical Rx.
- Complications: Growth failure, delayed puberty, malnutrition, ↓bone health, ↑malignancy risk.
⭐ Exclusive Enteral Nutrition (EEN) is first-line for induction in pediatric Crohn's Disease, promoting mucosal healing & better nutrition.
High‑Yield Points - ⚡ Biggest Takeaways
- Crohn's Disease: Transmural inflammation, skip lesions, non-caseating granulomas; terminal ileum commonest site. ASCA positive. Complications: fistulas, strictures.
- Ulcerative Colitis: Mucosal inflammation, continuous lesions starting from rectum; bloody diarrhea is hallmark. p-ANCA positive. Risk: toxic megacolon, colorectal cancer.
- Pediatric IBD: Growth failure and delayed puberty are key presentations, often preceding GI symptoms.
- Diagnosis: Endoscopy with biopsy is gold standard. Fecal calprotectin indicates intestinal inflammation.
- EIMs: Common include arthritis, uveitis, skin manifestations (erythema nodosum, pyoderma gangrenosum), and PSC (esp. with UC).
- Treatment: Exclusive Enteral Nutrition (EEN) is first-line for pediatric CD induction. Others: 5-ASA, corticosteroids, immunomodulators, biologics.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

