Overview & Initial Approach - Spot the Source
- GIB: Bleeding from GI tract.
- UGIB: Proximal to Ligament of Treitz (e.g., varices, PUD).
- LGIB: Distal to Ligament of Treitz (e.g., Meckel's, intussusception).
- Initial Approach:
- ABCDE: Secure airway, IV access (2 large bore).
- Resuscitation: Crystalloids; blood if Hb < 7 g/dL or shock.
- History (medications, liver disease), exam (PR).
- Spot the Source:
- UGIB: Hematemesis, melena. NG aspirate: blood/coffee grounds.
- LGIB: Hematochezia (fresh/maroon blood).
⭐ In neonates, perform Apt-Downey test on bloody stools/vomitus to differentiate maternal vs. fetal blood.
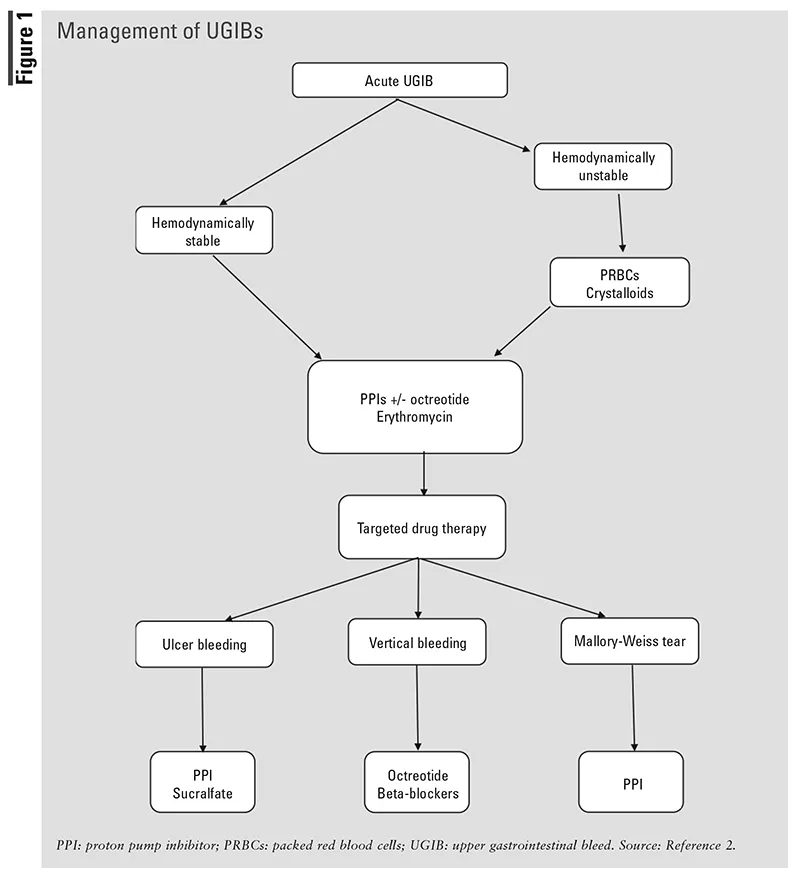
Upper GI Bleeding - Gullet Gushes
- Bleeding proximal to Ligament of Treitz.
- Presentation: Hematemesis (fresh red/coffee-ground), melena. Hematochezia in massive bleeds.
- Common Causes:
- Adults: Peptic Ulcer Disease (PUD) (>50%), varices, esophagitis, Mallory-Weiss tear.
- Children: Esophagitis, PUD, varices (portal HTN), gastritis.
- Initial Management:
- Secure ABCs; 2 large-bore IV lines; IV fluids (crystalloids, blood).
- IV Proton Pump Inhibitors (PPIs).
- Early endoscopy (diagnostic & therapeutic) within 24 hrs.
- Octreotide for suspected variceal bleed.
- Risk stratification: Rockall / Glasgow-Blatchford score.
⭐ Most common cause of significant upper GI bleeding is Peptic Ulcer Disease (PUD).
Lower GI Bleeding - Colon Carnage
- Bleeding distal to Ligament of Treitz. Presentation: hematochezia (BRBPR), maroon stools.
- Adult Causes:
- Diverticulosis: Commonest cause, typically painless, massive bleeding.
- Angiodysplasia: Painless arteriovenous malformations (AVMs), common in elderly.
- Colitis: Inflammatory Bowel Disease (IBD), ischemic, infectious (often painful).
- Neoplasms: Colorectal cancer (CRC), polyps (can be occult or frank bleeding).
- Anorectal: Hemorrhoids, fissures (bright red blood on toilet paper/surface).
- Pediatric Causes:
- Meckel's diverticulum (painless, brick-red stools).
- Intussusception (currant jelly stool, pain).
- Diagnosis & Management Pathway:
- Hemodynamic stabilization: ABCs, IV fluids, blood transfusion if Hb < 7 g/dL.
- Exclude Upper GI Bleed (e.g., nasogastric lavage if diagnosis unclear).
- Colonoscopy: Gold standard for diagnosis and potential therapy.
- If severe/obscure bleeding: CT Angiography (CTA), tagged RBC scan, then angioembolization or surgery.

⭐ Diverticulosis is the most common cause of significant lower GI bleeding in adults, typically presenting as acute, painless, large-volume hematochezia.
Diagnostic Tools & Management - Scope & Stop
- Stabilize: ABCs, IV access (2 large-bore), fluids, blood (Hb <7 g/dL or active bleed).
- Labs: CBC, coags (PT/INR, PTT), LFTs, RFTs, type & crossmatch.
- Endoscopy (Scope):
- EGD (UGIB): Within 24h. Diagnostic & therapeutic.
- Colonoscopy (LGIB): If stable + prep. CT Angio for brisk bleed.
- Capsule/Enteroscopy: Obscure GIB.
- Hemostasis (Stop):
- Endo-Therapy: Injection (adrenaline), thermal (cautery/APC), mechanical (clips/bands).
- Target: High-risk stigmata (Forrest Ia-IIb).
- Post-Scope/Failure: PPIs (UGIB). Repeat scope, IR (embolization), or surgery if refractory.
⭐ Active variceal bleeding: Endoscopic variceal ligation (EVL) is first-line therapy.
High‑Yield Points - ⚡ Biggest Takeaways
- Anal fissure is the most common cause of minor lower GI bleeding in infants.
- Suspect Meckel's diverticulum with painless, profuse rectal bleeding in young children.
- Intussusception classically presents with currant jelly stool and colicky abdominal pain.
- Neonatal hematemesis: Consider swallowed maternal blood; confirm with Apt-Downey test.
- Esophageal varices from portal hypertension cause severe upper GI bleeds.
- Infectious colitis (e.g., Shigella) causes bloody diarrhea, fever, and abdominal pain.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

