Thyroid Physiology - Neck's Powerhouse
- Axis: Hypothalamus (TRH) → Pituitary (TSH) → Thyroid (T3/T4). Negative feedback.
- Synthesis: Iodide trapping → Oxidation → Organification (Thyroid Peroxidase - TPO) → Coupling → Release.
- T4: Thyroxine (prohormone, major circulating); T3: Triiodothyronine (active, potent).
- Peripheral conversion: $T_4 \rightarrow T_3$ by deiodinases (e.g., D1, D2).
- Transport: Bound to Thyroxine-Binding Globulin (TBG, ~70%), albumin.
- Actions: ↑Basal Metabolic Rate (BMR), essential for brain/somatic growth, ↑catecholamine sensitivity.

⭐ Wolff-Chaikoff effect: Excess iodide transiently inhibits TPO & organification, ↓T3/T4 synthesis.
Hypothyroidism - The Slowdown Show
Thyroid hormone deficiency → metabolic slowdown. Early Dx & Rx critical.
- Congenital Hypothyroidism (CH): Most common preventable cause of intellectual disability.
- Screening: Neonatal, Day 3-5 (TSH ↑, T4/FT4 ↓). Treat by 2 weeks.
- Causes: Dysgenesis (85%, e.g., ectopic thyroid), dyshormonogenesis.
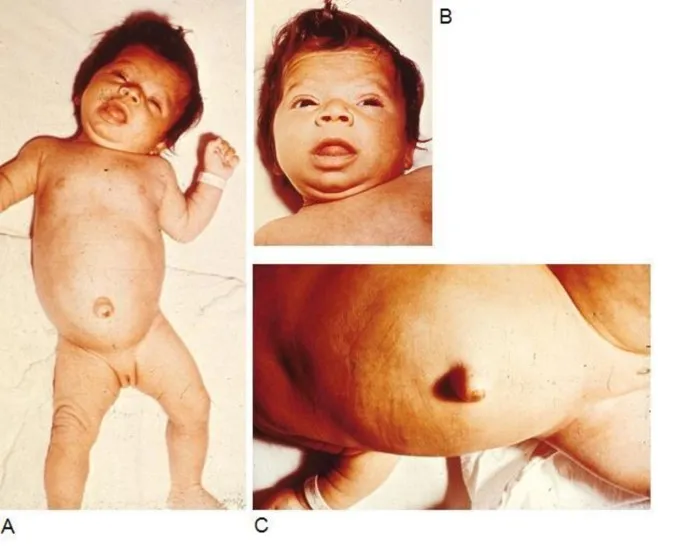
- Clinical: "Quiet baby", prolonged jaundice, macroglossia, umbilical hernia, hoarse cry, poor feeding, hypotonia.
- Acquired Hypothyroidism:
- Causes: Hashimoto's thyroiditis (autoimmune, most common >6 yrs, goiter, +Anti-TPO Ab), iodine deficiency.
- Clinical: Growth failure (↓ height velocity), ↓ school performance, cold intolerance, constipation, dry skin, lethargy.
- Diagnosis: ↑ TSH, ↓ T4/FT4 (primary).
- Treatment: Levothyroxine (e.g., CH: 10-15 µg/kg/day). Monitor TSH.
⭐ Neonatal screening for CH is crucial. Early levothyroxine (ideally within 2 weeks of birth) prevents irreversible intellectual disability.
Hyperthyroidism - The Overdrive Orchestra
- Etiology:
- Graves' disease (most common): Autoimmune, TSH-Receptor Antibodies (TRAb) positive.
- Neonatal thyrotoxicosis: Transplacental maternal TRAb; transient (3-12 weeks).
- Rare: Toxic adenoma, McCune-Albright syndrome, iodine-induced.
- Clinical Features: "Thyroid on overdrive"
- Weight loss (despite ↑appetite), heat intolerance, hyperactivity, anxiety, poor school performance.
- Cardio: Tachycardia, palpitations, widened pulse pressure.
- Goiter: Diffuse, firm (±bruit).
- Graves' specific: Exophthalmos, lid lag, proptosis.
- Growth: Accelerated linear growth, advanced bone age, later potential for short stature if untreated.
- Diagnosis:
- ↓TSH, ↑Free T4 (FT4), ↑Free T3 (FT3).
- TRAb positive in Graves' disease.
- Thyroid Ultrasound: Diffuse goiter, ↑vascularity (thyroid inferno).
- Management:
- Anti-thyroid drugs (ATDs):
- Methimazole (MMI): Preferred. Initial dose 0.2-0.5 mg/kg/day (max 30 mg/day).
- Propylthiouracil (PTU): For thyroid storm or MMI intolerance/allergy. Risk: severe hepatotoxicity.
- β-blockers (e.g., Propranolol): Symptomatic relief (tachycardia, tremors).
- Definitive Therapy (if ATDs fail/contraindicated): Radioactive Iodine (RAI) or Thyroidectomy.
- Anti-thyroid drugs (ATDs):
- Thyroid Storm (Thyrotoxic Crisis):
- Life-threatening: Hyperthermia, severe tachycardia, delirium, heart failure.
- Rx: PTU (first), Iodides (Lugol’s/SSKI, ≥1hr after PTU), Propranolol, Corticosteroids. 📌 Mnemonic: PIPS (PTU, Iodides, Propranolol, Steroids).

⭐ In children, methimazole is the first-line antithyroid drug; PTU is reserved for specific situations like thyroid storm or MMI allergy/intolerance due to its black box warning for severe liver injury and vasculitis.
Thyroid Nodules & Goiter - Neck Check-up
- Goiter: Thyroid gland enlargement.
- Types: Diffuse (smooth; e.g., Graves', early Hashimoto's), Nodular (lumpy).
- Pediatric Causes: Iodine deficiency (endemic areas), Hashimoto's thyroiditis, Graves' disease, dyshormonogenesis.
- Thyroid Nodules (Pediatrics):
- Less common vs. adults, but ↑ malignancy risk (~20-25%).
- Risk Factors for Malignancy: Hx radiation, family Hx thyroid Ca, rapid growth, firm/hard, fixed, cervical LAD, hoarseness.
- Evaluation: TSH, Ultrasound (USG).
- USG High-Risk: Microcalcifications, irregular margins, taller-than-wide, hypoechoic.
⭐ Malignancy risk in pediatric thyroid nodules is ~20-25%, significantly higher than adults.
- Neck Examination:
- Inspect: Swelling, symmetry, movement with swallowing.
- Palpate: Size, consistency (soft, firm, hard), mobility, tenderness. Assess cervical lymph nodes.
High‑Yield Points - ⚡ Biggest Takeaways
- Congenital hypothyroidism (CH): most common preventable cause of intellectual disability; newborn screening (↑TSH, ↓T4) is vital.
- CH causes: worldwide iodine deficiency; iodine-sufficient areas: thyroid dysgenesis (ectopic most common).
- Juvenile hypothyroidism: presents with growth failure, declining school performance, and delayed bone age.
- Graves' disease: most common cause of pediatric hyperthyroidism; look for exophthalmos, goiter, ↑T4/T3, ↓TSH.
- Neonatal thyrotoxicosis: transient, in infants of mothers with Graves' disease (transplacental TSH-receptor antibodies).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

