Intro & Screening - Lipid Patrol Start
- Definition: Abnormal pediatric lipid levels (NHLBI/AAP). Atherosclerosis risk from childhood → adult CVD.
- LDL-C: Acc <110, Borderline 110-129, High ≥130 mg/dL.
- Triglycerides (TG) (0-9y): Acc <75, Borderline 75-99, High ≥100 mg/dL.
- TG (10-19y): Acc <90, Borderline 90-129, High ≥130 mg/dL.
- Types: Hypercholesterolemia, hypertriglyceridemia, low HDL-C, mixed.
- Screening:
- Universal: 9-11 yrs & 17-21 yrs. 📌 '9-11 call for lipids, 17-21 for a clean scene'.
- Selective (>2y): Risk factors (FamHx CVD/lipids, obesity, DM, HTN, smoking, CKD, Kawasaki+aneurysms, post-transplant).
- Test: Fasting Lipid Profile (FLP) (preferred); Non-HDL-C (alternative).
⭐ Universal lipid screening: once at 9-11 years, again at 17-21 years.

Etiology - Root Cause Roundup
- Primary (Genetic):
- Monogenic:
- Familial Hypercholesterolemia (FH): AD; LDLR/APOB/PCSK9 mutations.
- Familial Defective ApoB100.
- Autosomal Recessive Hypercholesterolemia (ARH/LDLRAP1).
- Polygenic hypercholesterolemia.
- Familial Combined Hyperlipidemia (FCHL).
- Hypertriglyceridemia: LPL/ApoCII deficiency.
- Monogenic:
- Secondary (Acquired/Lifestyle):
- Obesity (most common).
- Unhealthy diet (↑sat/trans fats, sugar).
- Sedentary lifestyle.
- Diabetes Mellitus (T1 & T2).
- Hypothyroidism.
- Nephrotic syndrome.
- Cholestatic liver disease.
- Medications (corticosteroids, isotretinoin, antipsychotics, protease inhibitors).
- 📌 Mnemonic: 'Obese Kids Have Nasty Lipid ProfileS' (Obesity, Kawasaki, Hypothyroid, Nephrotic, Liver, PCOD, Steroids).
⭐ Familial Hypercholesterolemia (FH) is the most common genetic disorder causing severe elevations in LDL cholesterol and premature atherosclerotic cardiovascular disease.
Clinical Clues & Dx - Spotting Saboteurs
- Often asymptomatic. Family Hx: premature CAD, dyslipidemia, sudden death.
- Signs (severe/genetic, esp. FH):
- Tendon xanthomas (Achilles, hands, feet).
- Xanthelasmas (eyelids).
- Arcus cornealis (< 45 yrs).
- Pancreatitis with severe ↑TG.
- Dx: Fasting lipid profile. Non-HDL-C = $TC - HDL-C$.
- LDL-C (Friedewald): $LDL-C = TC - HDL-C - (TG/5)$; if TG < 400 mg/dL.
- Direct LDL-C if TG ≥ 400 mg/dL.
- Exclude secondary causes: Glucose, TSH, LFTs, urinalysis.
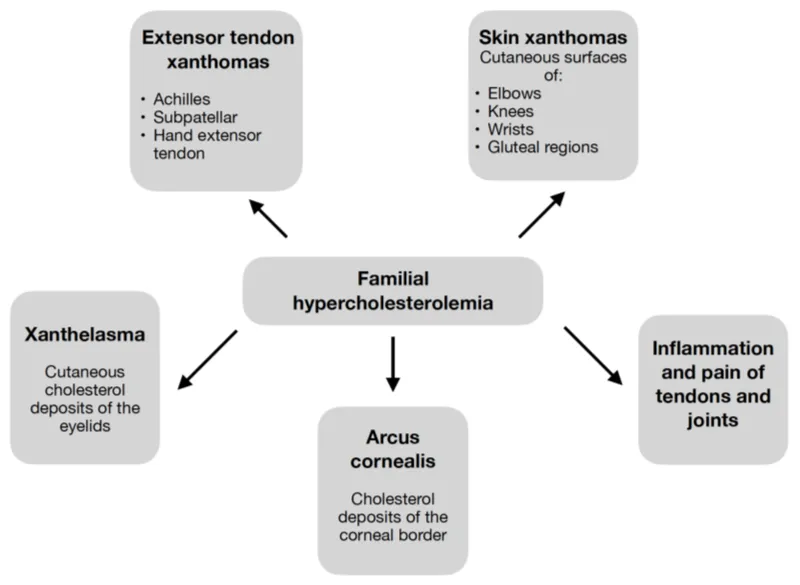
⭐ Tendon xanthomas in a child strongly suggest Familial Hypercholesterolemia (homozygous/severe heterozygous).
Management - Lipid Takedown Plan
1. Goals:
- LDL-C: <130 mg/dL (general); <100 mg/dL (high-risk, e.g., FH, post-transplant).
2. Lifestyle Modifications (LSM) - Cornerstone:
- Diet: CHILD-1 (>2 yrs); CHILD-2 if targets unmet. Family-based approach.
- Activity: ≥60 minutes/day moderate-to-vigorous.
- Weight management; Smoking prevention.
3. Pharmacotherapy:
- Indications (Age ≥10 yrs; ≥8 for severe FH):
- LDL-C ≥190 mg/dL (despite LSM).
- LDL-C ≥160 mg/dL + (Family Hx early CVD or ≥2 risk factors).
- LDL-C ≥130 mg/dL + Diabetes.
- Drugs:
- Statins (1st line): e.g., Pravastatin, Atorvastatin (check age approvals).
- Ezetimibe (if statin intolerant/insufficient).
- Bile Acid Sequestrants (BAS).
- Fibrates (for severe hypertriglyceridemia TG >500 mg/dL, post-LSM).
- PCSK9 inhibitors (for severe refractory FH, specialist use).
4. Monitoring:
- Lipid profile, LFTs (baseline, periodic with statins), CK (if myalgia).
⭐ For children with LDL-C ≥190 mg/dL despite 3-6 months of lifestyle therapy, statin medication is typically recommended starting at age 10 years (or earlier in severe FH).
High‑Yield Points - ⚡ Biggest Takeaways
- Universal screening: ages 9-11 & 17-21 years.
- Selective screening: high-risk children (family Hx, obesity, DM).
- Lifestyle modification (diet, exercise) is first-line management.
- Statins: first-line drug if lifestyle fails; for LDL-C ≥190 mg/dL (or ≥160 mg/dL + risks).
- Target LDL-C: <130 mg/dL (general); <100 mg/dL (high-risk).
- Suspect Familial Hypercholesterolemia (FH) with very high LDL-C & family Hx.
- Rule out secondary causes (e.g., hypothyroidism, nephrotic syndrome, drugs).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

