Varicose Veins - Twisted Troubles
- Dilated, tortuous, elongated superficial veins; primarily in legs.
- Etiology: ↑ Intra-abdominal pressure (pregnancy, obesity, chronic constipation), prolonged standing, DVT history, congenital valve weakness, female sex, family history.
- Pathophysiology: Superficial venous hypertension due to valvular incompetence (reflux) or venous obstruction. Perforator incompetence allows blood from deep to superficial veins, ↑ pressure.

- Clinical Features: Asymptomatic, cosmetic concerns, aching, throbbing, heaviness, itching, swelling, skin changes (pigmentation, eczema, lipodermatosclerosis), ulceration (venous ulcers, typically medial malleolus).
⭐ Most common site: Great Saphenous Vein (GSV) and its tributaries.
- Complications: Superficial thrombophlebitis, bleeding, chronic venous insufficiency, ulceration.
- 📌 Trendelenburg Test: Differentiates saphenofemoral junction (SFJ) incompetence from perforator incompetence (Perthes test for deep vein patency).
Varicose Veins Clinical & Complications - Signs & Soreness
- Symptoms:
- Leg aching, heaviness, fatigue, burning, or throbbing; worse with prolonged standing, relieved by elevation.
- Night cramps, itching (pruritus) over veins.
- Ankle swelling (edema), especially in evening.
- Signs:
- Dilated, tortuous, bluish superficial veins (GSV/SSV territories common).
- Visible/palpable varicosities.
- Pitting ankle edema.
- Tenderness along affected veins.
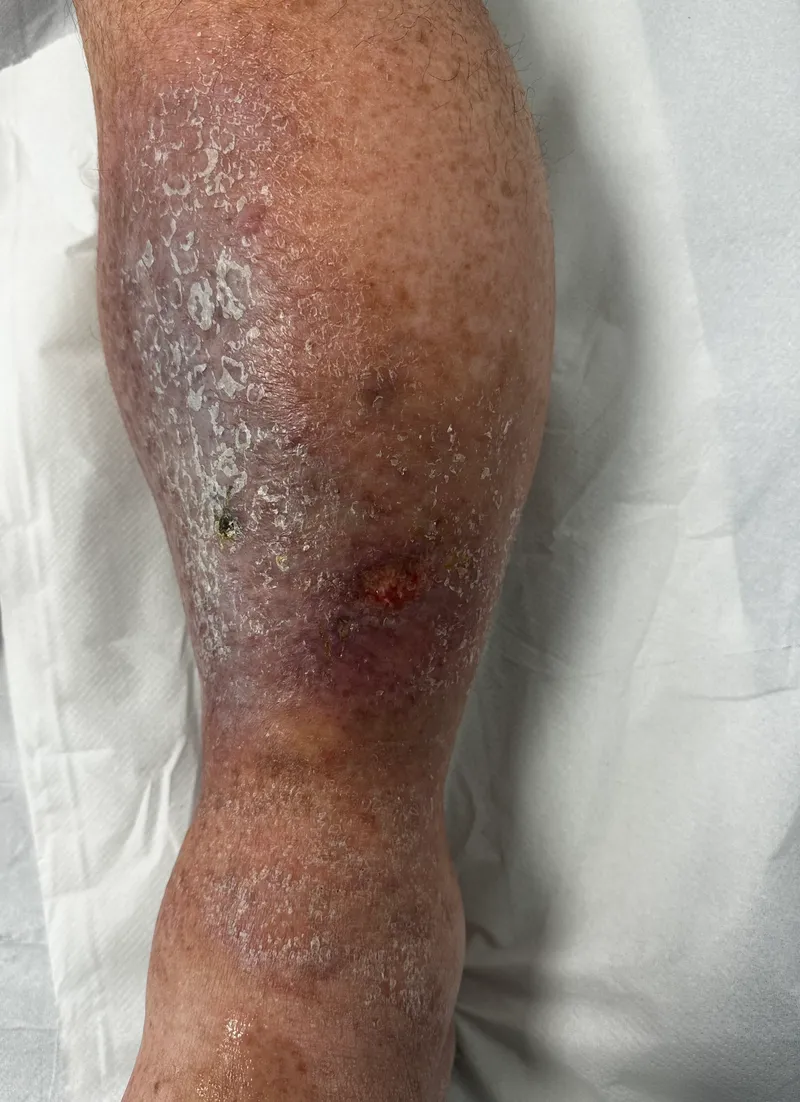
- Complications (Chronic Venous Insufficiency - CVI):
- Skin Changes:
- Corona phlebectatica (ankle flare).
- Hemosiderin pigmentation (brownish).
- Stasis dermatitis/Venous eczema: itching, scaling, weeping.
- Lipodermatosclerosis: induration, fibrosis, "inverted champagne bottle" leg.
- Atrophie blanche: white, stellate scars.
- Venous Ulcers: Medial malleolus commonest; shallow, irregular, painful.
- Superficial thrombophlebitis: painful, tender, palpable cord.
- Bleeding from varices (can be profuse).
- Secondary lymphedema.
- Skin Changes:
⭐ Lipodermatosclerosis signifies severe CVI, with chronic inflammation and fibrosis of skin and subcutaneous tissues.
Lymphatic Disorders - Drainage Dilemmas
- Lymphedema: Chronic tissue swelling from impaired lymphatic drainage.
- Progression: Early pitting edema → late non-pitting (brawny) induration.
- Skin changes: Thickening, hyperkeratosis, papillomatosis, peau d'orange; "buffalo hump" (foot dorsum).
- Stemmer's sign +ve: Inability to tent skin at base of 2nd toe.
- Complications: Recurrent cellulitis/lymphangitis, fungal infections, Stewart-Treves syndrome (lymphangiosarcoma in chronic cases, e.g., post-mastectomy).
⭐ Milroy disease is an autosomal dominant congenital lymphedema, typically affecting lower limbs, caused by mutations in the VEGFR3 (FLT4) gene.
- Lymphangitis: Inflammation of lymphatic channels. Red, painful subcutaneous streaks; fever. Often Strep. pyogenes.
- Chylous Effusions: Accumulation of chyle (lymphatic fluid rich in TGs) in body cavities (e.g., chylothorax) due to thoracic duct injury/obstruction.
High‑Yield Points - ⚡ Biggest Takeaways
- Varicose veins: dilated, tortuous superficial veins, typically in legs.
- Pathogenesis: venous valve incompetence → ↑ intraluminal pressure & stasis.
- Key risks: obesity, pregnancy, prolonged standing, family history.
- Complications: stasis dermatitis, ulceration, poor healing, superficial thrombophlebitis.
- Lymphedema: interstitial fluid accumulation from impaired lymphatic drainage.
- Types: Primary (e.g., Milroy disease - congenital); Secondary (e.g., filariasis, post-surgery, malignancy - acquired).
- Lymphangitis: acute inflammation of lymphatic channels, commonly streptococcal.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

