Lung Development Defects - Embryo's Oopsies
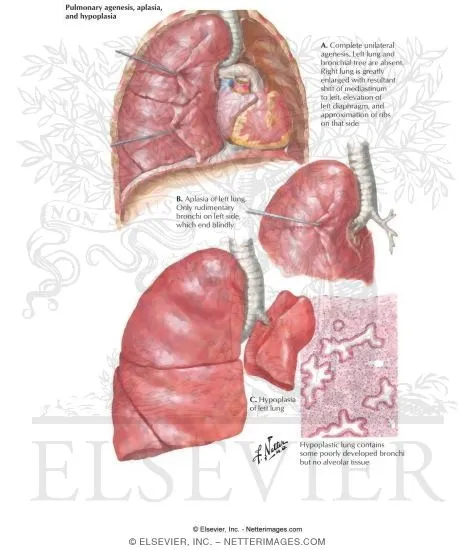
- Pulmonary Agenesis: Complete absence of lung tissue & bronchus.
- Pulmonary Aplasia: Rudimentary bronchus present, no lung parenchyma.
- Pulmonary Hypoplasia: ↓ lung volume & weight for gestational age; ↓ acini & alveoli.
- Often secondary to conditions limiting thoracic space or ↓ amniotic fluid.
⭐ Pulmonary hypoplasia is strongly associated with oligohydramnios (e.g., Potter sequence) and congenital diaphragmatic hernia.
- Causes of Hypoplasia:
- Congenital Diaphragmatic Hernia (CDH): Abdominal contents in thorax.
- Oligohydramnios: Insufficient amniotic fluid (e.g., renal agenesis - Potter sequence).
- Chest wall abnormalities: e.g., Jeune syndrome.
- Reduced fetal breathing movements.
Cystic Anomalies - Bubbly Troubles
- Developmental cystic lung lesions; often present with a "bubbly" appearance on imaging.
Congenital Pulmonary Airway Malformation (CPAM)
- Hamartomatous proliferation of terminal bronchioles; typically communicates with the airway.
- Presents: Neonatal respiratory distress, recurrent infections. Risk: Pneumothorax, malignancy.
⭐ Congenital Pulmonary Airway Malformation (CPAM) Type 1 is the most common type and generally has a good prognosis.
| CPAM Type (Stocker) | Approx. Freq. | Cyst Characteristics | Prognosis | Key Features/Associations |
|---|---|---|---|---|
| Type 0 | Rare | Acinar dysgenesis/agenesis | Fatal | Tracheal/bronchial atresia; incompatible with life |
| Type 1 | ~60-70% | Large, single/multiple (2-10 cm) | Good | Most common type |
| Type 2 | ~15-20% | Small, multiple (<2 cm) | Poorer | Associated with other congenital anomalies |
| Type 3 | ~5-10% | Microcystic/Solid-appearing | Poor | Bulky lesion, often affects entire lobe |
| Type 4 | ~5-10% | Large, peripheral, thin-walled | Variable | 📌 Risk of pleuropulmonary blastoma |
- Results from abnormal budding of the ventral foregut or tracheobronchial tree.
- Typically mediastinal or intrapulmonary; lined by ciliated columnar epithelium; wall may contain cartilage, smooth muscle, and bronchial glands.
- Usually solitary, round/oval, fluid or mucus-filled; does NOT typically communicate with the airway.
- Presents: Often asymptomatic; may cause symptoms due to compression (e.g., dyspnea, dysphagia) or infection.
Sequestration & CLE - Lost & Found Lung Bits
⭐ Pulmonary sequestrations are characterized by non-functional lung tissue that receives systemic arterial blood supply, not from pulmonary arteries.
Pulmonary Sequestration: Non-functional lung tissue, no normal airway connection; systemic arterial supply.
- Types: Intralobar (ILS) & Extralobar (ELS).
| Feature | Intralobar (ILS) | Extralobar (ELS) |
|---|---|---|
| Location | Within lung (LLL common) | Separate mass (L-sided, subphrenic) |
| Pleura | Shared visceral pleura | Own visceral pleura |
| Venous Drainage | Pulmonary veins (mostly) | Systemic veins (azygos, hemiazygos) |
| Presentation | Older; recurrent pneumonia | Neonates; resp. distress, anomalies |
| Anomalies | Rare (10%) | Common (60%); CDH, CCAM |
Congenital Lobar Emphysema (CLE):
- Progressive overdistension of lobe(s); LUL > RML > RUL.
- Cause: Bronchial check-valve (cartilage defect).
- Symptoms: Neonatal respiratory distress, wheezing.
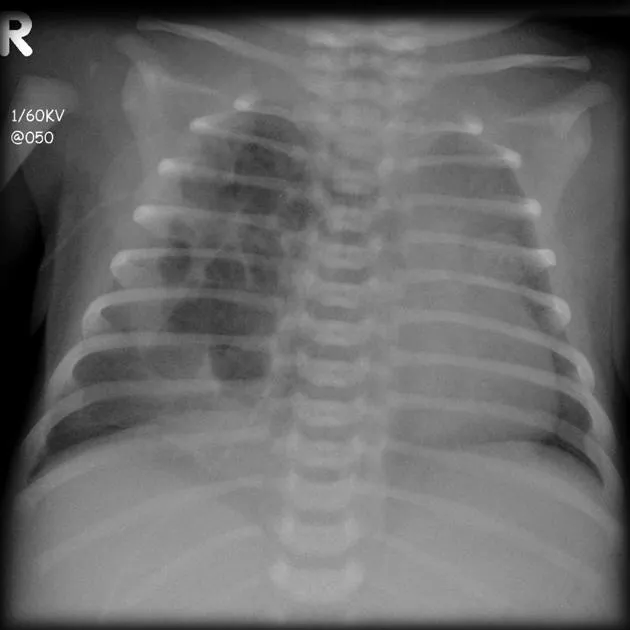
- CXR: Hyperlucent lobe, mediastinal shift, compressed lung.
Tracheoesophageal Fistula - Wrong Pipes

- Abnormal connection between trachea & esophagus; often with Esophageal Atresia (EA).
- Associations: VACTERL (Vertebral, Anal, Cardiac, Tracheo-Esophageal, Renal, Limb defects), Trisomy 13, 18, 21.
- Clinical Triad (infants):
- Choking/coughing/cyanosis with feeds
- Excessive salivation/drooling
- Respiratory distress
- Diagnosis: Inability to pass NG tube; X-ray (coiled NG tube, air in stomach for distal TEF).
⭐ The most common type of tracheoesophageal fistula is Esophageal Atresia with a distal TEF (Gross Type C, ~85% of cases), often presenting with polyhydramnios in utero.
High‑Yield Points - ⚡ Biggest Takeaways
- Pulmonary Sequestration: Non-functional lung, systemic arterial supply, no bronchial connection.
- CPAM: Hamartomatous cystic airway lesion; Type 1 (large cysts) best prognosis.
- Bronchogenic Cysts: Mediastinal foregut cysts, respiratory epithelium lining.
- CDH: Bochdalek type (posterolateral) commonest, causes pulmonary hypoplasia.
- TEF: Esophageal atresia with distal fistula (Type C) most common; polyhydramnios link.
- Pulmonary Hypoplasia: Incomplete lung development, from oligohydramnios or CDH.
- CLE: Progressive lobar overinflation, due to bronchial cartilage defect.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

