UTI Overview - Urinary Unrest
- Definition: Microbial invasion & inflammation of urinary tract.
- Key Terms:
- Bacteriuria: Bacteria in urine. Significant if >105 CFU/mL (mid-stream clean catch).
- Pyuria: WBCs in urine (>10 WBCs/μL or >5 WBCs/HPF).
- Classification:
- Lower UTI: Cystitis, urethritis.
- Upper UTI: Pyelonephritis.
- Uncomplicated vs. Complicated (e.g., male, pregnant, catheter, obstruction).

⭐ Escherichia coli is the most common uropathogen, accounting for ~80% of uncomplicated UTIs.
Microbial Villains & Vulnerabilities - Pathogen Parade
- Bacterial Culprits:
- Escherichia coli (UPEC): Dominant cause (~80%); P fimbriae (pyelonephritis), Type 1 fimbriae (cystitis).
- Staphylococcus saprophyticus: Young, sexually active females.
- Klebsiella pneumoniae: Often nosocomial, common in diabetics.
- Proteus mirabilis: Urease producer; associated with struvite stones, alkaline urine.
- Enterococcus faecalis: Nosocomial, elderly, post-instrumentation.
- Pseudomonas aeruginosa: Catheter-associated, resistant strains.
- Fungal:
- Candida albicans: Catheters, immunocompromised, post-antibiotics.
- Key Vulnerabilities:
- Female sex, sexual intercourse.
- Urinary stasis: Obstruction (BPH, calculi), neurogenic bladder.
- Catheterization (foreign body).
- Systemic factors: Diabetes Mellitus, pregnancy, immunosuppression.
- Anatomical: Vesicoureteral reflux (VUR).
⭐ Proteus mirabilis infection characteristically produces urease, leading to alkaline urine (pH > 7.0) and promoting struvite (magnesium ammonium phosphate) stone formation.
Infection's Invasion & Host Defense - Battle for Bladder
- Invasion Pathway:
- Uropathogens (e.g., UPEC) ascend urethra.
- Adherence to urothelium: P-fimbriae (Type 1 pili) bind mannose receptors; S-fimbriae.
- Biofilm formation; intracellular bacterial communities (IBCs) possible.
- Host Defense Arsenal:
- Mechanical: Flushing action of urine, complete bladder emptying.
- Mucosal Barriers:
- Glycosaminoglycan (GAG) layer: anti-adherent.
- Tamm-Horsfall protein (Uromodulin): binds bacteria, prevents attachment.
- Secretory IgA.
- Inflammatory Response: TLRs (e.g., TLR4 for LPS) → cytokine release (IL-6, IL-8) → neutrophil influx.
- Epithelial cell exfoliation.
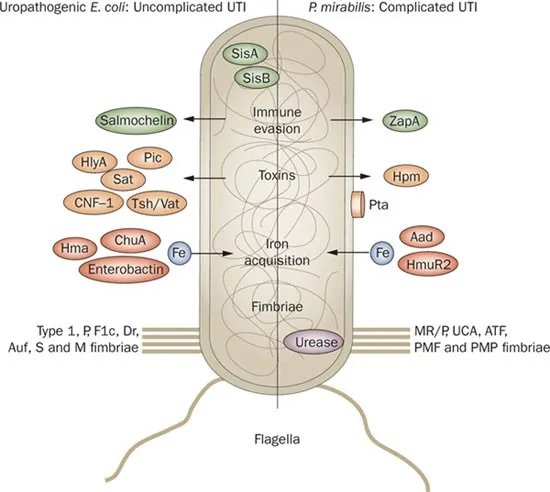
⭐ Uropathogenic E. coli (UPEC) can form Intracellular Bacterial Communities (IBCs) within bladder urothelial cells, acting as quiescent reservoirs that contribute to recurrent UTIs and antibiotic resistance persistence.
Clinical Clues & Diagnostic Drill - Symptom Sleuthing
- Symptom Spectrum:
- Lower UTI (Cystitis): Dysuria, frequency, urgency, suprapubic pain, ±hematuria.
- Upper UTI (Pyelonephritis): Fever, chills, flank pain/CVA tenderness, nausea/vomiting, ±cystitis symptoms.
- Elderly/Catheterized: Often atypical (e.g., confusion, fever without localizing signs).
- Diagnostic Approach:
- Key Lab Findings:
- Dipstick: Leukocyte esterase (LE) for pyuria; Nitrites for gram-negative bacteria (esp. Enterobacteriaceae).
- Microscopy: WBCs >5-10/HPF; Bacteria; WBC casts (hallmark of pyelonephritis).
- Culture (Gold Standard): ≥10^5 CFU/mL (mid-stream urine); ≥10^3 CFU/mL (symptomatic ♀); ≥10^2 CFU/mL (catheter).
⭐ WBC casts in urine sediment are pathognomonic for renal parenchymal inflammation, strongly suggesting pyelonephritis.
Complications & Chronic Concerns - Trouble Brewing
- Acute Storm:
- Pyelonephritis → perinephric/renal abscess, emphysematous pyelonephritis.
- Urosepsis, septic shock.
- Renal papillary necrosis (Key causes: DM, Analgesics, Sickle cell, Obstruction; 📌 POST CARD).
- Long-term Fallout:
- Chronic pyelonephritis: renal scarring, blunted calyces, thyroidization of tubules.
- Xanthogranulomatous pyelonephritis (XGP): destructive inflammation, foamy macrophages, often Proteus & staghorn calculi.
- ↑ Risk of CKD, hypertension.
- Recurrent infections.
- Pregnancy: ↑ pyelonephritis risk, preterm birth.
⭐ Xanthogranulomatous pyelonephritis (XGP) often presents as a unilateral renal mass mimicking renal cell carcinoma, associated with Proteus and staghorn calculi. oka
High‑Yield Points - ⚡ Biggest Takeaways
- Most common cause of UTI is E. coli (UPEC).
- Significant bacteriuria: >105 CFU/mL in mid-stream urine.
- Acute pyelonephritis presents with fever, flank pain, and WBC casts.
- Cystitis involves dysuria, frequency, urgency; typically no fever.
- Catheter-associated UTIs (CAUTI) are a major source of nosocomial infections.
- Treat asymptomatic bacteriuria in pregnant women to prevent pyelonephritis.
- Sterile pyuria may suggest renal tuberculosis or chlamydial infection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

