Intro & Causes - The Slow Burn
- Inflammation of prolonged duration (weeks to months).
- Characterized by co-existing:
- Active inflammation
- Tissue destruction
- Repair attempts (angiogenesis, fibrosis)
- Onset:
- May follow unresolved acute inflammation.
- May begin insidiously (de novo).
- Principal Causes:
- Persistent infections (e.g., Mycobacterium tuberculosis, Treponema pallidum, fungi, viruses).
- Hypersensitivity diseases (e.g., autoimmune: RA, IBD; allergic: asthma).
- Prolonged exposure to toxic agents (exogenous: silica; endogenous: cholesterol).

⭐ Infiltration with mononuclear cells (macrophages, lymphocytes, plasma cells) is a hallmark of chronic inflammation.
Cellular Players - The Chronic Crew
Persistent inflammation is orchestrated by a specialized cellular cast (📌 MLP-EM: Macrophages, Lymphocytes, Plasma cells, Eosinophils, Mast cells). These cells interact, releasing mediators sustaining the response and influencing tissue injury/repair.
| Cell | Origin/Key Features | Key Functions in Chronic Inflammation |
|---|---|---|
| Macrophages | Monocytes; M1 (classical), M2 (alternative) | Phagocytosis, Ag presentation, cytokines (TNF, IL-1, IL-6), growth factors |
| Lymphocytes | T-cells (CD4+, CD8+), B-cells | Bidirectional macrophage activation (IFN-γ, IL-12); adaptive immunity |
| Plasma Cells | Differentiated B-lymphocytes | Produce antibodies against persistent antigens/autoantigens |
| Eosinophils | Granulocytes; recruited by eotaxin | Helminth defense; IgE-mediated allergic reactions (MBP release) |
| Mast Cells | Tissue-resident; surface IgE receptors | Release histamine, leukotrienes, proteases, cytokines; modulate inflammation |
⭐ Epithelioid cells in granulomas are activated macrophages with abundant pink cytoplasm, resembling epithelial cells, key for granulomatous inflammation.
Mediators & Mechanisms - Fueling the Fire
- Key Mediators:
- Cytokines: Pro-inflam: TNF, IL-1, IL-6; IFN-γ (T-cell driven macrophage activation); IL-10 (anti-inflam), TGF-β (fibrosis).
- Chemokines: Attract specific leukocytes (e.g., MCP-1).
- Growth Factors: PDGF, FGF, TGF-β stimulate angiogenesis & fibrosis.
- Mechanisms:
- Persistent stimuli (microbes, irritants).
- Macrophage-Lymphocyte interactions: Bidirectional activation.
- Concurrent tissue injury & attempted repair (fibrosis).
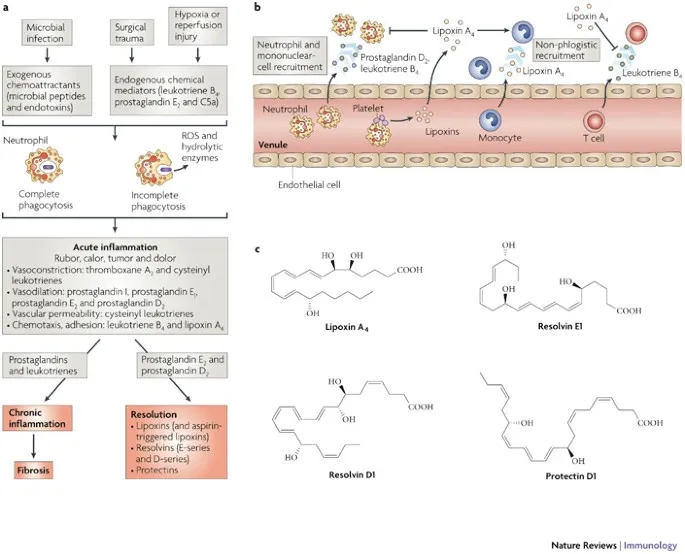
⭐ IFN-γ, produced by NK cells and T lymphocytes (Th1, CD8+), is the most potent endogenous macrophage-activating cytokine.
Granulomatous Inflammation - Walling Off Trouble
- Hallmark: Aggregates of activated macrophages (epithelioid cells), often with a collar of lymphocytes; may fuse to form multinucleated giant cells (e.g., Langhans, foreign body type).
- Purpose: To contain or "wall off" an offending agent that is difficult to eradicate.

| Type | Mechanism | Key Mediators | Examples |
|---|---|---|---|
| Immune | Persistent T-cell (Th1) response to antigen (Ag) | IFN-γ (activates Mφ) | Tuberculosis (caseating), Sarcoidosis (non-caseating), Leprosy, Fungal inf., Crohn's d. |
| Foreign Body | Inert material; direct Mφ activation | - | Sutures, talc, silica, asbestos, beryllium (can also be immune-mediated) |
Systemic Effects & Outcomes - The Body's Burden
- Fever: Persistent low-grade; IL-1, TNF mediated.
- Acute Phase Response:
- Liver: ↑CRP, SAA, Fibrinogen (IL-6 driven).
- Results in ↑ESR.
- Leukocytosis: ↑WBC count; pattern indicates etiology (e.g., neutrophilia, lymphocytosis).
- Anemia of Chronic Disease (ACD):
- IL-6 → ↑Hepcidin → ↓iron absorption & release.
- Cachexia: TNF-α (cachectin) causes muscle/fat loss.
- Secondary (AA) Amyloidosis: Chronic inflammation → ↑SAA → organ deposition.
⭐ ACD: Characterized by ↓ serum iron, ↓ TIBC, and normal/↑ ferritin.
High‑Yield Points - ⚡ Biggest Takeaways
- Chronic inflammation is characterized by prolonged duration and co-existing active inflammation, tissue injury, and healing attempts.
- Key cellular players are macrophages, lymphocytes (T and B cells), and plasma cells.
- Tissue destruction is often mediated by inflammatory cells and their products.
- Repair involves angiogenesis and fibrosis (scarring).
- Granulomatous inflammation (e.g., TB, sarcoidosis) features epithelioid macrophages and giant cells.
- Mediators include cytokines (e.g., TNF, IL-1, IFN-γ) and growth factors.
- Potential long-term sequelae include loss of function, fibrosis, and neoplastic transformation (e.g., chronic gastritis and cancer).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

