Regeneration & Cell Cycle - Repair Kickstart
- Regeneration: Ideal outcome; restores normal tissue. Requires intact Extracellular Matrix (ECM) & proliferative cells.
- Repair: Connective tissue deposition (scarring/fibrosis). Occurs if ECM is damaged or cells are permanent.
- Cell Types by Proliferative Capacity:
- Labile: Continuously dividing (e.g., epithelia, hematopoietic cells).
- Stable: Quiescent (G0), can divide if stimulated (e.g., hepatocytes, fibroblasts).
⭐ Liver shows remarkable regeneration; quiescent hepatocytes (stable cells) proliferate post-hepatectomy.
- Permanent: Terminally differentiated, minimal regeneration (e.g., neurons, cardiac muscle).
- Cell Cycle: G0 (quiescence) → G1 → S (DNA synthesis) → G2 → M (mitosis). Progression driven by cyclins & CDKs.

ECM & Growth Factors - Matrix & Movers
- Extracellular Matrix (ECM): Provides scaffold & signals.
- Collagens: Type III (early granulation), replaced by Type I (tensile strength).
- Elastin: Elasticity.
- Proteoglycans & Hyaluronan: Hydration, resilience, cell migration.
- Adhesion Glycoproteins: Fibronectin (scaffold, chemotaxis), Laminin (basement membrane), Integrins (cell-ECM linkage).
- Key Growth Factors (GFs): Regulate cell proliferation, migration, differentiation.
- PDGF: Recruits macrophages, fibroblasts, smooth muscle cells.
- FGFs (esp. FGF-2): Angiogenesis, fibroblast proliferation, ECM protein synthesis.
- TGF-β: Key fibrogenic agent; stimulates collagen/fibronectin synthesis, inhibits MMPs.
- VEGF: Angiogenesis, ↑ vascular permeability.
- EGF/TGF-α: Stimulate keratinocyte & fibroblast proliferation.

⭐ TGF-β is a potent fibrogenic agent, stimulating fibroblast chemotaxis, collagen synthesis, and inhibiting MMPs, but also has anti-inflammatory effects in later stages of repair.
Phases of Wound Healing - The Healing Timeline
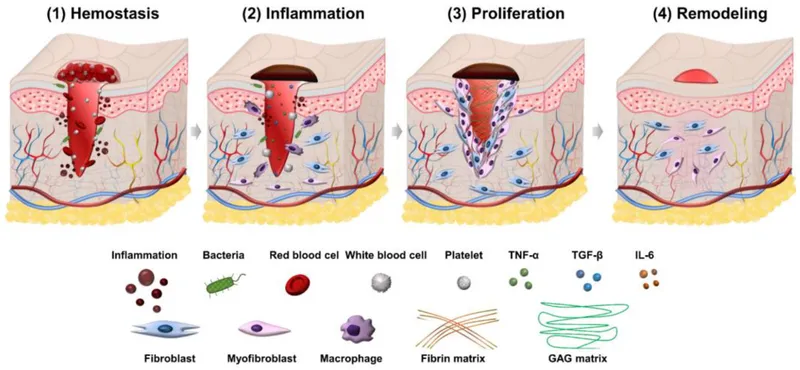
- 1. Inflammatory Phase (0-3 days): Initial response.
- Hemostasis (Immediate): Vasoconstriction, platelet plug, coagulation cascade → fibrin clot. Stops bleeding.
- Inflammation:
- Neutrophils (PMNs): Peak 24-48 hrs. Phagocytose debris, bacteria.
- Macrophages (M1): By 48-96 hrs. Phagocytosis, release growth factors (TGF-β, PDGF, VEGF). Orchestrate repair.
- 2. Proliferative Phase (Day 3 - Weeks): Filling wound defect.
- Granulation Tissue: Hallmark. Pink, soft. Consists of:
- Fibroblasts: Synthesize Type III collagen, ECM.
- Angiogenesis: New capillaries (VEGF, FGF-2).
⭐ Granulation tissue, hallmark of the proliferative phase, is characterized by angiogenesis (new blood vessels) and fibroblast proliferation, appearing pink and soft.
- Re-epithelialization: Keratinocyte migration & proliferation.
- Wound Contraction: Myofibroblasts reduce defect size.
- Granulation Tissue: Hallmark. Pink, soft. Consists of:
- 3. Remodeling Phase (Maturation) (Weeks - Months/Years): Scar development.
- Collagen Remodeling: Type III collagen → Type I. Fibers organize & cross-link.
- Tensile Strength: ↑ progressively. ~20% at 3 wks, max ~70-80% of original.
- Scar Maturation: Becomes paler, flatter, avascular.
Healing Intentions & Complications - Smooth or Scarred
- Primary Intention: Clean, sutured wounds; minimal tissue loss. Rapid healing, small scar.
- Secondary Intention: Large defects, infected wounds. More inflammation, granulation, contraction; larger scar. (e.g., ulcers, burns)
Factors Impairing Healing:
- Systemic: ↓Nutrition (Protein, Vit C, Zinc), Diabetes, ↓Circulation, Glucocorticoids.
- Local: Infection (commonest delay), mechanical stress, foreign bodies, ↓perfusion.
Complications:
- Deficient Scar:
- Wound dehiscence (rupture)
- Ulceration
- Excessive Scar Formation:
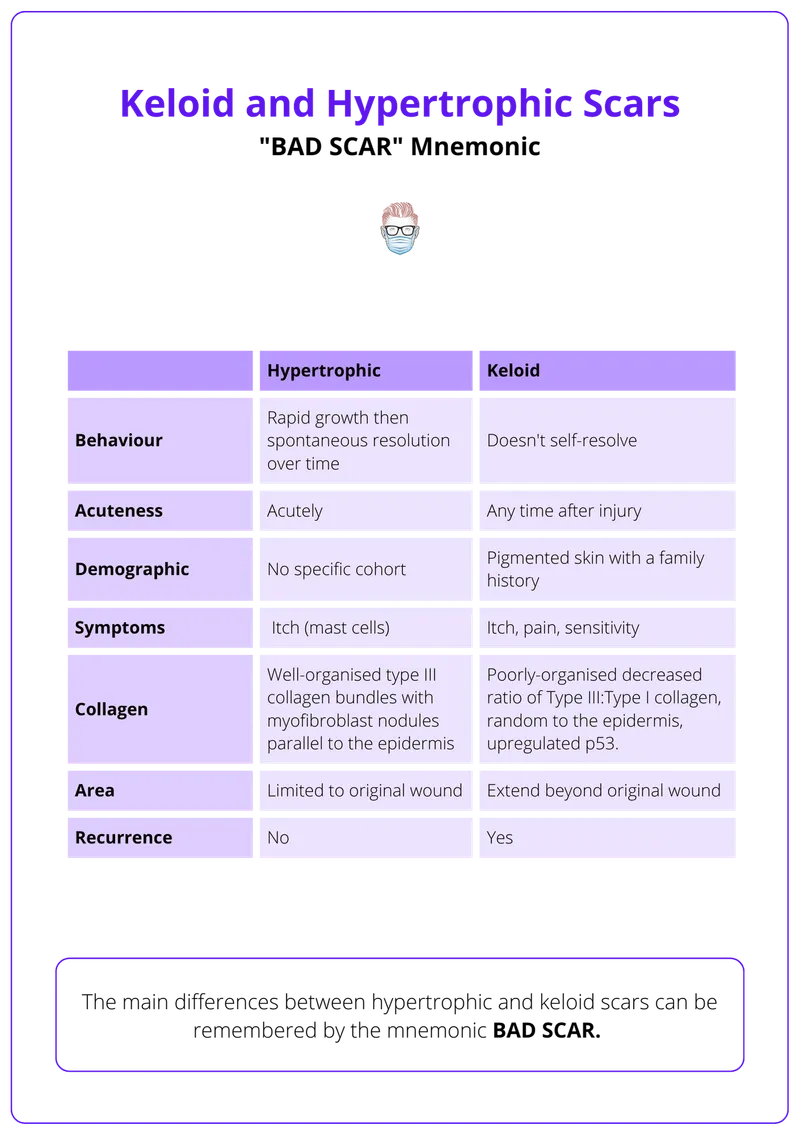
- Hypertrophic Scar: Raised, within wound borders; may regress. Type III collagen.
- Keloid: Extends beyond borders; rarely regresses, recurs. Disorganized Type I & III. 📌 African descent.
⭐ Keloids are composed predominantly of disorganized Type I and III collagen, extend beyond the original wound borders, do not regress, and often recur after excision.
- Contractures: Exaggerated contraction; causes deformities, limits movement (e.g., severe burns).
High‑Yield Points - ⚡ Biggest Takeaways
- Wound healing phases: Inflammation, Proliferation (granulation tissue), and Remodeling (collagen maturation, scar formation).
- Macrophages are key, releasing growth factors (TGF-β, PDGF, VEGF) that orchestrate repair processes.
- Granulation tissue is characterized by fibroblasts, new capillaries (angiogenesis), and inflammatory cells.
- Collagen transition: Type III collagen (early, weak) is replaced by Type I collagen (late, strong).
- Secondary intention healing: More granulation, significant wound contraction (myofibroblasts), and larger scars.
- Keloids involve excessive collagen beyond wound borders; Vitamin C is crucial for collagen synthesis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

