Intro & Pathophysiology - Gut's Little Outpouchings
- Diverticulosis: Presence of uninflamed diverticula (outpouchings).
- Diverticulitis: Inflammation and infection of diverticula.
- True vs. False Diverticula (📌 Key Difference):
- True: Involves all three gut wall layers (mucosa, submucosa, muscularis propria). E.g., Meckel's diverticulum.
- False (Pulsion/Pseudodiverticula): Herniation of mucosa and submucosa through the muscularis propria at weak points. Common in colon.
⭐ False diverticula (pulsion type) are common in the colon, lacking a muscularis propria layer.
- Commonest Location: Sigmoid colon (~95%); narrowest segment, highest intraluminal pressure (Law of Laplace).
- Epidemiology: ↑ with age; >50% by 60 years. Prevalence: Western > Asian populations.
- Risk Factors: Low-fibre diet, obesity, sedentary lifestyle, chronic constipation, smoking, NSAIDs.
- Pathophysiology:
- Segmental ↑ intraluminal pressure (e.g., from straining with low-bulk stools).
- Focal areas of weakness in colonic wall, typically where vasa recta penetrate the muscularis propria.
- Altered colonic motility and structure (e.g., elastin changes).
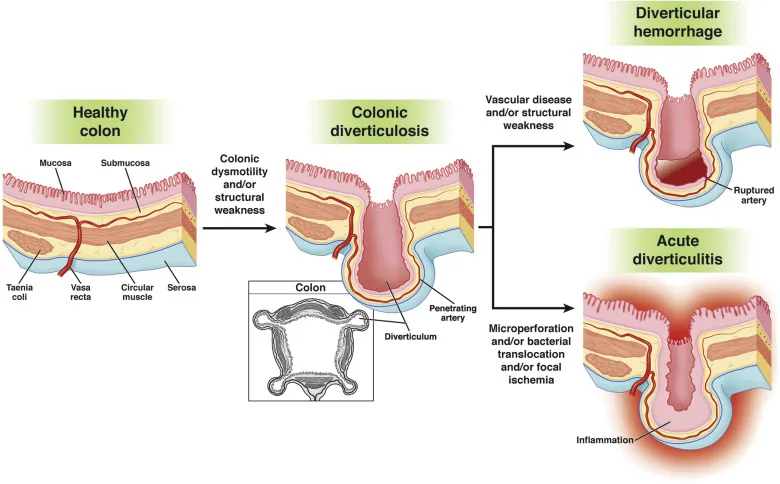
Symptoms & Complications - When Pockets Inflame
- Diverticulosis:
- Mostly asymptomatic.
- May cause vague symptoms: bloating, chronic constipation, intermittent crampy LLQ discomfort.
- Acute Diverticulitis:
- Acute, persistent LLQ pain (📌 'left-sided appendicitis').
- Fever (often low-grade), nausea, vomiting.
- Altered bowel habits (constipation > diarrhea).
- Leukocytosis common.

- Complications: (Mnemonic: 📌 "FAB-PPHS" - Fistula, Abscess, Bleeding (Hemorrhage), Perforation, Phlegmon, Stricture)
- Abscess: Most common; localized pus.
- Phlegmon: Diffuse pericolic fat inflammation/cellulitis.
- Fistula: 📌 Colovesical (most common; M>F) → pneumaturia, fecaluria, recurrent UTIs. Others: colovaginal, coloenteric.

⭐ The most common type of fistula in complicated diverticulitis is a colovesical fistula, presenting with pneumaturia or fecaluria.
- Perforation: Contained (abscess) or Free (peritonitis → surgical emergency).
- Stricture/Obstruction: Chronic inflammation → fibrosis, luminal narrowing.
- Hemorrhage: Painless, arterial; often from right-sided diverticula (typically in diverticulOSIS).
- Hinchey Classification (Perforated Diverticulitis):
Diagnosis & Management - Spotting & Soothing Strategies
- Diagnosis: Diverticulosis
- Often incidental finding (colonoscopy, barium enema).
- Diagnosis: Acute Diverticulitis
- CT scan (abdomen/pelvis with contrast): Investigation of choice. Shows inflamed diverticula, wall thickening, pericolic fat stranding, abscess.

- ⚠️ Avoid colonoscopy/barium enema in acute phase (risk of perforation).
- Labs: CBC (↑leukocytosis), ↑CRP.
⭐ Contrast-enhanced CT scan of the abdomen and pelvis is the gold standard for diagnosing acute diverticulitis and its complications.
- Management: Asymptomatic Diverticulosis
- High-fibre diet, hydration, physical activity.
- Management: Symptomatic Uncomplicated Diverticulosis
- Fibre, antispasmodics (controversial).
- Management: Acute Diverticulitis
- Management: Acute Uncomplicated Diverticulitis
- Outpatient: Clear liquid diet, oral broad-spectrum antibiotics (e.g., ciprofloxacin + metronidazole for 7-10 days).
- Management: Acute Complicated Diverticulitis
- Hospitalization, NPO, IV fluids, IV antibiotics.
- Percutaneous drainage for abscess >3-4 cm.
- Surgery for perforation, obstruction, fistula, or failure of medical management (e.g., Hartmann's procedure).
High‑Yield Points - ⚡ Biggest Takeaways
- Diverticulosis: Acquired false diverticula (mucosa/submucosa herniation) of the colon.
- Sigmoid colon is the most common site due to highest intraluminal pressure.
- Low-fiber diet is a key etiological factor.
- Diverticulitis: Inflammation/infection of diverticula; presents with LLQ pain, fever, and leukocytosis.
- Most common complication: Diverticulitis; painless, massive lower GI bleeding also occurs.
- Colovesical fistula is the most frequent fistula type following diverticulitis.
- CT scan is preferred for diagnosing acute diverticulitis; colonoscopy is contraindicated in the acute phase due to perforation risk.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

