Pancreatic Islets & DM Patho - Islet Insights
- Islet Cells & Hormones: (📌 A-G, B-I, D-S, PP-P)
- α-cells: Glucagon (↑glucose)
- β-cells: Insulin (↓glucose), Amylin
- δ-cells: Somatostatin (inhibitory)
- PP (γ)-cells: Pancreatic Polypeptide
- Diabetes Mellitus (DM) Patho:
- T1DM: Autoimmune β-cell destruction (insulitis, Type IV HSR) → absolute insulin deficiency. HLA-DR3/DR4.
- T2DM: Insulin resistance + β-cell dysfunction → relative insulin deficiency. Islet amyloid (IAPP) deposition.
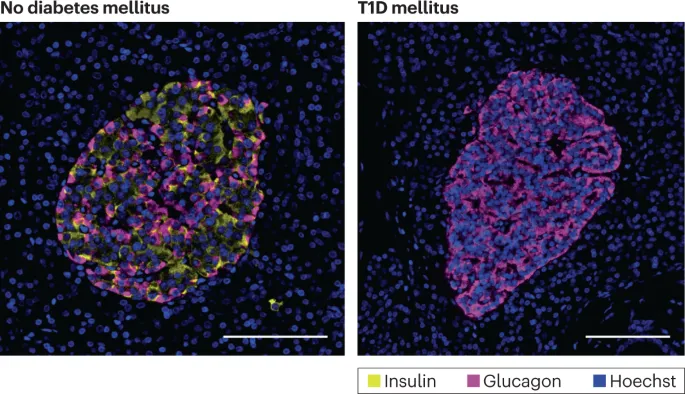
⭐ Insulitis (lymphocytic infiltration of islets) is pathognomonic for Type 1 DM.
Insulinoma - Sweet & Lowdown
- Most common functional PanNET; β-cell tumor secreting excess insulin.
- Clinical Features: Recurrent hypoglycemia.
- Neuroglycopenic: confusion, blurred vision, seizures, coma.
- Autonomic (adrenergic): sweating, palpitations, tremor, anxiety.
- Diagnosis:
- 📌 Whipple's Triad:
- Symptoms of hypoglycemia.
- Low plasma glucose (e.g., < 50 mg/dL).
- Relief of symptoms with glucose administration.
- Key Labs (during hypoglycemia): ↑ Insulin, ↑ C-peptide, ↑ Proinsulin; ↓ β-hydroxybutyrate.
- Negative oral hypoglycemic agent screen.
- 📌 Whipple's Triad:
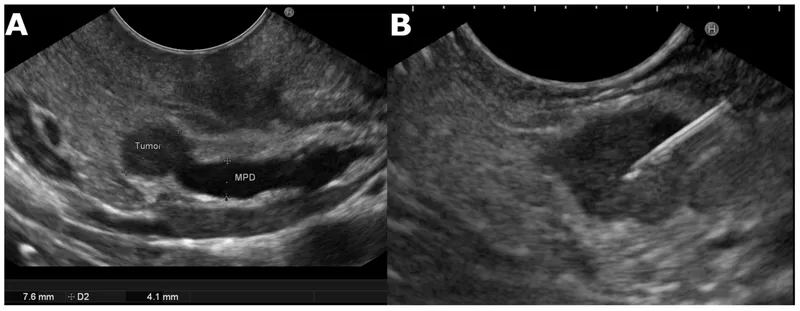
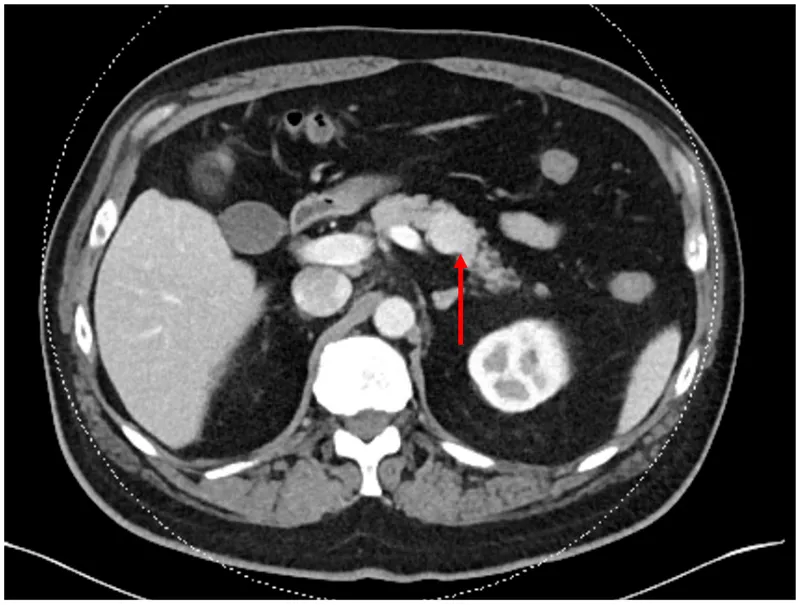
- Localization: Endoscopic ultrasound (EUS) is gold standard. CT/MRI.
- Pathology: Typically solitary, benign (>90%), small (<2cm). ~5-10% associated with MEN1.
- Treatment: Surgical resection (curative). Diazoxide, octreotide for unresectable cases.
⭐ Elevated C-peptide and proinsulin levels differentiate insulinoma from factitious hypoglycemia (exogenous insulin use).
Gastrinoma (ZES) - Acid Attack!
- Gastrin-secreting neuroendocrine tumor (NET) causing Zollinger-Ellison Syndrome (ZES).
- Locations: Duodenum (most common), pancreas. Often within the "Gastrinoma triangle".
- Pathophysiology: ↑ Gastrin → parietal cell hyperplasia → massive ↑ HCl secretion.
- Clinical Features:
- Multiple, refractory, or distal (e.g., jejunal) peptic ulcers.
- GERD, abdominal pain.
- Chronic diarrhea, steatorrhea (low pH inactivates pancreatic enzymes).
- Diagnosis:
- Fasting serum gastrin (FSG): > 100 pg/mL (suspect); > 1000 pg/mL with gastric pH < 2 (diagnostic).
- Secretin stimulation test: Paradoxical ↑ gastrin > 200 pg/mL from baseline.
- Endoscopy: Prominent gastric folds.
⭐ Approximately 20-30% of gastrinomas are associated with Multiple Endocrine Neoplasia type 1 (MEN1).
- Treatment: High-dose Proton Pump Inhibitors (PPIs); surgical resection if localized.
oka
Other PanNETs - Rare Hormone Havoc
| Tumor | Hormone ↑ | Key Features / Syndrome | Notes / Location | Malignancy |
|---|---|---|---|---|
| Glucagonoma | Glucagon | 📌 4 D's: Dermatitis (necrolytic migratory erythema - NME), Diabetes (mild), DVT, Depression | Tail/Body | High |
| VIPoma | VIP | WDHA Syndrome: Watery Diarrhea, Hypokalemia, Achlorhydria (Verner-Morrison) | Tail/Body | ~50% |
| Somatostatinoma | Somatostatin | Diabetes mellitus, cholelithiasis, steatorrhea, hypochlorhydria | Head/Periampullary | High |
⭐ Necrolytic migratory erythema (NME), an erythematous rash with blistering, crusting, and scaling, is a pathognomonic feature of glucagonoma.
High‑Yield Points - ⚡ Biggest Takeaways
- Insulinomas: Most common functioning PanNET, usually benign; cause hypoglycemia, Whipple's triad.
- Gastrinomas (ZES): Cause multiple peptic ulcers; often malignant and associated with MEN1 syndrome.
- Glucagonomas: Characterized by necrolytic migratory erythema, diabetes, and DVT.
- Type 1 DM: Autoimmune destruction of pancreatic β-cells leading to absolute insulin deficiency.
- Type 2 DM: Due to insulin resistance and relative insulin deficiency; islet amyloid deposition is common.
- VIPomas: Result in WDHA syndrome (Watery Diarrhea, Hypokalemia, Achlorhydria).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

