MDs vs Myopathies: Basics - Muscle Mayhem Kickoff
| Feature | Muscular Dystrophies (MDs) | Myopathies (General) |
|---|---|---|
| Nature | Genetic, progressive muscle fiber degeneration | Heterogeneous; acquired or inherited muscle disease |
| Defect | Muscle structural proteins (e.g., dystrophin) | Variable (inflammatory, metabolic, toxic, etc.) |
| Progression | Typically progressive weakness | Variable course; may be static or improve |
| Serum CK | Often markedly ↑↑ (DMD >10x ULN) | Variable (normal to significantly ↑) |
| Biopsy | Necrosis, regeneration, fibrosis, fatty change | Specific to cause (e.g., inflammation, vacuoles) |
Dystrophinopathies (DMD/BMD) - Dystrophin's Drama

- X-linked recessive; DMD gene (Xp21) defect → dystrophin protein deficiency.
- Dystrophin: anchors muscle fiber cytoskeleton (actin) to extracellular matrix.
- Duchenne Muscular Dystrophy (DMD):
- Frameshift/nonsense mutations → near absent/truncated dystrophin.
- Severe: onset <5 years, wheelchair by ~12 years, death by 20s-30s (respiratory/cardiac failure).
- Key signs: Gower's sign, calf pseudohypertrophy (fibrofatty replacement), markedly ↑CK.
- Becker Muscular Dystrophy (BMD):
- In-frame mutations → partially functional/reduced amount of dystrophin.
- Milder: later onset, slower progression, variable severity, longer lifespan.
- Diagnosis: ↑↑ Serum CK (DMD > BMD), genetic testing (confirmatory), muscle biopsy (dystrophin staining).
⭐ Serum Creatine Kinase (CK) levels are often >10x normal in DMD, typically highest in early childhood.
📌 DMD = Deleted/non-functional dystrophin (severe); BMD = Better/partially functional dystrophin (milder).
Other Major Dystrophies - Diverse Muscle Breakdown
- Myotonic Dystrophy (DM):
- DM1 (Steinert disease): Autosomal Dominant (AD). CTG repeat expansion (DMPK gene).
- Features: Myotonia (grip, percussion), progressive weakness (distal, facial, SCM), cataracts, frontal balding, cardiac conduction defects, testicular atrophy.
- 📌 Mnemonic: "My Tonia Can't Open Her Grip" (Myotonia, Cataracts, Open mouth/Hatchet facies, Heart block, Gonadal atrophy).
- DM2 (PROMM - Proximal Myotonic Myopathy): AD. CCTG repeat (CNBP gene). Milder; often proximal weakness, myalgia, cataracts.
- DM1 (Steinert disease): Autosomal Dominant (AD). CTG repeat expansion (DMPK gene).
- Facioscapulohumeral Dystrophy (FSHD):
- AD. D4Z4 repeat contraction (chromosome 4q35) → aberrant DUX4 gene expression.
- Features: Weakness of facial muscles (orbicularis oris/oculi), scapular winging (often asymmetric), humeral weakness (Popeye sign). Sensorineural hearing loss possible.
- Limb-Girdle Muscular Dystrophies (LGMDs):
- Genetically heterogeneous group. Progressive proximal muscle weakness (shoulder & pelvic girdles).
- Inheritance: Autosomal Dominant (LGMDD, e.g., LGMDD1 from DNAJB6) or Recessive (LGMDR, e.g., LGMDR1 from CAPN3).
- Key types: Calpainopathy (LGMDR1/LGMD2A), Sarcoglycanopathies (e.g., LGMDR3-6/LGMD2C-F), Dysferlinopathy (LGMDR2/LGMD2B).
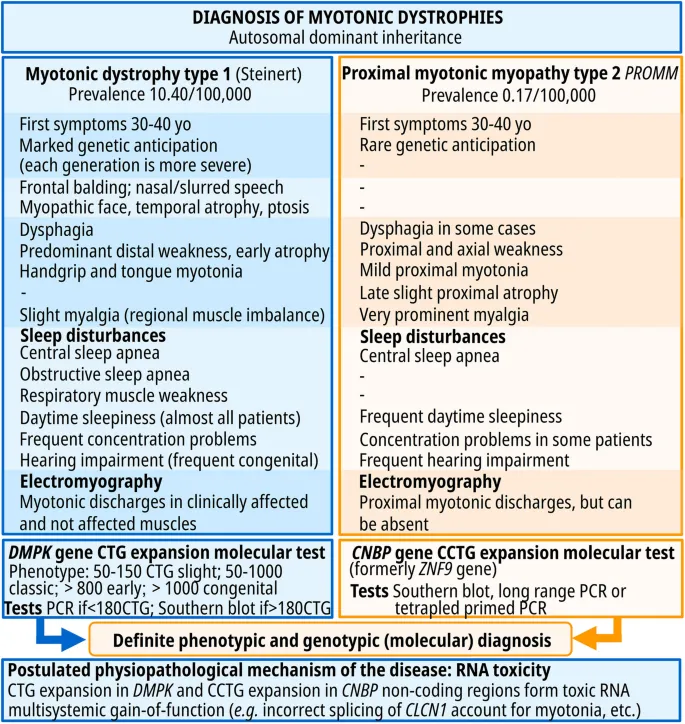
⭐ In Myotonic Dystrophy Type 1 (DM1), "anticipation" (earlier onset and increased severity in subsequent generations) is a key genetic feature due to the unstable CTG repeat expansion. EMG classically shows myotonic discharges ("dive-bomber" sound).
Congenital & Metabolic Myopathies - Inborn Muscle Flaws
- Congenital Myopathies: Infantile hypotonia, weakness; often static. Biopsy diagnostic.
- Central Core Disease: RYR1 gene.
⭐ Associated with malignant hyperthermia susceptibility.
- Nemaline Myopathy: Nemaline (rod) bodies (Z-band).
- Myotubular Myopathy: Central nuclei; X-linked (MTM1) common.
- Central Core Disease: RYR1 gene.
- Metabolic Myopathies: Exercise intolerance, cramps, rhabdomyolysis.
- Glycogenoses:
- McArdle (GSD V): Myophosphorylase def. 📌 "M" for Muscle, McArdle.
- Pompe (GSD II): Acid maltase def; cardiomegaly (infantile).
- Lipid Myopathy: CPT II def. (rhabdomyolysis trigger).
- Mitochondrial: "Ragged red fibers" (Gomori).
- Glycogenoses:
Mito & Inflammatory Myopathies - Energy & Immune Woes
Mitochondrial Myopathies:
- Defect: Impaired mitochondrial ATP production (energy failure).
- Histo: Ragged Red Fibers (RRF) on Gomori trichrome; "parking lot" inclusions (EM).
- Clinical: Proximal weakness, exercise intolerance, ophthalmoplegia, ptosis.
- E.g., MELAS, MERRF, Kearns-Sayre.
Inflammatory Myopathies:
- Patho: Immune-mediated muscle damage.
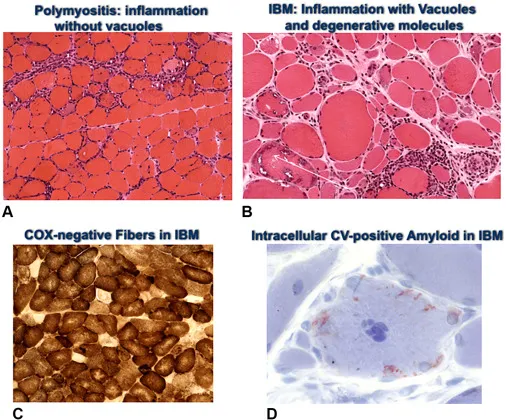
- Polymyositis (PM):
- CD8+ T-cell mediated; endomysial inflammation.
- Symmetrical proximal weakness.
- Dermatomyositis (DM):
- CD4+ T-cell, humoral; perifascicular atrophy, perimysial inflammation.
- Heliotrope rash, Gottron's papules.
⭐ Associated with ↑ risk of malignancy (e.g., ovarian, lung, GI).
- Inclusion Body Myositis (IBM):
- Affects individuals >50 years.
- Asymmetric weakness (distal > proximal); rimmed vacuoles.
High‑Yield Points - ⚡ Biggest Takeaways
- Duchenne Muscular Dystrophy (DMD): X-linked recessive, absent dystrophin (frameshift mutation), Gower's sign, markedly ↑ CK, calf pseudohypertrophy.
- Becker Muscular Dystrophy (BMD): Milder, X-linked, reduced/altered dystrophin (in-frame mutation), later onset.
- Myotonic Dystrophy (DM1): Autosomal dominant, CTG repeat expansion (DMPK gene), myotonia, cataracts, cardiac issues, frontal balding.
- Limb-Girdle Muscular Dystrophies (LGMDs): Genetically heterogeneous group, proximal muscle weakness of shoulder and pelvic girdles.
- Mitochondrial Myopathies: Exhibit ragged red fibers on Gomori trichrome stain, often with ophthalmoplegia and exercise intolerance.
- Dermatomyositis: Heliotrope rash, Gottron's papules/sign, perifascicular atrophy; associated with malignancy in adults.
- Polymyositis: Endomysial inflammation with CD8+ T cells, proximal muscle weakness, no significant skin involvement.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

