Open Fx Basics - Skin Deep Trouble
- Definition: Bone communicates with external environment; ↑ infection risk.
- Gustilo-Anderson Classification: Crucial for prognosis & management (Rx).
- Type I: Wound < 1 cm, clean; minimal muscle damage; simple/minimal comminution.
- Type II: Wound > 1 cm; moderate soft tissue (ST) damage; no flaps/avulsions; moderate comminution.
- Type IIIA: Extensive ST laceration, adequate coverage possible; or high-energy trauma; segmental/severe comminution.
- Type IIIB: Extensive ST loss, periosteal stripping, bone exposure; requires ST reconstruction (flap).
- Type IIIC: Associated arterial injury requiring repair, regardless of ST damage.

⭐ Infection rates correlate with Gustilo-Anderson grade: Type I (0-2%), Type II (2-7%), Type IIIA (~7% with aggressive Rx), Type IIIB (10-50%), Type IIIC (25-50%; amputation common).
Initial Care - Race Against Time
Follow ATLS. Prioritize: hemorrhage control, rapid IV antibiotics, neurovascular assessment, wound care, and early surgical consultation. Time is critical to prevent infection and preserve limb function.
- Critical Steps:
- Hemorrhage: Direct pressure, tourniquet if needed.
- Antibiotics: IV, broad-spectrum immediately.
⭐ Administer first dose of IV antibiotics within 1 hour of injury. Delays significantly ↑ infection rates.
- Wound: Remove gross contaminants, copious sterile saline irrigation (6-9L for high-grade), sterile moist dressing. Avoid direct antiseptic wound instillation.
- Tetanus: Administer toxoid +/- immunoglobulin.
- Neurovascular: Document meticulously pre/post reduction/splinting.
- Immobilization: Splint adequately to reduce pain and secondary injury.
Surgical Strategy - Fix & Cover
- Principle: Stable fracture fixation + Viable soft tissue envelope. "Fix & Flap".
- Timing:
- Definitive Fixation: Early, if patient/wound allows.
- Soft Tissue Cover: Crucial within 72 hours - 7 days.
⭐ Early flap coverage (<72h to 7 days) for Gustilo IIIB/IIIC ↓ infection, ↑ limb salvage.
- Fixation:
- External Fixators: Severe contamination, polytrauma, bone loss. Temporary/Definitive.
- Internal (IMN/Plates): Definitive stability if soft tissues permit.
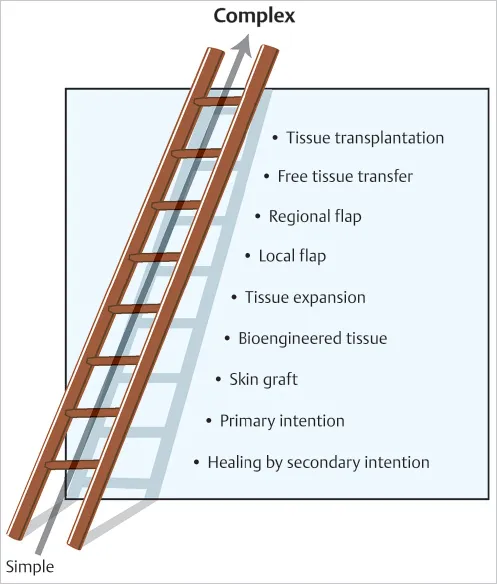
- Coverage (Reconstructive Ladder):
- Primary Closure/SSG: Gustilo I/II, clean bed.
- Local Flaps: e.g., Gastrocnemius, Soleus for tibial defects.
- Free Flaps: e.g., Latissimus Dorsi, ALT for large/complex defects.
- Approach: Ortho-plastic team essential.
Complications - Dodging Dangers
- Early Complications:
- Infection: Most common & feared. Risk ↑ with Gustilo grade. Prophylactic antibiotics are key.
- Compartment Syndrome: ⚠️ Surgical emergency! Severe pain, tense compartment. Requires immediate fasciotomy.
- Neurovascular Injury: Document pre & post-reduction.
- Gas Gangrene (Clostridial myonecrosis): Rare but life-threatening. Crepitus, foul discharge. Aggressive debridement.
- Thromboembolism (DVT/PE).
- Late Complications:
- Chronic Osteomyelitis: Persistent infection, sequestra formation.
- Nonunion/Delayed Union: Factors: infection, instability, poor vascularity.
- Malunion: Healed with deformity.
- Joint Stiffness/Arthritis.
- Complex Regional Pain Syndrome (CRPS).
- Amputation.

⭐ The most common organism causing infection in open fractures is Staphylococcus aureus (early) and Pseudomonas aeruginosa (late/nosocomial).
High‑Yield Points - ⚡ Biggest Takeaways
- Gustilo-Anderson classification is critical for management and prognosis.
- Administer IV antibiotics (Cefazolin; add Gentamicin for Type III) and tetanus prophylaxis immediately.
- Urgent, thorough surgical debridement is key to prevent infection.
- External fixation is often the choice for severe Type III fractures.
- Employ delayed primary closure or staged procedures for contaminated wounds.
- Major risks include infection (osteomyelitis), nonunion, and compartment syndrome.
- Add Penicillin for farm/soil contamination to cover Clostridium.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

