Spondylolisthesis - Slippery Spine Secrets
- Anterior vertebral slip, one vertebra over another. Most common: L5-S1, then L4-L5.
- Wiltse Classification (Types):
- I: Dysplastic (Congenital)
- II: Isthmic (Pars defect) - Most common overall
- III: Degenerative (Elderly, L4-L5 common)
- IV: Traumatic (Non-pars fracture)
- V: Pathologic
- VI: Iatrogenic/Post-surgical
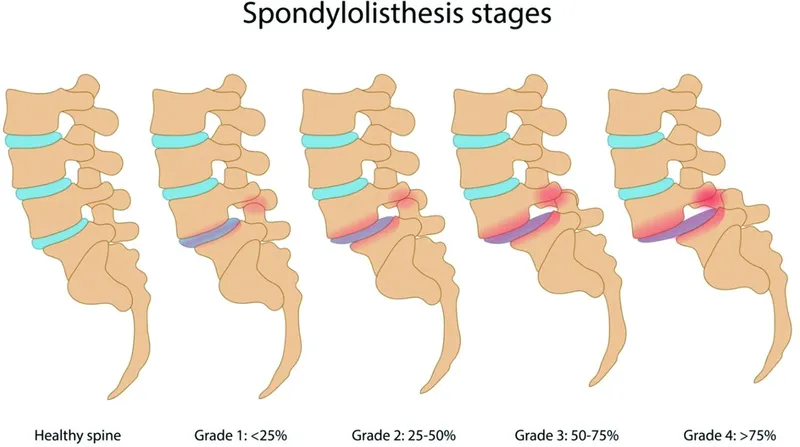
- Meyerding Grading (% slip):
- Grade I: 0-25%
- Grade II: 26-50%
- Grade III: 51-75%
- Grade IV: 76-100%
- Grade V: Spondyloptosis (>100%)
- Sx: Low back pain, radiculopathy, palpable "step-off".
- Dx: Lateral X-ray (grading); Oblique X-ray (Scottie dog for pars defect).
⭐ Isthmic spondylolisthesis (Type IIA - lytic) is the most common type in adolescents.
Spondylolisthesis - Why Vertebrae Wander
- Dysplastic (Type I): Congenital facet/sacral anomalies predisposing to slip.
- Isthmic (Type II): Defect in pars interarticularis (spondylolysis).
- Most common; often L5-S1 in young athletes (stress fracture).
- Degenerative (Type III): Facet joint arthritis & ligamentous instability.
- Common in elderly, typically L4-L5; no pars defect.
- Traumatic (Type IV): Acute fracture in posterior elements (not pars).
- Pathological (Type V): Bone disease (e.g., tumor, Paget's) weakening vertebral structures.
- Iatrogenic (Type VI): Post-surgical destabilization.
⭐ Isthmic spondylolisthesis (Type II) is the most frequent type, often resulting from stress fractures of the pars interarticularis in adolescent athletes, especially at L5-S1 due to hyperextension activities.
Spondylolisthesis - Decoding the Discomfort
- Forward slip of one vertebra over another. Most common: L5-S1.
- Types: Isthmic (pars defect, commonest), Degenerative, Dysplastic, Traumatic, Pathologic.
- Meyerding Grades: 1 (<25%), 2 (25-50%), 3 (50-75%), 4 (75-100%), 5 (>100% Spondyloptosis).
- Symptoms: Low back pain (↑ extension), radiculopathy, hamstring tightness. Palpable step-off.
- Diagnosis: X-ray (lateral, oblique for "Scottie dog" sign in isthmic). CT/MRI.
⭐ Isthmic spondylolisthesis is most common at L5-S1 due to a pars interarticularis defect.
- Treatment: Conservative (rest, physio); Surgery (decompression, fusion) for instability/neuro deficits_._
Spondylolisthesis - Spotting the Slip
- Diagnosis:
- Standing lateral X-ray: Essential for diagnosis, grading slip percentage. Dynamic views (flexion-extension) assess stability.
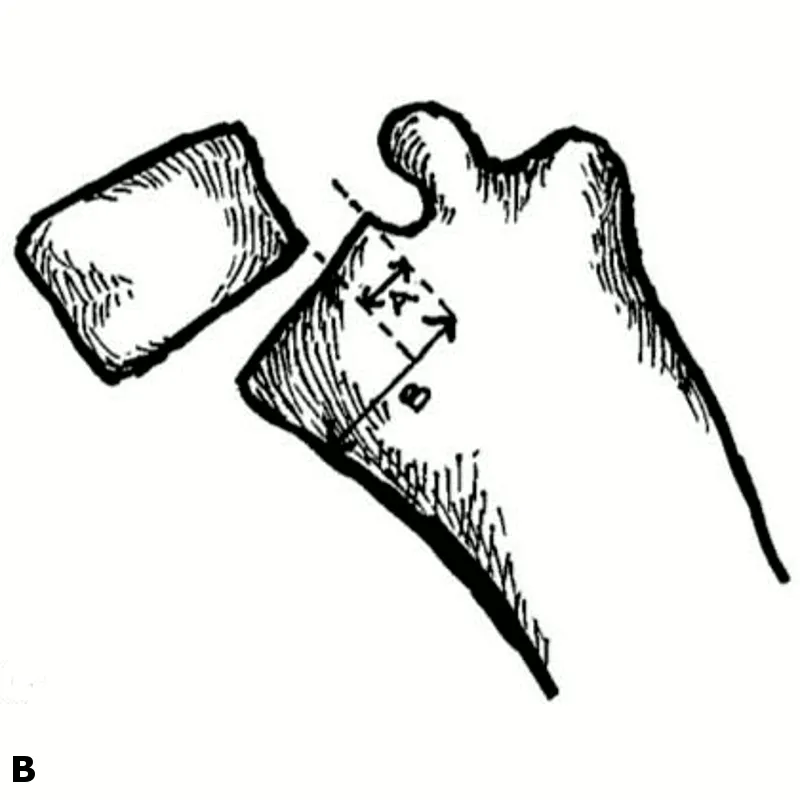
- Oblique X-ray: "Scottie dog" sign (collar fracture) reveals pars interarticularis defect (spondylolysis).
- CT scan: Superior for bony detail, confirming pars defect, pre-op planning.
- MRI: Evaluates soft tissues: disc integrity, nerve root compression, canal stenosis.
- Meyerding Classification (Anterior vertebral body slippage on lateral view):
- Grade I: 0-25%
- Grade II: 26-50%
- Grade III: 51-75%
- Grade IV: 76-100%
- Grade V (Spondyloptosis): >100% slip.
⭐ Isthmic spondylolisthesis at L5-S1 is the most common type and level, often seen in adolescent athletes.
Spondylolisthesis - Taming the Tilt
Forward slip of one vertebra over another. 📌 Types (DID TP): Dysplastic (congenital), Isthmic (pars defect, L5-S1 common, most frequent in <50y), Degenerative (L4-L5 common, >50y), Traumatic, Pathologic. Meyerding Grading (% slip):
- I: 0-25%
- II: 26-50%
- III: 51-75%
- IV: 76-100%
- V: >100% (spondyloptosis) Symptoms: Low back pain, radiculopathy, neurogenic claudication, hamstring tightness.
⭐ "Scotty dog" with a collar (fractured neck) on oblique X-ray indicates pars interarticularis defect (spondylolysis), key for isthmic type.
Management:
High‑Yield Points - ⚡ Biggest Takeaways
- Spondylolisthesis: Forward slippage of one vertebra over the one below.
- Most common is Isthmic type at L5-S1, due to pars interarticularis defect.
- Meyerding classification (Grade I-V) quantifies slip percentage.
- Key symptoms: Low back pain, radiculopathy, neurogenic claudication, hamstring tightness.
- "Scotty dog" sign on oblique X-ray suggests pars defect.
- Lateral X-rays are essential for diagnosis and grading.
- Treatment: Conservative for low grades; surgery for high grades or neuro deficits.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


